Renal anomalies occur when the primary kidney is displaced from the pelvis to the lumbar region. The shape of the kidney is almost always changed and the gates open forward.
- Correction of distal closure
- Distal bite symptoms
- Intraoral manifestations
- External appearances
- Functional symptoms
- Application in human anatomy.
- Application in dentistry
- Causes of distal occlusion
- classification
- Classification and symptoms
- Diagnosis of distal motor neuropathy
- Our team
- Maxim Bessarab
- Artak Mikhaylovich Kharchyan
- Genrikh Olegovich Krasnov
- OUR LOCATION
- ABOUT US
- INFORMATION FOR PATIENTS
- CONTACT
- What is a Distal Bite?
- Causes of the development of the distal bite
- Get advice
- Distal occlusion symptoms
- Shape of the kidneys during ultrasound examination
- Video. Horseshoe kidney in ultrasound examination
- Echostructure of the kidney
- Video. Renal arch arteries on ultrasound examination
- Treatment of distal occlusion
- Prognosis and prevention of distal bite
Correction of distal closure
According to various studies, distal or prognathic occlusion is the most common dental malocclusion. It occurs in about 30 % of children and 15-20 % of adults with misaligned teeth.
Distal bite (distal occlusion) – is a jaw condition in which the upper jaw is bitten forward in relation to the lower jaw. A disproportionate bite can be caused by both overdevelopment of the upper jaw and underdevelopment of the lower jaw.
Distal bite symptoms
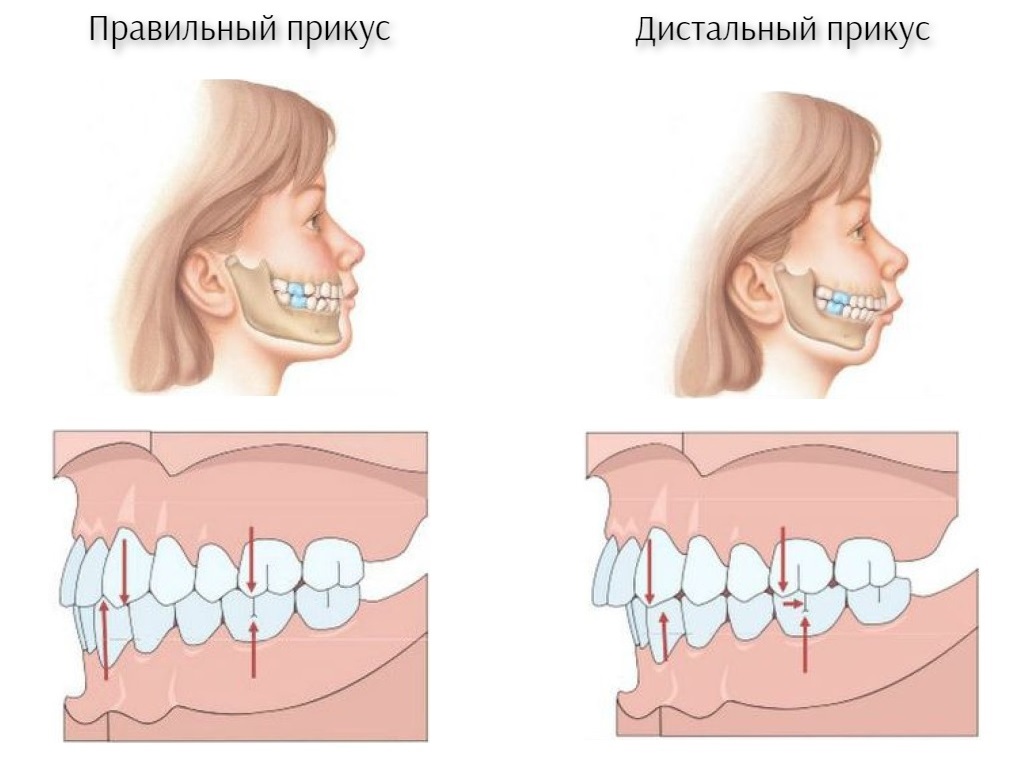
Distal bite is most easily recognized by the occlusion of the teeth. However, some occlusion anomalies affect the entire appearance: they shape facial features, facial expression, symmetry and affect posture.
Intraoral manifestations
In the oral cavity, the distal bite can be recognized by the fact that the upper front teeth protrude forward. In an orthognathic bite, the upper incisors overlap the lower ones by about 1/3. A distal bite results in a gap between the upper and lower incisors, called a sagittal gap.
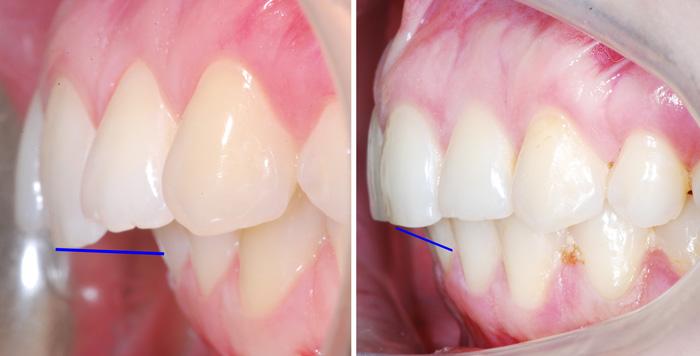
External appearances
Due to the disproportionate protrusion of the upper jaw, the distal bite can be recognized by a bulging or bird-like profile. The nose and upper lip protrude, the lower lip is sunken. The chin is sloping, disproportionately small, sometimes with a fold - a 'double chin'. With a pronounced distal bite (with a large sagittal fissure), the lips are not closed in a relaxed position and the mouth is always slightly open.
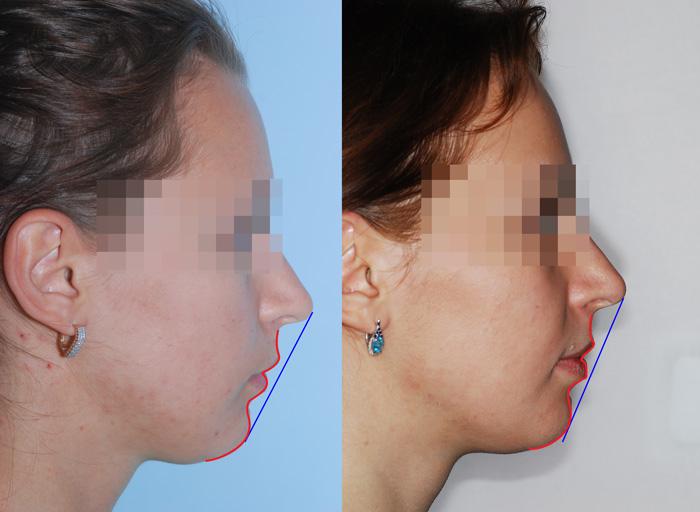
Profile before and after distal bite treatment
The distal bite is visually reflected in the posture - the whole body is slightly tilted forward. Distal occlusion is characterized by a pronounced curvature, an elongated, forward-leaning neck, and a protruding belly.
Functional symptoms
In addition to external symptoms, distal occlusion causes discomfort when swallowing, chewing, nasal breathing, and speaking.
However, occlusion anomalies usually develop gradually from childhood, so that the adult is more likely to adapt and not experience any discomfort.
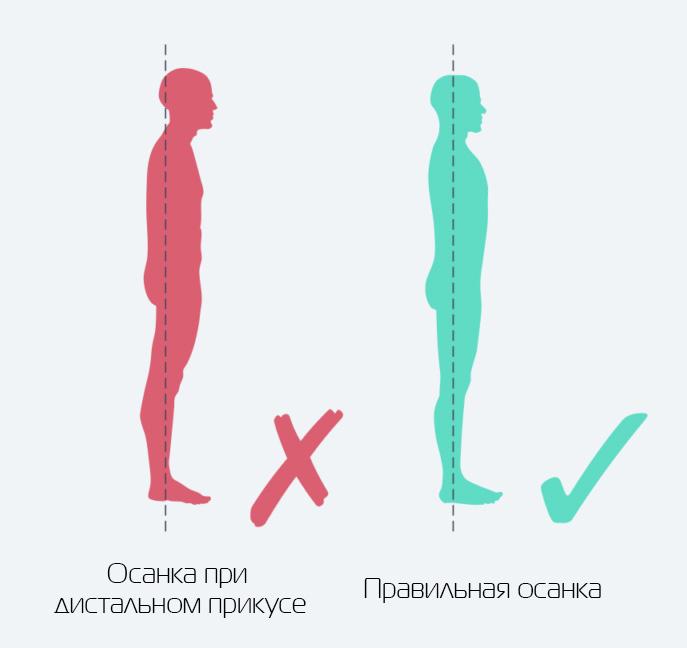
Application in human anatomy.
'Distal' and 'proximal' are terms that indicate where a particular anatomical unit is to be found or that are used to describe it. For example, the anatomical and surgical necks of the humerus, which are located at the proximal part of the bone (proximal), are called 'proximal anatomical formations'.
In addition to anatomical terminology, these terms are also used in clinic to denote pathological conditions:
- Syndromes: Distal Zudeck syndrome (pain in the lower limbs after trauma, accompanied by multiple abnormalities);
- Diseases: – Proximal duodenitis (inflammation of the part of the duodenum proximal to the stomach);
- Symptom of distal arthrogryposis (characteristic abnormal flexion of the joints of the hands and feet).
These concepts are widely applicable and used in teaching the fundamentals of normal and topographic anatomy and operative surgery to medical students.
For surgical protocols and subsequent analysis of typical surgical techniques, one can find a description of the direction of the suture along the wound indicating the location of the mass. For example, the location of bone tumors is described as follows: 'located on the proximal epiphysis of the humerus'.
Specific examples of the terms 'distal' and 'proximal'.
| Area | substance | Example |
| Anatomical Terminology | Explanation of the situation | Localization of the distal radiocarpal joints. |
| Definition of direction | Loss of cutaneous sensation extends distally; the food lump progresses from the proximal end of the esophagus to the distal end. | |
| Clinical Terminology | Explanation of the diagnostic signs | Symptom of distal attenuation. |
Application in dentistry
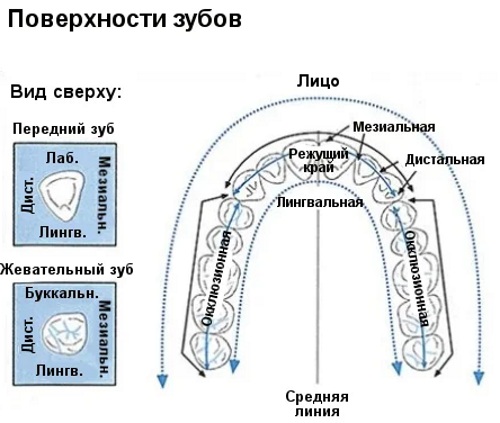
From the perspective of an average person looking at a row of teeth, the position of the teeth can be described as being 'side to' each other, or one tooth can be said to be 'in front' of the other.
To avoid confusion, it is common for dentists and oral surgeons to use the adjectives 'anterior' and 'posterior'. Even when two teeth meet as incisors, the position of the first incisor in relation to the second is called 'anterior'.
'Proximal' and 'distal' as terms to describe the position of a tooth do not describe the tooth itself, but rather its side surfaces or edges. The medial surface is that which faces the preceding (posterior) tooth. The distal surface is that which faces the preceding tooth.
Both terms are used to understand and discuss the treatment plan. The strategy of dental prosthetics and veneers includes a description of the manipulation of the distal and proximal tooth surfaces.
Causes of distal occlusion
It is important to know that in newborns, the lower jaw is usually 1-10 mm behind the upper jaw, resulting in a sagittal gap between the jaws. Later, during breastfeeding, teething, and chewing development, the lower jaw gradually returns to its normal position relative to the upper jaw, and the distal bite transitions to an orthognathic bite. This means that the distal bite is caused by an artificial diet that does not place much stress on the child during sucking and therefore does not stimulate the growth of the lower jaw.
Dental and occlusion abnormalities (including distal bite) are present in 60 % of children with rickets; 34 % of children with nasopharyngeal abnormalities (tonsils, chronic hypertrophic rhinitis, deviated septum, etc.) Bad habits such as prolonged sucking on pacifiers, fingers, toys and other foreign objects, and lip biting also negatively contribute to the formation of distal bite.
Other factors include calcium and fluoride deficiency, lack or insufficient solid food in the child's diet at a young age, early removal of baby teeth and missing dentures. In addition, distal bite can be caused by congenital jaw anomalies, birth trauma, jaw trauma, and posture abnormalities.
classification
In orthodontics, several classifications of distal bite have been proposed (according to E. Engl, AI Betelmann, FJ Distal bite in the dentist's mouth is primarily not a problem).
For example, E. Engl, who classified distal occlusion as Class II occlusion, distinguished 2 subclasses within this class:
- 1 subclass. – (1) fan-shaped inclination of the upper incisors, narrowing of the rows of teeth in the lateral areas
- 2 subclass – Palatal inclination of the upper central incisors; Deviation of the lateral incisors towards the lip and rotation around the axis; Absence of a sagittal gap between the upper and lower incisors
Betelmann distinguishes between several clinical variants of distal occlusion
- Upper macrognathia with normally developed lower jaw;
- Lower micrognathia with normally developed maxilla;
- Upper macrognathia in combination with lower micrognathia;
- Prognathism with lateral maxillary compression.
Based on the morphological changes revealed by the analysis of cephalometric images, Khoroshilkina distinguishes between gnathic, alveolar and combined forms of distal occlusion.
Classification and symptoms
According to many geneticists, the classification of the forms of this pathology is far from complete. The genes responsible for some forms of distal motor neuropathy have not yet been identified. In many cases the pathogenesis remains unclear. Therefore, all known forms of the disease are currently divided into autosomal dominant, autosomal recessive and taking into account sex-linked mechanisms of inheritance. Within these groups, different phenotypic subtypes of distal motor neuropathy with different clinical presentations are distinguished. These subtypes are named after the English terms hereditary motor neuropathy (HMN) or distal spinal muscular atrophy (DSMA). The most common variants of distal motor neuropathy are described below.
1. HMN – is a congenital form of distal motor neuropathy that occurs in newborns. It is characterized by a very slow progression and is inherited in an autosomal dominant manner. It is caused by defects in the TRPV4 gene, which is located on chromosome 12.
2. HMN2A – Distal motor neuropathy type 2A, autosomal dominant, caused by a mutation in the HSPB8 gene on chromosome 12 – its defects also cause another form of neuropathy, Charcot-Marie-Tooth syndrome. It occurs in adults and mainly affects the upper limbs. Slow onset of symptoms: muscle weakness, atrophy and abnormal sensitivity to vibration.
3. HMN2D – Distal motor neuropathy with predominantly lower limb involvement. Caused by a mutation in the FBXO38 gene, located on chromosome 5. The first symptoms usually appear in adolescence or adulthood. At the beginning of the disease, weakness is observed in the knees, which then develops into tremor in the lower limbs. In later stages of the disease, the shoulder muscles are also affected.
Diagnosis of distal motor neuropathy
The diagnosis of distal motor neuropathy can be made by examining the patient's family history, electroneuromyography, and molecular genetic testing. When examining a patient with almost any form of this disease, arm and/or leg muscle weakness and, in some cases, areflexia are noted. If distal motor neuropathy persists for a long time, muscle hypotrophy is noted, and in the severe form, atrophy of muscle tissue in the distal limbs. Anamnesis in some cases confirms similar changes in the patient's parents or other close relatives.
The pattern of electromyography (or electroneuromyography) can vary depending on the type of distal motor neuropathy and therefore the pathogenesis of the disease. For example, the DSMA1 type is characterized by a marked delay in nerve impulse fiber transmission, while the HMN5 form is typically normal, without the presence of a myocyte action potential. A biopsy of muscle tissue in the affected areas almost always shows signs of myocyte hypotrophy and heterogeneity. Molecular genetic diagnosis is only used for some forms of distal motor neuropathy (e.g. HMN2A, HMN, DSMA1). Prenatal diagnosis is possible and the material is obtained from a chorionic villus sample.
Our team

Maxim Bessarab
- md
- Specialist in arthroscopic and minimally traumatic joint and foot surgery
- Dr. Bessarab has extensive expertise in conservative
and surgical treatment of sports injuries. - He performs more than 500 arthroscopic surgeries a year.

Artak Mikhaylovich Kharchyan
- Orthopedic traumatologist of the highest category
- Candidate of Medical Sciences
- Head of department in a large city hospital in Moscow.
- Dr. Kharchyan is a leading specialist in joint arthroplasty and low trauma bone fractures in Russia.
- Dr. Kharchyan performs more than 400 operations per year, using the most modern technology.

Genrikh Olegovich Krasnov
- Traumatologist and orthopedic surgeon
- Member of the Russian Society of Traumatology and Orthopedics and the Russian Arthroscopic Society.
- Experienced in conservative and surgical methods of joint treatment.
- Specialized in orthopedic orthotics, shock wave therapy
- Performs up to 300 arthroscopic surgeries per year
OUR LOCATION

Monday - Friday: 7 a.m. to 8 p.m







ABOUT US
INFORMATION FOR PATIENTS
CONTACT





Orthopedic traumatologist Bessarab MS Orthopedic traumatologist Bessarab MS There are contraindications. Please consult a specialist. All rights reserved 2022 ©
What is a Distal Bite?
Distal bite is a fairly common problem. Studies show that 20 % of adults and 30 % of children are affected. The misalignment of teeth, in which the upper jaw protrudes beyond the lower jaw, not only causes aesthetic problems but also leads to serious health problems.
Occlusion abnormalities have a major impact on appearance. People who have a distal bite have irregular facial features. When the jaws come closer together, a sagittal fissure becomes visible.
Please note: A distal bite not only gives the face an irregular profile but also affects posture. The body involuntarily leans forward. A patient suffering from this pathology has a strong bend, an elongated neck and a protruding abdomen.
Causes of the development of the distal bite
Many different factors influence the development of the jawline. Many of them affect humans before birth. The most common causes of distal bite are:
- Genetics. Researchers have found that distal occlusion is a hereditary pathology in more than 60 percent of cases. Without early prevention, the problem can worsen. Parents should therefore deal with this immediately after the birth of their child. Especially if they have also been diagnosed with this disease.
- Peculiarities of fetal development. The unhealthy environment of the child's mother often leads to various fetal pathologies. The most dangerous factors include alcohol consumption, vitamin deficiency and radiation exposure.
- Special features related to breastfeeding. At birth, the position of the baby's jaw is not the same as in adulthood. During development it resembles the upper jaw. However, this is only the case if the child frequently uses the lower jaw when feeding. If you choose the wrong bottle (with a large opening for milk), the baby will move its mouth muscles less. This has an impact on the irregular development of the lower jaw.
- Illnesses in childhood. Misaligned teeth occur as a result of diseases such as sinus infections, catarrhs and other problems associated with abnormal breathing. Diseases such as rickets can also lead to this problem. Lack of calcium and other minerals is particularly acute at a young age.
Get advice
Answer all your questions before your appointment!
Distal bite is a characteristic dental anomaly located in the plane through which the sagittal axis passes. In this case, the upper jaw protrudes beyond the lower jaw and causes disruption of the closing process. This pathology is now widespread in childhood and adolescence, between 4 and 16 years of age.
When examining distal malocclusion and its causes, attention must first be paid to a discrepancy in the size and shape of the dental arches. It is the result of active development of the upper jaw bone and poor growth of the lower jaw bone.
It is an oral disorder in which the teeth in the anterior region do not bite together because the anterior region is too short or too long, and there is an abnormal bite in the posterior region. This is due to the narrowing of this area and the development of the mandibular area is impaired.
The development of this pathological process can be influenced by the following groups of factors.
- Endogenous factors, which include:
- The occurrence of diseases associated with abnormal functioning of the endocrine glands;
- heredity;
- Spontaneous anomalies during the development of the fetus in the uterus (alcohol consumption, insufficient intake of vitamins and minerals, medications, strong X-rays, the presence of concomitant diseases in the woman).
- Early extraction of baby teeth;
- Exposure to somatic diseases or trauma that may negatively impact dental development;
- diseases of the upper respiratory system;
- Abuse of tobacco, drugs or alcohol.
Distal occlusion symptoms
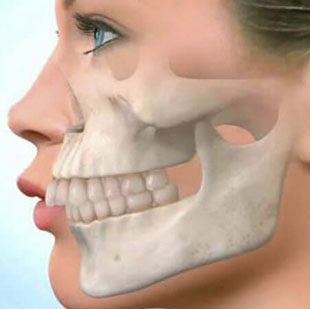
The most common symptoms include facial abnormalities caused by abnormal development of the neck muscles and musculoskeletal system. This leads to a disproportion of the face with pronounced recession of the lower lip. The disease can also be associated with excessive protrusion of the frontal incisors and abnormal tooth closure in the chewing zone.
Since this pathological process occurs in childhood, it may be associated with impaired swallowing and nasal breathing. The chewing muscles are not properly strengthened, which can gradually lead to a deterioration in the function of the temporomandibular joint and, as a result, destructive processes in the oral cavity.
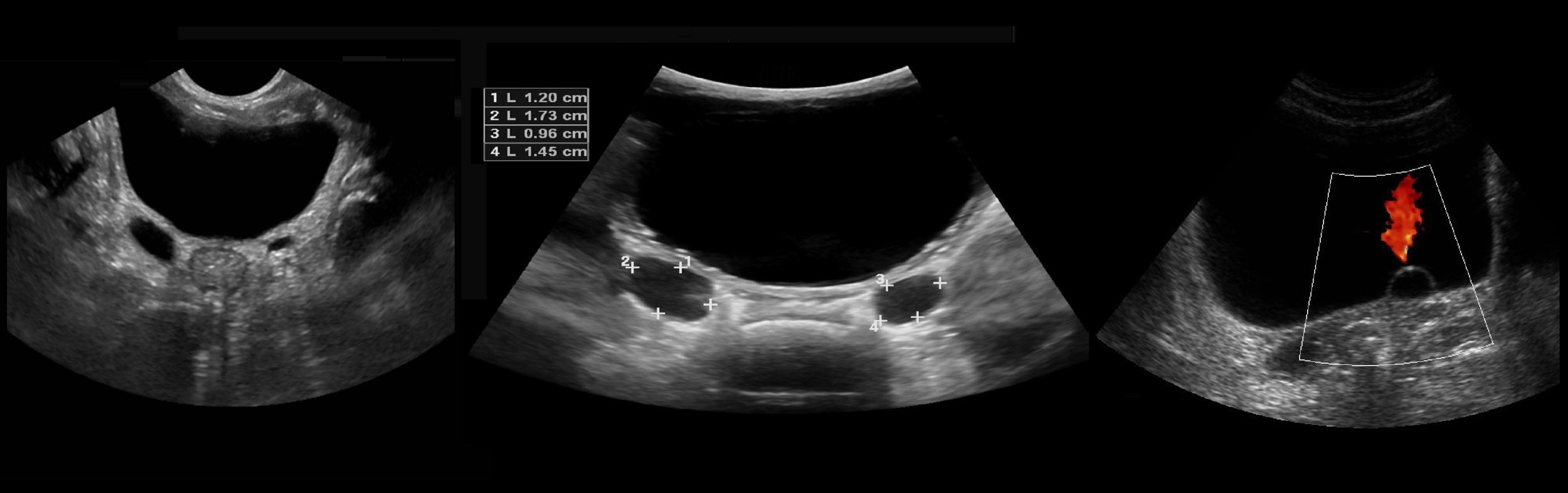
Shape of the kidneys during ultrasound examination
To view the upper pole of the kidney, ask the patient to take a deep breath. The shape of the kidney is bean-shaped - convex on the lateral side and concave on the medial side. The lower fetal kidney and the left cusp kidney are considered a variant of the normal.
Illustration. On the ultrasound (1) and the CT (2, 3) the outline of the kidney is wavy. In the embryo, the kidney develops from individual lobules that fuse together as they grow. The lobular structure of the kidney is clearly visible in the fetus and newborn and is occasionally preserved in adults.
Fig. A left cusp kidney is seen - a convex, irregular external outline caused by hypertrophy of the parenchyma in the middle third of the kidney. It is believed that the 'hump' in the fetus is caused by compression of the lower edge of the spleen.
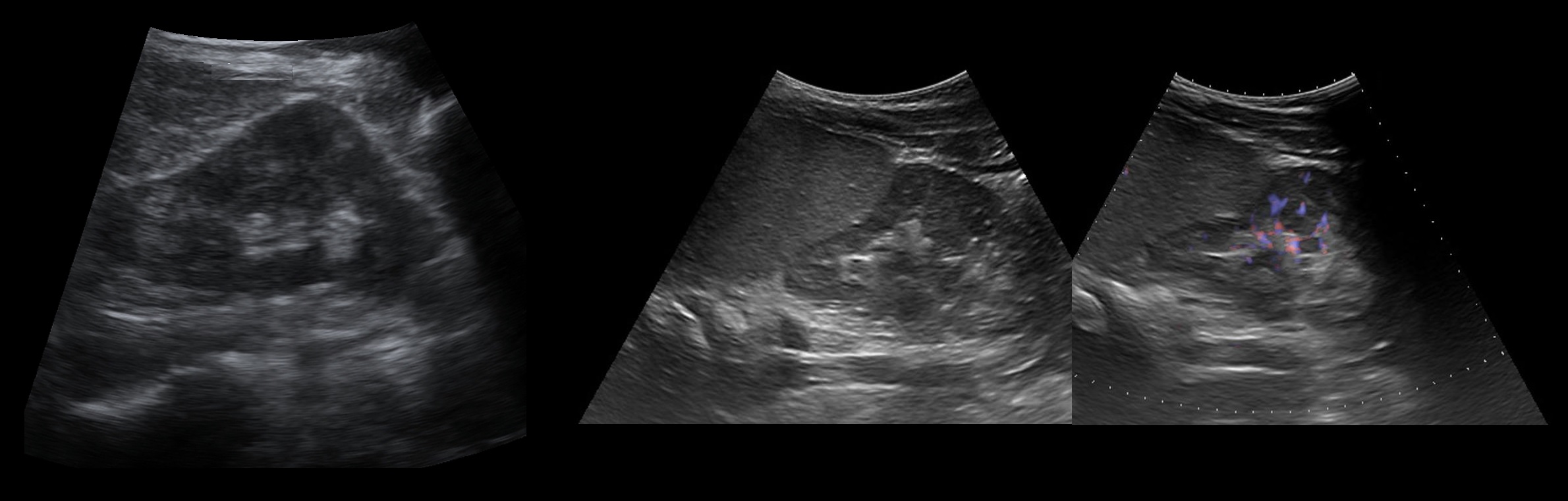
Illustration. Palpation from the anterior abdominal wall so as not to miss the isthmus between the kidneys. The isthmus in front of the spine is evidence of renal fusion - a horseshoe-shaped kidney. Variations on the anatomy of the horseshoe kidney can be found here.
Video. Horseshoe kidney in ultrasound examination
Echostructure of the kidney
In a normal kidney, the pyramids are hypoechoic, the cortical substance and the columns of Bertini are isoechoic relative to each other. The sinus normally contains invisible CHL, hyperechoic connective and fatty tissue, hypoechoic vessels, and pyramidal apexes.
If the pyramids, cortical substance and renal columns are highlighted, the echostructure of the renal parenchyma is unchanged. If they are not visible, the echo structure is altered due to the lack of clear cortical and cerebellar differentiation.
Illustration. Ultrasound shows a kidney with unchanged echo structure: cortical layer and Bertini columns hypoechoic in relation to the liver, pyramids almost hypoechoic, sinus hyperechoic.
Illustration. In 37 % of healthy newborns, the 'white pyramids' sign was discovered on ultrasound on the first day of life. Precipitation of Tamm-Horsfall protein and uric acid causes reversible tubular obstruction. At 6 weeks of age it passes without treatment.
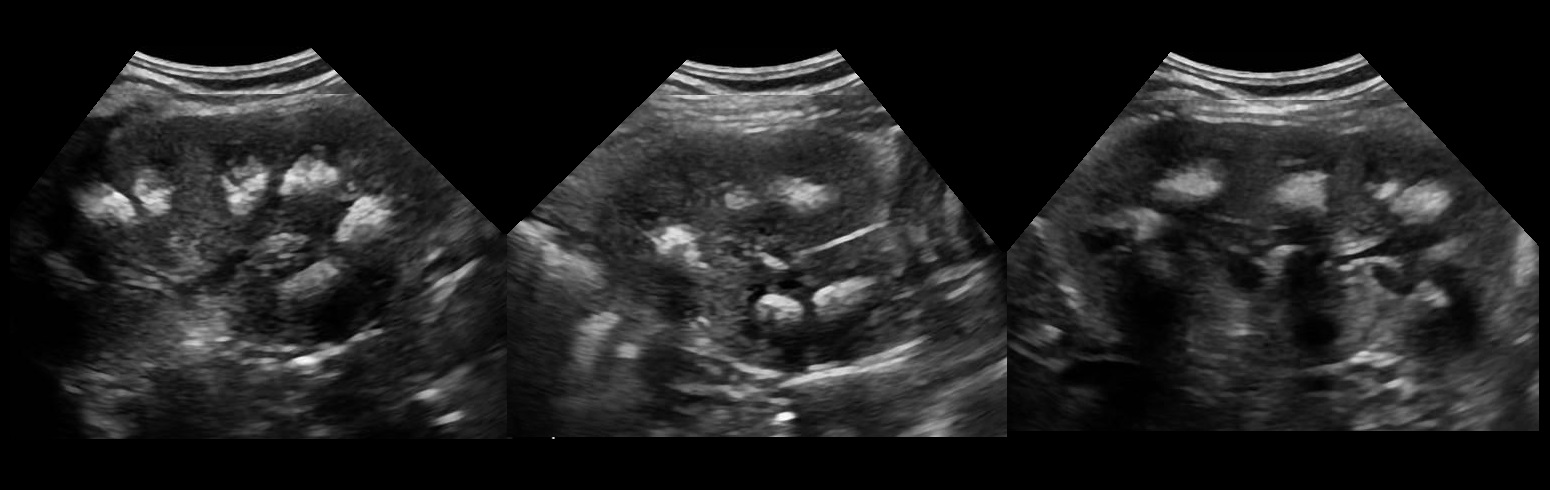
Illustration. On the ultrasound image of the healthy kidney, linear hyperechoic structures can be seen along the base of the pyramids (corticospinal junction) with a hypoechoic path in the middle. These are arch arteries that are mistaken for nephrocalcinosis or stones.
Video. Renal arch arteries on ultrasound examination
Illustration. On ultrasound, the lower pole of the kidney is separated by a hyperechoic fibrous bridge; the lower segment basin is 7 mm wide. This is a variant of the normal kidney structure. The kidney may be deformed so that its size and length are slightly less than in the opposite case. A slight enlargement of the renal pelvis below the erosion persists throughout life.
Treatment of distal occlusion
Distal bite, which can be treated at any age, is best corrected during childhood and adolescence. Ideally, the treatment should be carried out before the teeth change in infants.
In children, the goal of correction is to limit the growth of the upper jaw and promote the development of the lower jaw. For this purpose, removable orthodontic devices - plates - are used. There are several well-known models:
In addition to the plastic plates, other devices are often used: miobrace, trainer, LM-activator, etc. They are made of silicone and are effective, but only if the child's jaw is not yet developed.
Treatment may be accompanied by other measures:
- Selective teeth grinding;
- extraction of supernumerary teeth;
- myogymnastics;
- Preventing and avoiding bad oral habits;
- Normalization of nasal breathing when there are problems with the upper respiratory tract.
During the tooth change phase, other aids are used to correct the shape and alignment of the dental arches. Removable braces, but also palatal expansions, trainers, etc. can be used for this purpose.
Once the jaws are fully formed, the distal bite can only be corrected with fixed prosthetics. The most popular is orthodontic braces, the design of which consists of arches connected by special brackets. Thanks to the constant tension they create, the teeth move in the right direction. There are the following types of braces:
There are also vestibular and lingual versions - in the first case the brackets are attached to the outside of the teeth, in the second case inside.
How long the braces are worn depends on the severity of the misalignment, the condition of the bone, the patient's age and other factors. Once braces are fully in place, retainers are required, but they are worn for long periods of time and are designed to prevent the teeth from returning to their original position.
Prognosis and prevention of distal bite
The prognosis when treating distal bite is often good - especially if the treatment is ordered early enough by the orthodontist. But even if the correction begins only in adulthood, the chances of correcting the error are quite good if the doctor's recommendations are followed.
The prognosis for distal bite is unfavorable if not treated by a doctor as it causes a number of problems:
- Impairment of chewing and swallowing function - due to the reduction in the usable tooth surface, chewing performance is reduced, which leads to gastrointestinal diseases;
- Risk of periodontal disease – abnormal load distribution leads to damage to the posterior teeth;
- Dysfunction of the temporomandibular joints.
If the distal bite needs to be restored, it is very difficult because the upper and lower teeth are not fused together and in most cases there is asymmetry.
To prevent distal bite, the following guidelines should be followed:
- Breastfeeding and timely and complete introduction of solid food to the child;
- Prevention of rickets, vitamin and micronutrient deficiencies;
- Prevention and timely treatment of diseases of the nasopharynx that affect proper nasal breathing;
- Prevention of posture problems and diseases of the musculoskeletal system;
- Elimination of bad habits – sucking objects, pacifiers, finger sucking, etc.
If these recommendations are followed, distal bite can be prevented in most cases.
- Allergic stomatitis
- Dental anomalies
- Hyperesthesia of the tooth
- Hypertrophic gingivitis
- Enamel hypoplasia
- Dental dystopia
- Tartar
- dental plaque
- Oral candidiasis
- Catarrhal gingivitis
- Maxillary cysts
- Oral leukoplakia
- Mesial occlusion
- Malocclusion
- Periapical abscess
- periodontitis
- Sialadenosis
- Oral fibroma
- Chronic stomatitis
- Stomatitis
- Clubfoot correction in children.
- Podiatrist what kind of doctor.
- Medial and lateral side.
- Who is the orthopedist?.
- The flexion of the foot is.
- Long fibula muscle.
- rotation in anatomy.
- Syndrome of the tibial nerve.
