Maintaining the right balance between rest and exercise is very important for patients with rheumatoid arthritis. During an exacerbation of the disease, it is possible to continue playing sports, but the intensity of exercise should be reduced.
- Osteopathy is effective in treating joints
- Types, structure and function of joints
- General information
- Mechanism and causes of arthritis
- Types of joints
- types of pain
- What is the risk of this disease?
- Stages of acute arthritis
- Clinical forms of acute arthritis
- Traumatic acute arthritis
- Acute purulent arthritis (non-specific)
- symptoms
- causes
- All doctors who treat ankle pain 424
- Advice before an orthopedic appointment
- Diagnosis of ankle pain
- Moscow orthopedists – opinions
- Causes of Arthritis
- Symptoms of inflammatory arthritis
- Symptoms of arthritis
- arthritis in children
- Diagnosis of heel pain
- Treatment methods for heel pain
- heel spur
- bursitis
- Haglund's deformity
Osteopathy is effective in treating joints
Joint and periarticular soft tissue diseases belong to the group of musculoskeletal diseases. They can occur at any age and are one of the three most common causes for treatment. Pain, inflammation and reduced mobility are the top complaints patients hear from their doctor as they impact their lifestyle and reduce their quality of life.
In this article, the doctors at the Quality of Life Clinic explain the causes and triggers of joint pain. You will learn how to prevent joint pain and who to contact for treatment.
Types, structure and function of joints
The causes, mechanisms and treatment of joint diseases can be better understood by knowing the peculiarities of their structure and function.
Joints are connections between bones that give the body mobility. Bending the body, turning the head, stretching the arms and legs in and out - without joints, all movements of our body are impossible. They also provide support and help maintain balance.
Injuries to the joints impair the important support and movement function in space, significantly restrict mobility and are therefore psychologically difficult to cope with.
The movement of the joints is made possible by their structure. The bones that make up a joint are constantly rubbing against each other. To prevent them from damaging each other, their ends are covered with hyaline cartilage. This forms the joint surface on which the bones can move gently against each other.
In addition to the articular surface, the joints have:
– a joint space – this can contain articular discs and meniscus;
– Joint capsule – protects the joint from damage;
– Synovial membrane and synovial fluid – nourish and lubricate the joint;
– Ligaments – limit the range of motion;
– Periarticular nerves, vessels, muscles – nourish, strengthen and protect the joint.
All these formations provide ease of movement, amplitude and cushioning and protect against overloads. Therefore, their loss under pathological influences also impairs the function of the joint.
– Simple joints consist of two surfaces, meaning they are formed by two bones. For example, like a finger.
– Complex joints – consist of three or more surfaces. For example the elbow.
– Complexes – contain an intervertebral disc or meniscus. Example: the knee.
– Combined – contains several separate joints. For example the jaw joint.
General information
The disease affects tissues that are subjected to constant stress: the small joints of the hands and the metatarsals of the feet, the hip and knee joints, areas of the cervical and thoracic spine and, somewhat less commonly, the ankle and shoulder joints.
Tip! Aphakia of the interphalangeal joints of the hands occurs ten times more often in women than in men.
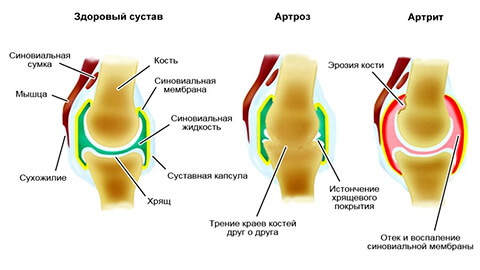
In many Western countries the term 'osteoarthritis' is not used but is replaced by the term 'arthritis'. This replacement is justified because in most cases arthritis is preceded or accompanied by inflammatory processes. In national medicine, the terms 'osteoarthritis' and 'arthritis' denote essentially the same disease, but with a different etiology of the process. In addition, the terms osteoarthritis, osteoarthritis and deforming osteoarthritis are used to describe the pathology.
Please note this! The difference between arthritis and osteoarthritis lies in the cause of the disease. In the first case it is an inflammatory process (the suffix -it means inflammation), in the second case it is a metabolic disorder (protein, minerals).
Mechanism and causes of arthritis
The main cause of arthritis is an imbalance in the formation and breakdown processes in cartilage and bone tissue. While in the normal state the synthesis processes predominate, in degenerative changes the destruction processes occur more quickly. The result is rapid aging and degeneration of the tissue structures. They begin to disintegrate first at the cellular level and then at the level of organ tissues. The first destructive changes occur:
The cartilage loses its natural elasticity and density and is no longer able to act as a shock absorber for movement. The mutual congruence of the shape of the articular surfaces is disrupted, which leads to deformation of the joint. This aggravates the development of pathological changes and sets in motion a number of irreversible processes. The bone tissue replaces the lost cartilage and begins to grow. Jags and protrusions form that limit mobility and can lead to serious disabilities later in life.
- Abnormalities in mineral metabolism can lead to gout-like joint changes, osteoporosis, etc.
- Poor tissue nutrition – venous stasis and poor microcirculation slow blood and lymphatic drainage. The mineral composition of bones is depleted, they become osteoporotic and lose their ability to regenerate. This phenomenon is characterized by lack of exercise, vascular abnormalities and hormonal disorders.
- Inflammatory processes – a consequence of acute infectious diseases, hypothermia, hormonal disorders.
- Autoimmune reactions – chronic inflammation, nervous stress, endocrine disorders and other causes can trigger aggression by the body's immune system against its own cells, including joint tissues. The most common autoimmune diseases are rheumatoid arthritis, scleroderma and lupus erythematosus.
- Increased joint wear - a mismatch between functionality and workload slows down synthesis and accelerates breakdown. This phenomenon occurs in athletes, dancers, overweight people and anyone who performs strenuous physical work or is subjected to long periods of static stress (standing work).
- Injuries such as bruises, sprains, fractures, puncture wounds and cuts disrupt the tissue structure and lead to deformation.
- Genetic diseases such as connective tissue dysplasia and disorders of collagen synthesis lead to an unstable, dysfunctional joint from the outset.
Types of joints
In anatomy, joints are differentiated according to the number of surfaces and their shape. In the groups that correspond to the individual shapes, the joint connections are differentiated according to their function.
Joints can also be divided into two levels by menisci: these are called complex joints. The movement can occur on one level or across the entire joint.
- Simple – two faces (shoulder);
- complex – three or more surfaces (elbow, wrist);
- complex (knee);
- non-complex (distal radioulnar joint).
They come in single, dual and multi-axis forms. This also includes combination joints, in which several joints are involved in the movement (temporomandibular joint).
types of pain
Joint pain varies depending on the disease. For example, you begin to hurt with a cold, while with an injury the symptom is sharp and intense. A more precise characterization depends on the diagnosis.
Depending on the trigger to which the bone movement joints react with pain, rheumatologists differentiate between these types:
- Mechanically. Joint pain is triggered by external factors: stress, trauma, dystrophic changes.
- Outbreak. If a person has been resting for a long time, the first movements cause discomfort. This is most commonly seen in the joints of the legs and hands.
- Inflammation. Arthritis can affect any area of the body, both during movement and at rest.
- Nocturnal. They occur when a person remains immobile.
Reflex pain is particularly worthy of mention. Although their origin is in the joints, they can be felt in unexpected places. Subjectively, muscles, neighboring organs and even the skin may hurt.
What is the risk of this disease?
The aseptic inflammatory process can subside spontaneously, but if it is accompanied by infection, a severe course of the disease with numerous complications and joint deformities is possible.
Stages of acute arthritis
Stages of Acute Serous Uncomplicated Arthritis:
- Initially – Inflammation and swelling of the synovial membrane and accumulation of serous contents in the joint cavity. The skin over the joint is swollen, red, and painful (moderate to severe);
- Developed – Worsening of all inflammatory symptoms without significant destruction of the joint tissue. However, there is destruction at the cellular level. The pain increases and the limb becomes difficult to bend;
- Restorative – gradual resolution of the acute inflammation and risk of hypertrophy of the connective tissue in the joint, leading to joint dysfunction. Therefore, proper rehabilitation is very important.
- Initially – Pus appears in the joint cavity but does not yet destroy the joint. Symptoms: Fever, swelling and pain, moving limbs is painful. X-rays show expansion of the joint cavity, which is due to an increased volume of pus. The surrounding tissue may be unchanged, but sometimes pustules form around the joint and the patient's condition worsens dramatically.
- Magnified – The soft tissues inside the joint are destroyed: synovial membrane, ligaments, muscle tendons. The limb is immobile and suffers from severe pain. This stage can occur with or without damage to the periarticular tissue.
- destruction – The cartilage covering the joint and the underlying bone are destroyed. Radiographs show focal destruction of cartilage and bone and narrowing of the joint stroma. Destruction can occur without penetration of pus into the surrounding tissue, with the formation of abscesses and cellulitis, or with penetration of pus to the surface of the body and the formation of a fistula.
- Ultimately – With timely treatment, it is possible to stop the purulent inflammatory process at any stage. Depending on the degree of joint deterioration, complete healing or partial loss of joint function may occur.
Clinical forms of acute arthritis
Which chondroprotectors to choose, how effective are they?
Each type of arthritis has clinical symptoms that it shares with other types, as well as its own characteristics.
Traumatic acute arthritis
Even minor trauma and overload damage the cells in the synovial lining; in response, they produce active substances (prostaglandins, cytokines) that maintain inflammation. In most cases of closed injuries, the arthritis is aseptic and manifests itself as mild swelling and pain in the joint. However, infection can enter the joint cavity. This happens with open wounds or when blood flows in from distant sources of infection, e.g. B. from ENT organs (tonsillitis, maxillitis), caries, etc., leading to the development of acute nonspecific arthritis, including purulent arthritis.
Aseptic inflammation can resolve spontaneously and without sequelae, but sometimes lesions remain that lead to impairment of joint function. Therefore, the disease should be treated under medical supervision, followed by rehabilitation.
Acute purulent arthritis (non-specific)
The occurrence of a nonspecific infection (pathogenic and opportunistic - constantly in the human body) in any type of arthritis leads to an aggravation of the general condition. The arthritis can be either serous or purulent. In serous (non-suppurative) arthritis, there is a slight increase in body temperature, redness and swelling of the periarticular tissue. If antibiotic therapy is carried out, the disease ends with a complete cure. If left untreated, it can eventually progress to a purulent process.
Purulent arthritis is a serious general illness with high fever, chills, headaches and malaise. At the same time, the affected area becomes red and swollen, with severe pain and the inability to move the limbs.
symptoms
Hairdressers, salespeople, drivers and computer programmers are the most common patients who ask whether arthrosis in the limbs can be cured. These people spend a lot of time standing, sitting at the computer or driving a car. Dancers, loaders, construction workers and athletes also put a lot of strain on their joints. One of the first symptoms of osteoarthritis is pain and a characteristic clicking sound that occurs when you try to move a limb. The symptoms often spread to other areas. When the weather changes, patients often notice a worsening of the pain. Swelling or swelling may occur around the joint. In advanced stages, bone deformities become visible.
causes
There are various causes of osteoarthritis. They can be caused by local pathological processes or by systemic diseases. The most common causes of osteoarthritis include:
- circulatory disorders;
- diabetes and other endocrine disorders;
- varicose veins;
- High blood pressure;
- Arteriosclerosis;
- Injuries, dislocations, fractures;
- high age;
- inflammation of the joints;
- mineral deficiency in the body;
- Psoriasis;
- bad posture;
- arthritis and synovitis;
- overweight;
- previous joint operations;
- frequent hypothermia.
All doctors who treat ankle pain 424
Choose an appointment online from metro stations: Yugo-Zapadnaya Prospekt Vernadskogo
Advice before an orthopedic appointment

Orthopedists diagnose, prevent and treat congenital and acquired deformities of the musculoskeletal system, including the effects of trauma. There are pediatric orthopedists and adult orthopedists. For children, examinations by an orthopedist are recommended as a preventative measure: at the ages of 1, 3 and 9 months and annually thereafter.
There are no special preparations for a visit to the orthopedist. You should shower hygienically and wear clothes that you can easily remove during the examination. It is very important that you bring any scans and CT scans you have previously taken with you.
Diagnosis of ankle pain
Your doctor will tell you what diagnosis you need to undergo. He can recommend the following:
- An x-ray of the spine.
- X-ray of the foot or hand
- X-ray of the extremities
- CT scan of the foot or hand
- Functional diagnostics Electroneuromyography (ENMG).
Moscow orthopedists – opinions
I have positive impressions of this consultation. The doctor explained everything to me in detail and showed me everything in detail. She recommended what I should do next regarding my problem. Everything happened slowly. She answered any questions that came up. She was very trustworthy and I would probably go to her again. She was attentive and friendly. You can tell she has a lot of experience and professionalism.
Competent and attentive doctor. The doctor listened carefully and recommended additional examinations. He made a preliminary diagnosis and prescribed medication to help in the initial stages. I will see this specialist again.
The doctor is very accommodating. He examined me thoroughly, answered my questions and prescribed me medication. He left a good impression!
He was recommended to me by a friend. I went to the doctor because of knee pain. I liked the reception. The doctor was young, but very competent. I have gone through all the diagnostics and will start treatment.
The doctor was attentive and friendly and I enjoyed everything about my visit. The doctor answered all my questions and now I'm wondering whether I should have surgery or not.
Everything was in order. The doctor examined me, gave me an injection and prescribed treatment. She is courteous and professional.
A very attentive and friendly doctor who I trust. He explained everything I needed to know about the problem and gave me advice that helped me. I'm very satisfied!
I went to the orthopedist to get help choosing shoes and insoles for my flat feet. The doctor gave me very detailed advice and helped me a lot; I can now walk in comfortable shoes without any discomfort.
The doctor was great and was very attentive to the patients. The doctor examined my foot, reviewed all the x-rays, explained the treatment and prescribed ointments. He treated me very well and it was a great honor and pleasure to be in his office. I am forever satisfied. I would recommend him to everyone I know.
Causes of Arthritis

The main causes of the disease are injuries, infections and metabolic disorders, which lead to poor nutrition of the joints.
Factors that increase the risk of occurrence:
- Genetic predisposition (only in women);
- Excessive strain on the joints (e.g. through sport);
- infectious diseases;
- caffeine abuse;
- Smoking;
- overweight.
Pathological changes in the joints can be accompanied by damage to the articular cartilage that covers the bones at their junctions. This type of disease is characteristic of degenerative arthritisOsteoarthritis is another group of degenerative joint diseases, of which traumatic arthritis and osteoarthritis are the most common.
Another group of osteoarthritis can be divided into: inflammatory arthritis. These diseases are associated with inflammation of the synovial membrane, which lines the joint capsule from the inside. Inflammatory arthritis is most commonly referred to as osteoarthritis:

Symptoms of inflammatory arthritis
Infectious arthritis usually involves the typical symptoms of an infectious disease, such as fever, pain and chills. In any case, the main source of complaint is the affected joint. The main symptoms are as follows:
Pain in the affected joint may occur with weight bearing (when moving) or at the end of the night. In the morning there is often stiffness (limited movement) in the affected joint. Then, as the day progresses, the person 'walks', mobility is restored and the pain disappears or decreases. In acute arthritis, joint pain can be constant. In chronic arthritis, the severity of symptoms gradually increases.
Symptoms of arthritis
There are many different symptoms of arthritis. Depending on the type of arthritis you have, symptoms may vary. However, the most common arthritis symptoms include:
- Pain, increased tenderness in the joints and stiffness in movement;
- Inflammation of the joint and adjacent tissues;
- limited joint mobility;
- fever and redness of the skin around the joint;
- Muscle weakness and wasting.
arthritis in children
Although arthritis is more common in older people, it can sometimes occur in children as well. In Russia, more than 20,000 children under 18 suffer from arthritis. Most types of arthritis that occur in children are classified as juvenile idiopathic arthritis (JIA). JIA causes pain and inflammation in one or more joints for at least six weeks. Although the exact cause of JIA is not known, symptoms often disappear with age and sufferers return to normal lives. The main types of JIA are described below.
Oligodynamic JIA (oligoarticular JIA) is the most common form of the disease. It affects the function of up to four joints in the body, most commonly the knees, ankles and wrists. Oligoarticular JIA is well tolerated and rarely causes complications. However, children are at risk of visual complications. To avoid this, it is important to have your eyes examined regularly by an ophthalmologist.
Polyarticular JIA or polyarthritis affects five or more joints. The disease can occur at any age in childhood. The symptoms of polyarticular JIA are similar to those of rheumatoid arthritis in adults. The disease is often accompanied by a skin rash and an increase in body temperature (fever) to 38°C or more.
Systemic JIA begins with symptoms such as fever, rash, lethargy (fatigue), and enlarged tonsils. These symptoms may later be accompanied by swelling and arthritis. Like polyarticular JIA, systemic JIA can occur in children of any age.
Enthesopathic JIA (JIA) is a form of juvenile arthritis that occurs more commonly in older boys and teenagers. It can cause pain in the soles of the feet and around the knee and hip joints where the ligaments attach to the bones.
Diagnosis of heel pain
When you go to the doctor, you will be examined according to a set schedule. The doctor will ask you in detail about your symptoms, explain the type, extent and location of your pain and examine the affected area. If necessary, he will order a series of laboratory and instrumental tests. This includes:
- A general blood test. It is important to detect the inflammatory process, a decrease in hemoglobin in anemia and changes in platelets in coagulation problems.
- Blood chemistry. It indicates changes in metabolism and helps detect diabetic changes, rheumatic and gouty arthritis, and infections caused by pathogenic streptococci.
- Marker test. This is necessary if bone tumors are suspected.
- Herbal examination of purulent secretions for flora. Required in the presence of purulent lesions, selection of antimicrobial drugs.
- X-ray examination of the bones and soft tissues of the foot. Helps to diagnose unexplained heel pain, including after trauma, against the background of degenerative processes.
- Ultrasound for arthritis, bursitis, neuroma, tunnel syndrome and localization of inflammation.
- Puncture of bone or synovial membrane if infections or tumors are suspected.
- CT or MRI scan to accurately diagnose damage to structures in the foot and heel area.
Treatment methods for heel pain
When pathologies occur in the heel area, attempts are made to treat them conservatively, but this is not always possible. If conservative treatment is ineffective, this is an indication for surgery. Surgical treatment eliminates the cause of heel pain quickly and permanently. Modern surgery is based on minimally invasive, outpatient techniques with minimal trauma and short recovery time.
heel spur
Surgical treatment of heel spurs is indicated if conservative treatment is unsuccessful within 6 months. The types of surgical treatment for heel spurs are osteophyte removal and plantar fasciotomy.
These procedures are performed under local anesthesia. An endoscopic probe and microsurgical instruments are inserted by the surgeon through a small incision. Using micro camera guidance, he cuts out the bony process and, if necessary, the inflamed area of the fascia. The thick part of the adductor muscle of the big toe is cut so that the nerve is not compressed.
If the pain associated with heel spurs is caused not by an osteophyte but by excessive tension on the soleus tendon, a tenotomy - a partial division of the tendon - is performed. The procedure is carried out without an incision - through punctures with high-frequency electrical current (radiofrequency tenotomy).
bursitis
Bursectomy – the surgical removal of the synovial capsule – is indicated when conservative treatment of synovitis fails. The operation is performed without incision using an arthroscopic technique.
Microsurgical instruments and a miniature video camera are inserted into the joint through 2-3 punctures with a diameter of 4-5 mm. This is followed by dissection and removal of the joint capsule. The incisions are covered with a sterile dressing. The procedure takes about 30 minutes. The recovery time is 2 days.
Haglund's deformity
If Haglund deformity cannot be treated conservatively, surgery is indicated. During an endoscopic procedure - without incisions - the bony process is removed from the surface of the calcaneal tuberosity, followed by excision of the posterior capsule of the calcaneus. This procedure restores the mechanical function of the Achilles tendon and eliminates the cause of the pain.
Read more:- Which doctor treats the hip joints.
- Which doctor treats flat feet?.
- Which doctor treats adult posture?.
- Traumatology orthopedist which doctor.
- What kind of doctor treats the joints.
- What kind of doctor treats knee joints.
- Which doctor do you go to if you have joint problems?.
- Who treats the joints.
