Relaxation exercises are used to combat fatigue and other neurological disorders. These exercises completely offset the effects of stressful situations.
- Lower Limb Ultrasound (Start)
- The jumper's knee in the ultrasound examination of the lower limbs
- General information
- 4+5 Triceps calf muscle? (triceps surae muscle).
- 4. Biceps calf muscle
- Treatment of calf pain
- prevention of pain
- clinical signs
- symptoms
- Benign curl-fasciculation syndrome
- Do benign fascioculations occur in a healthy person?
- As a preventive measure
- What to look out for
- Human Calf Muscle Anatomy Information:
- Which doctors you should go to for a calf muscle exam:
- Clinically Relevant Anatomy
- Epidemiology/Etiology
- What should I eat if I have cramps during pregnancy?
- Calf cramps in the first, second and third trimester of pregnancy and after childbirth
Lower Limb Ultrasound (Start)
Ultrasound lower limb injuries are common in athletes and affect the quadriceps tendon, which is commonly found in basketball or volleyball players. The injury occurs secondary to frequent, repetitive jumps, but can also be the result of severe bending caused by a quick jolt while running. Because the right quadriceps occupies two joints, it is the most commonly injured component of the lower limb. In the distal part of the thigh, the quadriceps tendon consists of three layers. The superficial layer arises from the rectus femoris muscle, the middle layer consists of the combined vastus medialis and vastus lateralis muscles, and the deep layer arises from the vastus intermedius muscle. While most of the tendons of the quadriceps femoris attach to the anterior superior region of the patella, the superficial fibers of the rectus muscle insert to the anterior surface of the patella and attach to the patellar tendon, known as the continuation of the anteromedial region of the quadriceps.

Tendinosis of the rectus muscle tendon is shown on lower limb ultrasound as a hypoechoic and possibly thickened tendon. Although thickening can be demonstrated with color Doppler, the term tendinosis is used instead of tendinitis because the thickening is due to neovascularization and not inflammation. Anechoic interlayers at the site of patellar enthesis are tears that can affect one, two, or all three layers. Full-thickness fractures commonly occur 1-2 cm proximal to the insertion site in the non-vascular zone. However, there may be a lower limb injury that ultrasound shows an area of cartilage irregularity or even an echogenic, retracted, and masked tendon tear. While the torn tendon is usually retracted (with wavy fibers visible on ultrasound), in uncertain or doubtful cases, dynamic maneuvers in which the leg is passively flexed and extended or in which the kneecap is manually moved downward show whether the proximal intact fibers move with the patella. Detachment of the continuation of the quadriceps anterior to the patella from the anterior cartilage of the patella with production of hypoechoic fluid is commonly noted in the management of anterior knee pain. An isolated rupture of the distal rectus femoris muscle can occur clinically with a delay and only show up much later after the injury as a palpable 'pseudotumor' in the form of a drawn-in tendon stump.
The jumper's knee in the ultrasound examination of the lower limbs
Patellar tendon tendinopathy that causes pain in the front of the knee is commonly referred to as 'jumper's knee'. It is similar to an injury to the quadriceps tendon and, as the name suggests, affects people who play sports that require repetitive jumping. There is no real inflammation of the tendon, which is why the term tendonitis is not appropriate. Conspicuous findings on ultrasonography include hypoechoic tendinosis, possible anechoic intertendinal tears, and hyperemia due to neovascularization, which correlate with the severity of the patient's symptoms. The deep segment of the proximal patellar tendon is most commonly affected.
A tear of the medial head of the calf muscle, known as 'tennis foot', most commonly affects middle-aged athletes who report acute metatarsal pain during active ankle flexion and simultaneous knee extension. Ultrasonography studies have shown that medial calf head tears occur most commonly at the distal musculotendinous junction and are more common than soleus tendon tears, which have previously been implicated as the clinical syndrome. When evaluating symptoms suspected on lower-limb ultrasound, an alternative diagnosis of deep vein thrombosis, which may also be associated with lower-limb symptoms, should be considered.
The medial head of the calf muscle is best assessed longitudinally. Ultrasound characterization of a calf muscle tear involves disruption of the normal alternating linear hyperechoic and hypoechoic layer at the distal muscle-tendon junction, where a collection of hypoechoic bubbles replaces the normal conical appearance of the distal aspect. Large tears are characterized by retraction and heterogeneous fluid extending proximally between the medial head of the calf muscle and the soleus. When the lesion heals, the fibrous tissue between the medial aspect of the calf and the soleus muscle can be identified as an area of heterogeneous increased echogenicity. The treatment of tennis foot is generally conservative.
General information
The calves (regio suralis) are the rear upper muscle area of the lower leg. However, not all calf muscles are calf muscles. The most important muscle in the calf region is the triceps (triceps surae muscle). Anatomically, it is correct to divide the musculature of the lower leg into the following parts:
For more information see the topics: Superficial Tibialis Muscles and Deep Tibialis Muscles There are only two muscles called the calf muscles:
4+5 Triceps calf muscle? (triceps surae muscle).
The triceps surae is the calf muscle combined with the soleus and is one of the strongest muscles in the human body. The plantaris muscle can also be interpreted as the fourth head of the calf muscle.
4. Biceps calf muscle
The biceps calf muscle belongs to the posterior superficialis group. It is a muscle that largely determines the external appearance of the calf. Its two protuberances are clearly visible when standing on tiptoe.
- Function: tightens the leg and can twist it outwards
- Origin: lateral head: femur and lateral condyle - medial head: medial condyle of femur
- Anchoring: via the tendon of the Soleus muscle as an Achilles tendon on the heel bone
- Denervation: muscular branches of the deep fibular nerve
In plastic surgery, this calf muscle has a double meaning. On the one hand, it can be used to correct a defect in the knee area. On the other hand, in the case of extremely large calves, it can also be completely or partially removed without functional restrictions (calf hypertrophy), with shortened calves. On the other hand, it can also be removed completely or partially without functional impairment by performing a calf reduction.calf muscle hypotrophy) it is possible to enlarge the calves with calf implants. This usually occurs between the gastrocnemius muscle and the tibial fascia. For more general information see the chapter on calf corrections.
Treatment of calf pain
Compression therapy is useful for varicose veins. The patient's legs are fixed with elastic bandages that relieve pressure on the vein walls, thus reducing the risk of stretching and blood clots. Compression clothing improves well-being and eliminates the feeling of heaviness and pain in the lower limbs. To correct painful venous circulation disorders, venotonics are prescribed, which must be taken orally to improve the venous system and blood vessels throughout the body. To relieve inflammation, a regimen is prescribed, which also includes taking nonsteroidal drugs. Angioprotective drugs are used to strengthen the stretched inner vessel walls in the lower limbs. With myositis of the lower limbs, the affected muscles in the foot should not be strained. To protect them, the doctor can bandage the inflamed area on the leg with an elastic bandage and place a warm compress with anti-inflammatory gels or ointments underneath. Physiotherapy treatments such as magnetotherapy and paraffin therapy have also been shown to be effective in myositis as they improve blood circulation and reduce calf swelling.
Surgical intervention is required for severe purulent leg inflammation. After the operation, the patient must undergo mandatory antibiotic therapy. With parasitic and toxic myositis, drugs are prescribed to flush parasites and harmful substances from the body. If the calf muscle is damaged, massages are combined with heat treatments. Painkillers can also help relieve calf pain. If infectious myositis is diagnosed, antiviral drugs and antibiotics are prescribed. In diseases caused by ischemia, vasodilators are used. If the nerve inflammation is caused by an injury in the calf, B vitamins, pain relievers, and medications are taken to reduce swelling.
The following methods are used to treat calf pain:
prevention of pain
To prevent soft tissue inflammation and avoid calf pain, consider these recommendations for good health:
- Massage your legs after a day's work to improve blood circulation, reduce swelling and prevent fatigue;
- Change in diet by enriching it with fruits and vegetables;
- hot foot baths to improve heat exchange;
- vitamin and mineral complexes 2-3 times a year;
- moderate physical activity;
- limiting alcohol and coffee consumption;
- walking breaks and breaks from strenuous work;
- weight loss;
- avoiding tight clothing that compresses the veins;
- choosing comfortable, low-heeled shoes;
- foot baths with cool water; go barefoot in summer.
clinical signs
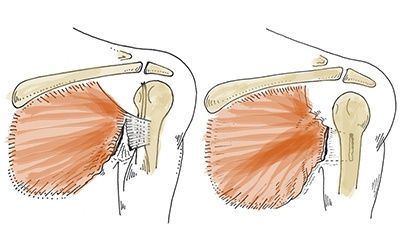
Most often, a muscle tear occurs in the lower leg or other parts of the body in competitive athletes: gymnasts, wrestlers, volleyball players, weightlifters, rowers, etc. The symptoms of a muscle tear are primarily severe pain that is localized to the injured muscle.
- disruption of muscle continuity;
- A defect in the muscle that can be detected by examination and palpation;
- bulging of the muscle on the side opposite the tear in the form of a roll (in the case of a complete tear);
- Hematoma and swelling at the site of injury.
symptoms
An acute pain syndrome immediately after the impact, strain or sprain is the main symptom. Blood loss and hematoma (if there is no epidermis tear) follow. Mobility in the affected area is limited and any attempt to stretch the muscle tissue causes severe pain. This symptom is observed with both a full and partial rupture. There is rarely a deepening in the affected area, which can be clearly felt on palpation.
For a partial tear, a cast is applied to fix the injured limb in a position where the edges of the injured muscle are as close together as possible.
A complete muscle tear requires surgical intervention in which the muscle itself is sewn up with surgical sutures. Suture material is also used in the event of a tendon tear.
Professional medical care is crucial for a good prognosis. During recovery, full function of the muscle is restored. If this is not observed, there is a risk of severe scarring, which limits the mobility of the muscle.
Benign curl-fasciculation syndrome
The most common symptom of benign curl fasciculation syndrome is twitching of the thigh muscles (including the fascia in the buttocks) or the lower leg muscles (fascia in the calf muscles).
Sudden spasms or involuntary muscle contractions;
Anxiety symptoms (headache, shortness of breath, lump in the throat).
The fasciculations in the legs and buttocks can last from a few seconds to several years (they occur at regular intervals, e.g., 2 to 4 times a day).
On examination, there is no decrease in nerve conduction velocity, a decrease in sensitivity, or a change in reflexes.
Do benign fascioculations occur in a healthy person?
Mild fascioculations in healthy individuals usually occur during muscle relaxation: during sleep, in the morning, at rest. But there can also be other causes:
- Excessive physical activity (exercising, lifting weights, etc.);
- Excessive physical exertion (overexertion);
- excessive exertion; Stress;
- excessive cold;
- Unhealthy habits (alcohol consumption, smoking);
- Excessive caffeine consumption.
Muscle twitching can occur as a result of trauma or mineral (magnesium and calcium) deficiencies.
Convulsions resolve spontaneously after a period of time (the interval may depend directly on the duration of stress or other nervous system overload) without muscle weakness, atrophy, or loss of sensitivity. They are not life-threatening or clinically significant and are therefore classified as 'mild'.
As a preventive measure
To prevent muscle spasms associated with pain, experts recommend muscle stretching exercises. Such an exercise is quite simple.
To do this, you have to stand about a meter away from a wall. Then lean forward and touch the wall. Don't lift your feet off the floor for even a second. Stay in this position for about five seconds, and then return to the starting position. The exercises should be performed three to four times a day for five minutes.
Training on a stationary bike is another effective preventive measure. This is especially advisable for people who are sedentary and lead a sedentary lifestyle.
Doctors also recommend wrapping your feet in a blanket before bed and drinking plenty of water throughout the day to help prevent croup.
If you want to prevent croup, you should also avoid alcohol, coffee and tea (or minimize their consumption) and, if possible, not take any medication that can trigger the syndrome.
What to look out for
The choice of treatment plan for calf pain depends on the cause of the discomfort. In most cases, surgery is not necessary; conservative measures such as medication, physiotherapy and physical therapy may be sufficient. These measures will help:
- to improve blood circulation;
- to suppress inflammatory processes;
- eliminate pain and swelling;
- flush out toxins;
- Strengthening of ligaments and muscles.
It is dangerous to self-administer drugs and other therapeutic measures. For example, heparin-based drugs are prescribed for thrombosis, but when blood does not clot properly or the walls of the vessels are weak, these drugs can cause bleeding. Too much exercise can damage the musculoskeletal system, while too little exercise will not have the desired therapeutic effect. For this reason, only the doctor should create a treatment plan that includes a series of exercises.
The Hello! clinic network has the most modern diagnostic devices, which enable a precise diagnosis to be made in the early stages of the disease. Experienced doctors develop individual treatment and rehabilitation plans for patients based on classical and modern techniques, which allow them to quickly get rid of their pain, without side effects and without the risk of recurrence.
Human Calf Muscle Anatomy Information:
The calf muscle – A biceps muscle located on the posterior surface of the human calf. It is located above the cambialis muscle, with which it is attached to the heel via the thick Achilles tendon.

The functional activities include above all the movement of the foot in the sagittal plane and the stabilization of the body during movement (walking and running). When the calf muscle is overstretched, cramps can occur. In addition, spasms can indicate a disruption in the arterial and venous blood supply. Injuries to the calf muscle can result from overuse, sometimes from an impact.


Which doctors you should go to for a calf muscle exam:
Is something worrying you? Would you like to learn more about the calf muscle or do you need an examination? You can make an appointment with dr. – Clinic Eurolaboratory is always there for you! The best doctors will examine you, advise you, provide the necessary care and diagnose the problem. You can also doctor at home. clinic Eurolaboratory is open for you around the clock.
How to contact the clinic:
Phone number of our clinic in Kiev: (+38 044) 206-20-00 (multi-channel). The secretary of the clinic will find a suitable day and time for you to visit the doctor. Click here for our coordinates and directions. For more information about all of the clinic's services, visit the clinic's website.
If you have previously been examined, remember to take the results with you to a consultation with your doctor. If examinations have not yet been carried out, we will carry out the necessary work in our clinic or with our colleagues in other clinics.
It is important that you take a very close look at your general health. There are many diseases that do not initially make themselves felt in our body, but unfortunately are treated too late. This simply means that you have to be examined several times a year to be examined by a doctor several times a yearnot only to prevent a terrible disease, but also to keep the body and the whole organism healthy.
If you want to consult a doctor, you can find and read answers to your questions on the Internet Tips for self care. If you are interested in reviews of clinics and doctors, you can get information on the forum. You can also go to the medical portal EurolaboratorySign up to keep up to date with the latest calf muscle news and updates on the site, automatically sent to your inbox.
Clinically Relevant Anatomy
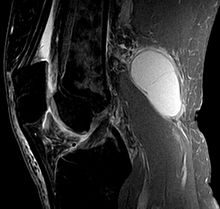
A Baker's cyst is an enlarged bursa that lies between the medial head of the calf muscle and the capsular equivalent of the semitendinosus muscle—the cervical collateral ligament.
For a cyst to form, two conditions must be met: an anatomical connection and chronic joint effusion. A joint effusion in the knee joint can fill the calf and adductor muscle capsules with synovial fluid, and when fluid outflow is impeded by a unidirectional mechanism, the calf and adductor muscle capsules enlarge into a pseudocystic cavity called a Baker's cyst.
Epidemiology/Etiology
A Baker's cyst, or popliteal fossa cyst, develops when there is an underlying problem with the knee joint that is accompanied by an inflammatory response caused by the formation of intra-articular bodies in osteoarthritis, rheumatoid arthritis, rupture of the anterior cruciate ligament or meniscus, or by Particles mainly from the polyethylene padding after a knee endoprosthesis.
- A primary cyst is a mass unrelated to the pathology of the knee joint.
- A secondary cyst is an enlargement of the synovial sac between the tendons of the calf muscle and the semitendinosus. Fluid enters through the canal that connects the normal synovial sac to the joint. This is the most common occurrence.
The size of the cyst can vary from very small (asymptomatic) to large, but resizing is very common. A septum separating the semitendinosus and calf component may be present, particularly in small cysts. This can act as a valve, allowing fluid to enter the subclavian cyst instead of exiting it.
There are differences between cervical cysts in children and adults. In children, these are cysts filled with jelly-like material that form in the back of the knee. They are usually asymptomatic and are not associated with intra-articular pathology. They often resolve spontaneously, although this process can take several years. In adults, Baker's cysts often occur in conjunction with other intra-articular pathologies and inflammation.
What should I eat if I have cramps during pregnancy?
Nourishment – A key factor in preventing or reducing spasms and pain. What to eat if you have leg cramps during pregnancy? In particular, we recommend:
- Foods rich in magnesiumBuckwheat, legumes, spinach, wholemeal bread, fish, almonds, nuts, cocoa, dark chocolate;
- Foods rich in potassium: beans, broccoli, carrots, tomatoes.legumes, broccoli, spinach, carrots, tomatoes, grains of all kinds, oatmeal;
- Foods rich in vitamin B6including meat, sausage and fish, potatoes, rye and wheat bread.
However, alcohol and coffee should be strictly avoided. Hard drinks should be avoided during pregnancy. during pregnancy Hard drinks are generally forbidden during pregnancy, and coffee causes magnesium to be absorbed from the body.
Calf cramps in the first, second and third trimester of pregnancy and after childbirth
Leg cramps are at their worst in the third trimester, just before the upcoming one childbirth. Apparently, this is due to the aggravation of the mechanisms described above, such as weight gain, restriction of movement, significant increase in the uterusand nightly snacking, etc.
Keep in mind that labor doesn't always go away automatically after you give birth. Even if your weight is gradually returning to normal and Print the uterus under Annoy i vesselsThe demand for magnesium continues to increase. According to research, the magnesium requirement of breastfeeding mothers is also quite high. Therefore it is important to familiarize yourself with your doctorwho will prescribe you an appropriate daily dose.
Read more:- Acute pain in the calf muscle when running.
- Calf muscle cramps when walking.
- Inferior paresis - what is it?.
- Which muscles hurt after running?.
- cruciate ligament of the foot latin.
- Clubfoot exercises for kids.
- What types of foot.
- How to enlarge the foot.
