Depending on the severity of the injury, the leg can be weight bearing after a month in mild cases and after three months in severe cases. Of course, putting weight on the leg for such a long period of time is problematic, which is why crutches can be used. It is advisable to wear special footwear or supinating shoes for up to a year.
- Sprains and subluxations of the forearm
- causes
- Types of lower limb dislocations in children
- Symptoms of a dislocated leg in children
- sprains of the ligaments
- degree of sprain
- torn ligaments
- Symptoms of torn ligaments:
- Sprained ankle: treatment
- Avoiding re-spraining your ankle
- prevention of injuries
- Answers to common questions
- What first aid does the injured person need?
- How long does rehabilitation after an injury take?
- How is the CCHS developing?
- Benefits of treatment at the ON CLINIC
- Consequences of an ankle sprain
- Prevention of ankle injuries
- Sprained foot: which ointment will help?
- therapeutic measures
- rehabilitation and recovery
Sprains and subluxations of the forearm
Every joint, ie the flexible connection between two bones, has a certain 'degree of freedom' – and only within this range is the natural human movement, bending and stretching, etc. possible.
When the head of one of the bones protrudes beyond the anatomical bed allotted to it by nature and cannot retract on its own, it is called a dislocation or subluxation. The difference between the two can often only be determined by an instrumental examination (eg X-rays): a complete dislocation is accompanied by destruction of the ligaments, while a subluxation can cause the ligaments to be stretched but not torn. Another criterion is the presence or absence of contact between the articular surfaces: in a subluxation there is at least partial contact, while in a complete dislocation there is no contact.
Symptomatically, dislocation and subluxation are very similar - the joint is red and swollen, the limb is in an unnatural position, its mobility is severely restricted (with associated nerve damage, tactile sensitivity may also be impaired), and the injured person usually feels strong pain.
From a mechanical and anatomical point of view, the tendency that traumatologists have known for a long time is quite natural: the more complex the joint, the more complex, varied and dangerous the dislocation.
Shoulder dislocations are the most common in trauma statistics. The second most common are dislocations and subluxations of the forearm (20-25 % of all recorded traumatic dislocations). According to some data, the gender and age structure of victims is dominated by men aged 10-30 years and women over 50 years.
A subluxation of the forearm is considered an age-related dislocation if it is not resolved after two weeks.
causes
The causes of (sub)luxation of the ulnar and radialis bones are as diverse as the causes of dislocations in general. The absolute leader is traumatic mechanical impact: bumps, falls with the arm erect or half-bent, trying to hold an unbearable weight, etc. However, the topic of this article is not the acute, but the long-term dislocation of the forearm, and it is not accidental that such an injury is highlighted as a special problem for traumatology. With a chronic dislocation, intensive degenerative-dystrophic processes in the periarticular tissue, the so-called ossification, set in after two to four weeks: muscles and other elastic tissues are replaced by rapidly growing and ossifying scar tissue (in some cases cartilage). A characteristic feature of a long-term dislocation of the forearm is the impossibility (in the vast majority of cases) of reducing it by a closed method.
Types of lower limb dislocations in children
There are different types of this type of injury in terms of origin, severity, age, etc. e.g. eg, an ankle dislocation in a child can be external, internal, posterior, and anterior.
- Acquired dislocation when due to trauma or other external causes;
- congenital dislocations resulting from congenital malformations and injuries sustained during childbirth.
A distinction is made between complete dislocations, in which there is complete separation of the joint parts, and incomplete dislocations, in which the joint surfaces partially come into contact.
Specialists also classify injuries by the age of the injury, distinguishing between fresh (up to 3 days), non-fresh (up to 3-4 weeks), and old (more than 4-5 weeks) dislocations.
Symptoms of a dislocated leg in children
The symptoms of an injury depend largely on the type and location of the injured joint. Common symptoms of a dislocated leg include:
- sharp, stabbing pains at the time of injury;
- significant swelling of the injured area;
- reddening of the skin;
- Increased local skin temperature in the area of the injury;
- Decreased sensitivity; numbness in the area of the injury;
- inability to move;
- bruising;
- External deformation of the joint area.
A child with such an injury complains of increased pain when trying to move his leg, take a step, or turn.
sprains of the ligaments
ligament strains A sprain occurs when a person makes sudden movements with a force that exceeds the allowable load on the joint. When a ligament is pulled, the ligament capsule that stiffens the joint is partially damaged or incompletely torn.
The ligaments of the ankle (especially when rotating the foot) and the wrist are most commonly damaged. Damage to the ligaments of the knee joint is less common. In high-heeled shoes, the foot often twists inward, stretching the Achilles tendon.
degree of sprain
The following degrees of ligament injuries can be distinguished:
- grade 1A sprain is defined as a ligament rupture in which the mechanical integrity of the ligament is preserved, with individual fibers tearing. Slight swelling without bleeding is characteristic. The patient may experience moderate pain, limitation of movement and support;
- Grade IIThe articular sac of the ligaments is partially damaged, there are numerous fiber tears, frequent blood loss and moderate swelling. Support is difficult to maintain and movement is quite painful and limited. There is some instability of the joint.
- grade 3Complete ligament tear with severe pain, swelling and bruising. The instability of the joint is noticeable during movements.
In the case of grade 1 and 2 ligament tears, conservative treatment is usually sufficient.
Complete ligament tears are treated surgically.
torn ligaments
Torn ligaments – A common injury in people whose work requires a long physical strain. In most cases, a torn ligament is associated with a sprain or fracture, but it can also occur as an injury in its own right.
Depending on the cause of the injury, a distinction is made between traumatic and degenerative ligament tears. While the first type of injury can be caused by trauma, the second occurs as the body ages.
Symptoms of torn ligaments:
- Joint pain and restriction (inability to straighten or raise the injured arm or leg);
- swelling, hematoma;
- change in the outer contour of the injured joint (joint instability);
- Numbness and tingling in the injured limb.
A special case of ligament tear is damage to the meniscus.
Sprained ankle: treatment
What to do if you get one sprain How do you start with a sprained ankle? If the symptoms are clearly visible and it is clear that moderate to severe contortionIf symptoms persist and worsen during the sprain, seek professional medical help immediately.
If symptoms persist and worsen within 36 hours, there is cause for concern and it is immediate seek immediate medical advice to a specialist. Physician Consult a specialist doctor and, if necessary, refer him to one X-RAY. And what treatment does he usually prescribe for severe ones dislocated hock?
First of all, a bandage is created a bandage or cast for a few days or weeks, and anti-inflammatory drugs are prescribed.
And how will treat sprained Self-treat ankle if we're sure it's a minor injury? And what is particularly important in order to act immediately, as quickly as possible?
In the first place are rest and cold. Ice wrapped in a cloth or towel should be applied to the ankle 34 times on the first day. To avoid frostbite on the painful area, the ice compress should not be used for more than twenty minutes.
Other immediate measures include applying compression associationand elevation FootA neck roll or pillow can also be placed under the foot for 23 days.
more elastic bandage tightening bandage should be applied very gently and not disturb the natural circulation of the foot Foot. This can be recognized by the color of the skin: below below the bandage The skin should not take on a purplish-blue tint. The normal sensitivity of the skin should also be intact and there should be no tingling in the foot and toes. feet.
These measures will help reduce inflammation and bruising caused by reduced blood flow to the affected area vessels Ankle. It is better to use a cane or crutches to move around the house.
Avoiding re-spraining your ankle
Nobody wants to get hurt again. Special physiotherapeutic treatments to strengthen the tendons, increase their flexibility and stretch the calf muscles should be carried out as a preventive measure. Only an active lifestyle can eliminate the risk of a sprain.
Such trivial exercises are the best prevention against injuries. But of course without fanaticism and with care. People with a sedentary lifestyle are at the top of this risk group. Proper footwear also helps prevent injuries: wear fewer or no high heels, uncomfortable shoes and large platforms.
prevention of injuries
The following tips will help reduce the risk of ankle injuries:
- Before every workout, do a warm-up routine. This improves the mobility of the ligaments and makes them less susceptible to impact;
- Be as cautious as possible on slippery surfaces. It's best to hold on to handrails. Elderly people should always use walking sticks for support in slippery conditions;
- Shoes should be comfortable and have a stiff heel cap and a stable heel height of up to 4 cm;
- Do not jump from great heights. This is especially true for young people, as they are more likely to injure their lower limbs when parking.
In the first few months after the injury, special attention should be paid to protecting the joint. It is advisable to wear orthotics or wrap the sprained joint with an elastic bandage. The rehabilitation period is also supported by special exercises that can be ordered with delivery in the TopZdrav shop.
Answers to common questions
What first aid does the injured person need?
It is important to know that the level of assistance depends on the severity of the injury. Ankle subluxation does not cause much pain and there is no obvious deformity of the foot, although it is impossible to kick the foot. The injured person should be given a cold compress, bandaged (scarf, sling) and taken to the hospital.
In cases where the symptoms clearly indicate a sprain or a torn ligament, first aid should be carried out in several stages:
- Remember to remove shoes as the swelling makes it difficult to do so later without pain;
- Place the limb in an elevated position - place a pillow, bag or rolled-up jacket under the foot;
- Put cold on the injured area. This can be a bag of frozen berries, ice cream, or any other product from the freezer. The sachet should be wrapped in a towel or other thick cloth before use. The duration of the compress in the emergency phase is 15 minutes, no longer, otherwise frostbite may occur. However, frostbite can be repeated after a break of 10-15 minutes.
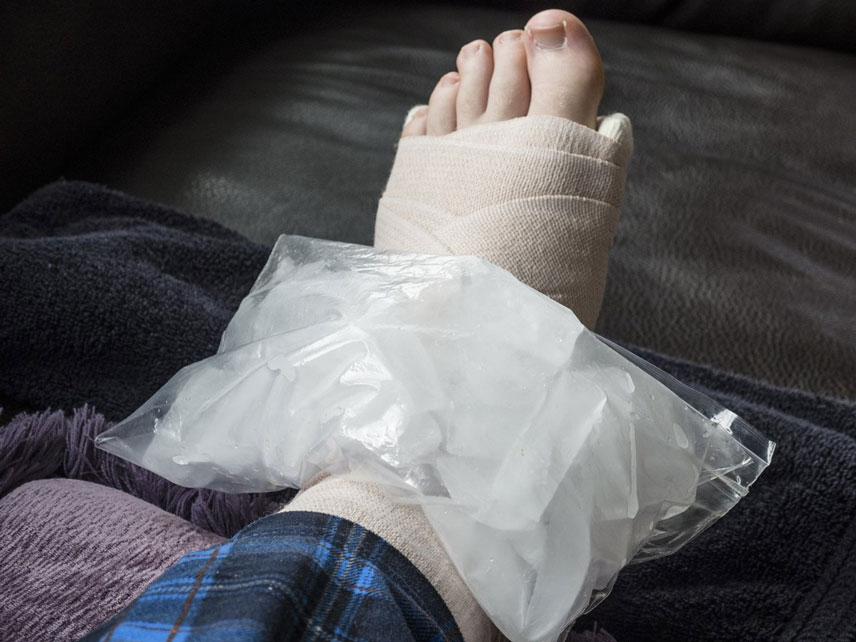
If the foot is significantly deformed, twisted or bent, the bandage should not be applied. It is enough to fix the limb so that it does not move during transport. It is advisable to take the injured person to the hospital for treatment within 2-3 hours of the injury.
How long does rehabilitation after an injury take?
Complete restoration of ankle anatomy and function depends on the severity of the injury. In the case of subluxations, rehabilitation usually takes up to 2-3 weeks. In the case of dislocations, the joint instability persists for up to 4 months. During this time, excessive strain should be avoided, ie jumping, dancing and running should be avoided. Massage, simulation exercises, wearing bandages and orthopedic shoes are helpful.
How is the CCHS developing?
Human spatial movements (walking, jumping, running, etc.) are not possible without the proper functioning of the ankle joint. This joint is made up of the bones of the tibia, fibula, and talus. The stability of the bones and the connection of the foot with the lower extremity is ensured by ligaments.
On the outside, the stability of the foot is provided by the tibiofemoral, calf-femoral, and anterior and posterior talofemoral ligaments, and on the inside by the deltoid ligament (medial ligament). The connection between the tibia and fibula is made by the tibiofibular ligament. The calcaneal ligament helps hold the talus in place during extension. The anterior fibular ligament attaches to the perineal process and the talar neck, the posterior fibular ligament attaches to the perineal process and the posterior talar process. The medial ligament on the inside of the leg, in turn, connects the shin, ankle, heel, and ankle bone.
Repeated trauma, sprains, dislocations, ankle injuries, long-term fibula tendinitis, or other patient events result in instability - the inability of the ligament to maintain the correct position of the foot during walking, jumping, or other exertion. The ligaments on the outside of the foot, one edge away from the fibula (thinner) are more commonly affected, while the deltoid ligament on the inside of the foot (thicker) is less commonly affected.
This condition of uncontrolled changes in foot position during work is known as ankle instability. If left untreated, chronic instability develops, affecting quality of life and making it difficult for patients to move about space safely.
Various anomalies of the foot related to the nervous system (abnormal perception of position in space, lack of sensors and weakening of nerve signals, disruption of the stage of analysis of signals from sensors controlling body position, etc.) or muscle function (increased reaction time, reduced action strength) are widespread. These abnormalities can occur after a ligament injury and lead to chronic ankle instability (CNLS).
Benefits of treatment at the ON CLINIC
- Qualified medical specialists. The experienced and competent doctors at the ON CLINIC are specialists at the highest level. They keep up to date with the latest developments in the treatment of joint diseases, regularly exchange experiences with colleagues from Russia and abroad, and conduct scientific activities.
- The clinical and laboratory facilities are excellent. Our clinics have state-of-the-art, efficient and safe equipment for effective diagnosis, treatment, prevention and rehabilitation. Our own clinical-diagnostic laboratory enables us to carry out rapid tests.
- The diagnosis is quick and effective. The excellent equipment of the clinic enables a wide range of diagnostic methods: magnetic resonance imaging, computed tomography and other examinations allow us to quickly and accurately obtain information about the state of health of our patients.
- Comprehensive approach. In the ON CLINIC, multidisciplinary consultation is common in order to achieve the best possible treatment results.
- effective therapy. A comprehensive, all-encompassing approach to treatment and prevention includes many modern methods.
- Individual approach. Therapy is tailored to the patient's gender, age, and other characteristics.
- Comfort. The clinics of our center are conveniently located in the center of Moscow. You can make an appointment anytime between 9am and 9pm. All communication with our employees and doctors at the ON CLINIC takes place in a relaxed and confidential atmosphere.
How do I know if I need surgery for CHNS?
Your doctor will be able to answer this question after an examination. Surgery is recommended if the ligaments are partially or completely damaged.
What is the difference between arthroscopy and endoprosthesis?
Arthroscopic techniques are used as a minimally invasive method to restore joint integrity and function. Arthroplasty replaces all or part of the joint if it cannot be restored.
Consequences of an ankle sprain
It is not uncommon for an ankle injury to be accompanied by a complete rupture of a ligament and a fracture of the ankle. Early medical attention is extremely important in such cases, as delayed or inadequate treatment can result in tendons and ligaments not healing properly and the foot becoming deformed and unstable.
This can lead to the following problems:
- Regularly recurring dislocations of the ankle.
- Progressive or developing diseases such as arthrosis or arthritis.
- Formation of dense scar tissue.
- Formation and growth of bone osteophytes.
- Difficulty moving the injured joint after it heals.
- Inflammation of the soft tissues surrounding the ankle.
- Chronic hemarthrosis.
- Complete or partial muscle wasting, impaired blood circulation in the limb.
It is important to know that neglected cases can only be rehabilitated through surgery, otherwise there is a risk of permanent disability.
Prevention of ankle injuries
The insidious thing about ankle injuries is that a sprained ankle increases the susceptibility to further injury from clumsy movement, improper footwear, fast walking, or exercise.
So if you frequently sprain your leg while walking and then have a long limp or fall on a 'flat spot', you should consider how you can prevent these conditions. To do this, proceed as follows:
- Choose and wear good quality shoes that fit your size and are comfortable to walk in. Preferably with a small, stable heel and an orthopedic insole. Women should be aware that walking in heels makes their feet more prone to injury, so avoid wearing them for long periods of time.

To avoid sprains and more serious ankle problems, care should be taken as most ankle injuries are caused by not looking under your feet when walking.
Sprained foot: which ointment will help?
The first task in treating the aftermath of an injury is to relieve the patient's pain. Painkilling ointments can easily meet the requirements and can be successfully used on the advice of a doctor and with an individual selection of painkillers. Immediately after the injury, only cooling painkilling ointments can be used. Painkillers with a warming effect are only acceptable a few days after the dislocation, when the inflammation is slowly subsiding. Popular ointments for this purpose are:
Short list of ointments for sprains:
- Dolgit;
- ketonal;
- voltaren;
- bystromgel;
- emulsifier;
- deep relaxation;
- fastum gel;
- Naiz Gel;
- Diclofenac.
The above remedies are easy to find at the pharmacy. They are based on nonsteroidal anti-inflammatory drugs and are used for bruises. They are safe and hypoallergenic and are even suitable for children of all ages.
Hormone mixtures should only be used with great caution in adults. They speed up the recovery process and help when other remedies don't work, but can often also be harmful. If a doctor prescribes a hormone mixture, it should only be used in the prescribed amount.
therapeutic measures
Addressing this issue involves a comprehensive approach. In a first step, the doctor administers an anesthetic to the patient and adjusts the dislocated joint. For this purpose, anesthesia is performed. This can be local or general.
During general anesthesia, the muscles are completely relaxed. This makes it easier to carry out the repositioning. Treatment measures vary depending on the degree of dislocation:
- Grade 1. After the dislocation, an elastic bandage is applied for at least 3 days. This is followed by compresses, iodine netting, physiotherapy and massage. The foot must rest until the bandage is removed. The therapy takes place at home.
- Grade 2 Once the ankle is reduced, the doctor applies a cast. The cast is worn for 10 to 14 days. The full recovery time is at least 21 days. After the cast is removed, physical therapy, massages and wraps are required.
- Grade 3 Once the bone is immobilized, the doctor applies a cast. The foot is placed in a cast from the toes to the upper shin. The shoe is worn for at least 1 month. After the cast is removed, the same measures are taken as for grade 1 and 2 injuries. In this case, the patient may experience severe pain, so novocaine injections are administered.

During the dressing and recovery, anti-inflammatory and analgesic drugs are prescribed: Nimide, Ibuprom, Ibuprofen, Dicloberl. In home treatment, both tablets and ointments (gels) are used. This comprehensive approach helps in cases where the pain is long-lasting.
Sometimes doctors recommend the use of anticoagulants. Such an ointment allows the bruise to quickly subside, which speeds up the recovery of the leg. With a complete rupture of fibers and ligaments during the injury, surgical intervention is required.
rehabilitation and recovery
An important step on the road to full recovery is rehabilitation. Once the bandage is removed, the patient should take a short walk. Therapeutic exercises are always recommended and include the following:
- Squeezing and relaxing the toes of the painful foot;
- Alternating movement from heel to toe;
- Walking outwards and inwards on the heel;
- turning a round object with the foot;
- To swim;
- Training on a stationary bike.

Once the muscles of the ankle are strengthened, jogging and light jumping can be done with caution. Physiotherapy – UHF – is recommended as an additional preventive measure. Five to 10 sessions may be sufficient to treat mild to moderate cases. The affected leg can be fully loaded no earlier than 1 month after the beginning of the rehabilitation period.
Rehabilitation may involve the use of ointments. These reduce inflammation in the joint. It is recommended to apply the ointment on the leg for 1-2 weeks. Supportive rehabilitation measures may include electrophoresis, cryotherapy, radon foot baths, and paraffin applications.
If the ankle was operated, specialists recommend wearing supinators and special orthopedic shoes during the rehabilitation period (about 6 months). How long you have to wear these shoes depends on how quickly your foot heals.
Read more:- Treated subluxation of the ankle.
- Inward subluxation of the foot.
- X-ray foot subluxation.
- dislocation of the ankle.
- Ankle ligament strain, ICD.
- Injury to the ligaments of the ankle.
- Damaged ligaments of the ankle.
- contusion of the ankle.
