Later, when the baby is a few weeks old, engorgement may occur in one or more milk lobes. This often manifests itself as a fairly large, painful lump, ball, or lump in one part of the breast.
- Fallen nail: why it occurs and how to fix it
- The bent nail problem
- Who is recommended to use shoe soles
- How to choose an RCA?
- WET SHOES
- CONCLUSIONS AND TOTALS
- Why does the vagina fart?
- Causes of vaginal farting
- What to do if your vagina farts
- How to do Kegel exercises
- preventive measures
- Summary
- production form.
- Storage tips
- Special properties of the materials
- If the inflammation in the breast has already started
- What causes engorgement in a breastfeeding mother?
- Insertion of tampons with medication
- How effective is vaginal tamponade?
- tamponade technique
Fallen nail: why it occurs and how to fix it
The problem. It is an embarrassing and ugly sight when one, several or all of your toenails or fingernails curve down as if to peck at something. And it's not even about aesthetics: this defect can indicate serious problems in the body. That's why it's so important to know how to fix a bent nail and prevent it from curling again. The solution. The elimination of the deformation depends on the cause of its occurrence. There are many options, but most of them only work in combination, with prevention of the curvature playing a large role. But first you should see a specialist – a family doctor, dermatologist, podiatrist or mycologist. Only he or she will be able to tell you what type of crooked nail repair will help you.
- The problem of the broken nail
- Causes of a bent nail
- Diagnosis of a curved nail plate
- How to fix a crooked nail
- How to fix a crooked nail without pathology
- Folk remedies to help correct a crooked nail
- How to prevent crooked nails
The bent nail problem
The nail plate of a healthy person is smooth and even, pale pink in color. Many conditions affect their appearance and structure. These include, in particular, the general condition of the body and its individual systems, the amount of trace elements supplied, especially calcium, and the constitutional characteristics of the nail structure.
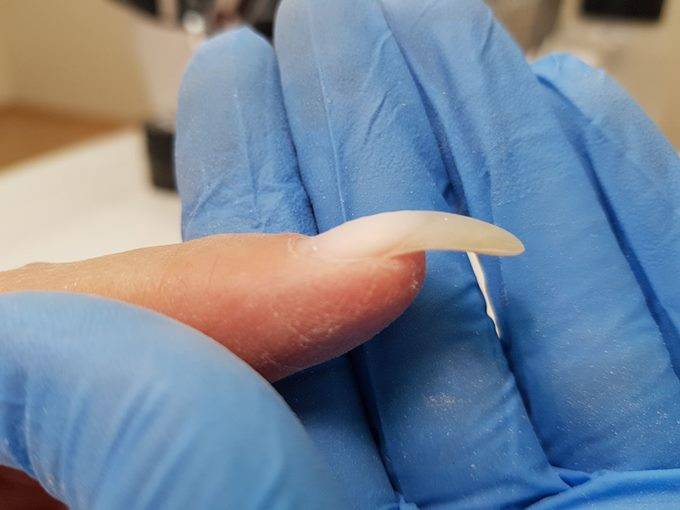
Any change in the normal state of the nail plate serves as a signal for health problems. The most common external signs are pitting, growths, roughness, delamination, yellowing of the nail and deformation.
One of the most common nail plate defects is its downward curvature. This deformation occurs when the weakened nail becomes thin and soft, bending at the edges and growing into the sides of the cuticle.
It is difficult to correct a crooked nail yourself, because even a professional manicure will not solve the problem. Such a nail shape not only looks unsightly, but also causes practical problems: the curved nail interferes with simple activities and bumps into clothes, hair and objects that we use.
This type of deformation is most common when the nail plate grows back on the middle and index fingers. This defect can go unnoticed for a long time if the manicure gives the nail plate an oval, square or soft-edged contour.
When the nail structure is altered (increasing the length, filing into a ballerina, stiletto, or almond shape), an abnormal direction of growth is evident. Improper technique or unsuitable nail architecture can also be the cause of this defect.
Who is recommended to use shoe soles
- people in the last months of pregnancy;
- people whose body weight is above the norm;
- People who suffer from calluses or corns on their feet.
- tendon sprains;
- plantar fasciitis;
- Diseases of the spine and joints of the lower limbs;
- different leg lengths (less than 3 cm);
- arthritis, arthrosis;
- heel spur;
- injuries in the heel area of the foot;
- flat feet;
- other foot problems.
- injuries to the sole of the foot;
- microangiopathy and diabetes with ulceration;
- Vascular diseases, in which blood flow in the feet is impaired;
- Acute arteriosclerosis.
If one leg is no more than 2-3 cm shorter than the other, you can make up the difference by putting a garter under the shorter leg. In this case, do not choose a product made of elastic material, such as B. Silicone, as this puts undue stress on the foot when walking. It is better to choose a stiffer bondage belt. They are usually multi-layered and have a hard-wearing upper material (natural leather, microfiber).
How to choose an RCA?
To choose the right orthopedic product, you should consult your doctor. Only he can recommend which ball shoes are most suitable for your specific problem and, if necessary, suggest the correct thickness of the insoles (3-12 mm). The choice depends on the condition and the goal to be achieved. The special design of the product reduces the likelihood of heel injuries, eliminates corns and blisters, helps reduce pain when walking and corrects foot deformities.
The material of the insoles should be chosen depending on the intended use of the instep pad:
1. Silicone insoles are recommended:
- for sports activities,
- with heel spur,
- after injuries to the Achilles tendon,
- for convalescence after fractures,
- with salt deposits in the joints of the lower limbs;
- For painful heel, knee or ankle joints.
They prevent blisters and cracks, counteract the development of flat feet and relieve leg fatigue. These products have a clear orthopedic effect, but are quite complex in design and are not suitable for dress shoes. Silicone is non-allergenic and provides good shock absorption when walking and running (e.g. Cinch ST-41).
2 Gel products are intended more for prophylaxis. They reduce pressure on the heel and prevent spurs, cracks and blisters. These thin and soft insoles can be used with model shoes. They are not suitable for serious illnesses.
3. Leg length correction insoles are used for back and joint problems as well as flat feet. They have a good orthopedic effect, but cannot be worn with all shoes because they are quite wide.
4. Special leather soles with a latex base ensure an optimal microclimate in the shoe and prevent the development of plantar fasciitis. They are also used for different leg lengths. These products have almost no orthopedic effect, but in addition to their excellent ventilation properties, they are distinguished by their high quality and durability.
WET SHOES

This can especially happen in near-freezing temperatures when there are puddles or slush.
Some moms are convinced that it's okay to walk through puddles in snowshoes because the material protects against moisture. And of course it does. The material is moisture-repellent. It protects against splashing water and snow. But the seam between the rubber boots and the fabric is not airtight. Water can penetrate through this seam if you e.g. B. standing in a puddle.
Therefore, when wearing snow boots, you should not step in water that is higher than the rubber boots.
If you have to walk through deep puddles, opt for EVA boots. These are breathable and warm - even in colder waters. And they are warm (for cold water).

Another cause of wet shoes is mechanical damage. For example, punctured, damaged shoes. A few micro cuts and that's it. The shoe is leaking.
The best way to check shoes for mechanical damage is to place them in a pool of water (but not so high that they could leak) for a few hours and stuff the insides with newspaper. If the newspaper gets wet, we have a leak. Shoes are checked in the same way if there is a suspicion that they are leaking near the sole.
Whenever the shadow of a doubt causes the shoes to leak - straight into the sink!
CONCLUSIONS AND TOTALS
It's damp inside, but your feet are dry - condensation. We just dry the shoes and that's it. There's no point in fighting physics.
It's damp inside - your feet are wet. Your feet are probably sweating. Shoes and socks must be adapted to the weather.
It's damp inside - your feet are wet. Your shoes may be leaking. This is probably due to misuse or mechanical damage. It's not difficult to find the cause.
The ideal is to check for leaks (in a pool of paper) immediately after purchase.
Unused shoes can hardly be held responsible for mechanical damage.
And don't forget the manufacturer's 30-day guarantee. This is enough time to discover a defect. But in 99.9 % cases, wet feet are due to the three causes mentioned.
hp A situation where the water overflows (if you step into a very deep puddle) is not a problem - everything is all too obvious there.
Why does the vagina fart?
This can happen to any woman with a vagina, at any age. However, the sound of the vaginal fart often occurs during intimate moments. With age or after having children, the vaginal canal expands slightly. It loses its former tightness. With strenuous exercise, sexual intercourse, or other activity such as coughing, sneezing, squatting, etc., these loose walls expand and some air is drawn into the vaginal canal from the outside like a pump and is recruited there. When the vaginal walls contract again, this air is expelled out through the vagina, accompanied by the characteristic sound of 'farting' or 'snoring'. During intercourse, this is more likely to happen in the kneeling and 'cowgirl' positions.
The pelvic floor plays a key role in this concert, as the pelvic floor muscles can constrict the vagina and vaginal opening. We know that vaginal bloating is common after childbirth and is more common after multiple births through the natural birth canal. But it also affects women of all ages and after a cesarean section, hysterectomy or perineoplasty.
Causes of vaginal farting
The main causes of increased vaginal sounds are a weak or tight pelvic floor, prolapse and flexion of the uterus combined with weak anogenital muscles, known as vaginal relaxation syndrome. Because the pelvic floor responds to our hormones, some women fart more often during ovulation or menstruation.
A tight (spasm) pelvic floor can act like a suction, drawing air into the vagina, and then a whistle, releasing the trapped air with a slower, higher-pitched note. Remember that a tight pelvic floor works the same way as a weak pelvic floor because it often doesn't relax or contract properly. A weak pelvic floor lets in more air and then expels it with a fast, deep sound as abdominal pressure increases due to lack of control of contractions.
What to do if your vagina farts
A perfectly functioning pelvic floor does not allow a lot of air to be sucked into the vagina during activity, since the vaginal space is shaped and narrow by good tone at rest. A properly functioning pelvic floor moves with inhalation and exhalation, allowing small amounts of trapped air to escape naturally and silently.
How can I avoid having to fart air through my vagina during sex? There are 2 ways to solve the problem: conservative and surgical. The first consists of training, exercises to strengthen the vaginal muscles, combined with a special pelvic massage, and the insertion of hyaluronic acid fillers to seal the vaginal opening. The surgical way to eliminate vaginal bloating and stop farting during sex is plastic surgery of the anterior and posterior walls of the vaginal canal, or comprehensive levatoroplasty. These services are offered in our clinic in Moscow. Let's take a quick look at each of the points mentioned.
How to do Kegel exercises
When you urinate, contract your muscles to stop the flow of urine for about four seconds. Then relax those same muscles to get the urine flowing again. These are your pelvic floor muscles that you work with Kegel exercises.
To make sure you're using the right muscles, insert a finger or two into your vagina. Tighten those muscles. If you feel your fingers tighten (even just a little), it means you've found the right muscles and they're working! Repeat Kegel exercises about five to ten times a day, ten times per session. You have to be patient as it may take up to 8-10 weeks before you notice an improvement but it will definitely happen. If you supplement your regular Kegel exercises with special intimate devices (kegel, intravaginal trainer) and a pelvic floor massage, your treatment can progress better.
preventive measures
Prophylactic measures for defecation are prescribed every time the sanitary napkin is changed, i.e. every two years. During this period, the lubricant loses its original properties. In Russian conditions, service intervals must be significantly reduced and an inspection must be carried out as soon as a strange noise appears, the machine starts to run or any of the above signs of damage to the mechanism appear.

The high loads to which the gripper is exposed require the use of special lubricants. Inferior mixtures harden quickly and are destroyed by water or aggressive brake fluid. Only high-temperature, moisture-resistant, and chemical-free lubricants should be used. In addition, the right grease must be compatible with plastic and rubber parts. A special lubricating grease is used for the pins – the guide elements of the mechanical mounts.
Summary
The brake caliper is a technically complex component. It works in an area with high loads and temperatures - with aggressive driving, these can reach 500-600 degrees Celsius. The mechanism therefore requires regular maintenance. Otherwise, it may block unexpectedly on the road.
Change the brake fluid at least once a year, regardless of mileage. Otherwise, a critical amount of water will accumulate, which will quickly lead to corrosion of the printing plate. Check your brake discs and pads regularly and replace them in good time - especially before a long journey! Timely replacement of worn and damaged parts, regular lubrication will significantly increase the life of the caliper.
production form.
O 15, 25, 30, 40, 50, 60, 70, 80, 100 ml in orange glass vials with screw caps, closed with polymeric stoppers or caps, or polymer caps with sealing elements, or with polyethylene stoppers or 'Topaz' stoppers and polymeric overseals or 'Topaz' caps, or in orange glass vials, or 100 ml in orange glass vials, closed with 'Topaz' screw closures and caps or aluminum caps, or 15, 25, 30, 40, 50, 60, 70, 80, 100 ml in polymer vials closed with polymer stoppers or caps and polymer caps or polymer caps with gasket elements.
250 ml in glass vials closed with caps.
Each vial, jar and instructions for use should be placed in a consumer carton or cardboard package. The vials, jars can be put in a package (cardboard box) with the same number of instructions for use.
The bottles and glasses are labeled with writing paper or stationery or with an adhesive label.
Storage tips
Shoes are best kept in the boxes in which they were purchased. We do not recommend packing them in plastic bags - the natural materials inside cannot breathe. It is therefore best to choose boxes with openings that also allow ventilation.
In order for the boxes to keep their shape, manufacturers recommend putting washers inside - preferably made of wood, but also made of plastic or foam. We do not recommend putting newspapers inside the boots as they can disrupt the shape and rub off the paint on the inside.
Winter boots should be stored in a dry place away from heat sources. Placing them near a radiator will dry out and crack the skin. Balconies are also not the best choice as the air temperature there is volatile and this can lead to mould.

When storing shoes, it is advisable to cover them with pieces of paper so that the leather surfaces do not come into contact with each other, which can lead to abrasions and loss of shape.
Special properties of the materials
Each material has its own special cleaning and storage properties that we must not overlook:
- suede shoes. They are best cleaned dry with a brush and cleaning foam. To avoid abrasion, the pairs should be separated with a soft cloth when stored.
- leather shoes should dry for at least 12 hours after washing, preferably even longer. To keep the color, apply a shoe cream or polish after drying. Wait for it to fully retract and then remove it.
- Care of nubuck shoes It requires special care - it is moisture-averse. Use a special nubuck eraser to remove small stains and a cloth dampened with warm water and 2-3 drops of ammonia to clean large stains.
All of these tips are simple and inexpensive, but your winter boots are sure to serve you for several years with proper care.
If the inflammation in the breast has already started
There is another possibility when there is no obvious seal but there is pain and redness of the skin. It could be galactophritis, i.e. inflammation of the milk duct.
The reddening of the affected area indicates an incipient inflammation. The engorgement is very slight and is not in the lobules but in the duct.
This type of inflammation is the most dangerous because it develops imperceptibly and is not immediately noticeable. Within the first twenty-four hours of noticing the problem, milk may change: pale yellow, thick, like butter or jelly.
'Jelly milk is also a sign of inflammation. It's not a simple engorgement, it's mastitis!
Ordinary engorgement, where milk has lodged in the milk lobe, can develop into mastitis after three days. However, it rarely lasts that long.
Another sign of inflammation can be an elevated body temperature. However, it is not uncommon for a high fever to accompany the congestion from the start. This is because protein from milk enters the bloodstream.
With inflammation, the temperature can rise up to 37 degrees, which is not a good sign.
The temperature returns to normal within a few hours or a day after the congestion flap is drained.
Fever is not a contraindication for breastfeeding! And the baby can't 'poison' the milk if it already has an infection. This is what the World Health Organization is trying to tell healthcare professionals about in the document 'Mastitis. Causes and Management' (2000)!
But it can be a lot worse for the mother if she stops breastfeeding!
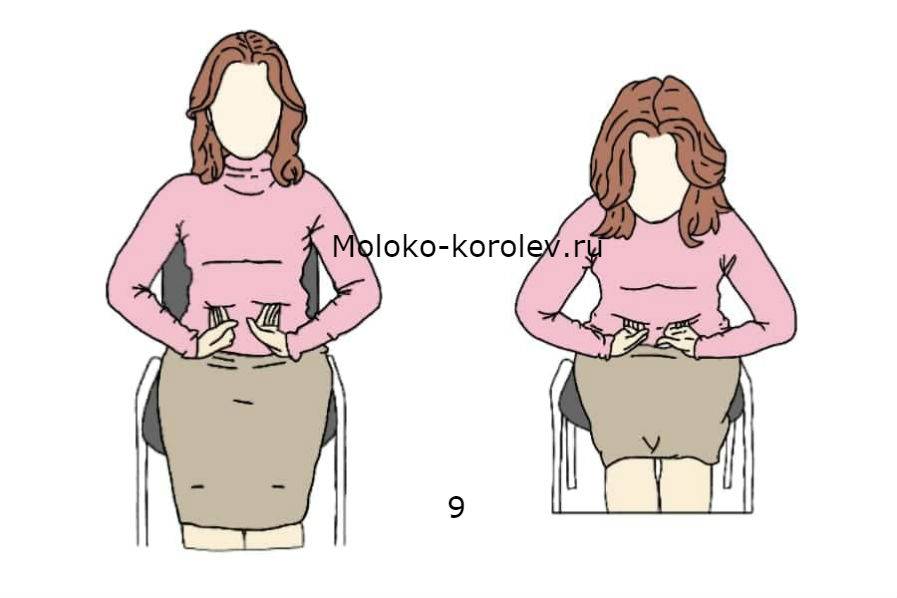
What causes engorgement in a breastfeeding mother?
Breast engorgement is very uncomfortable. Sometimes the mother feels so bad that she finds it difficult to breastfeed her child.
That is why it is better to know the causes of this painful condition.
In most cases it is due to the way breastfeeding is organised:
– insufficient feeding,
– deformation of the nipple when sucking,
– Irregular breastfeeding (one breast every 2-3 hours),
– Hyperlactation (which can also lead to extra pumping),
– cracked nipples where the shell covers the tubules,
– Rapid introduction of supplementary food,
- sudden cessation of breastfeeding.
The causes can lie in the care of the breast:
– Prolonged compression of the breasts (tight underwear, sleeping on the stomach),
- Mechanical trauma to the chest (e.g. contusion).
Less often, congestion is related to the mother's organism:
– Lipid metabolism (a blocked milk duct often looks like a small white dot on the nipple because a plug has formed),
– Maternal illness, stress, fatigue.
A lactation consultant can help minimize the risks. She will teach you how to breastfeed your baby well and show you different breastfeeding positions. She will tell you what you need to improve on the organization and variety of breastfeeding and what precautions you can take if you are a heavy breastfeeder.
Insertion of tampons with medication
Treatment of diseases of the female reproductive system can be topical or general. With topical treatment, the focus of the disease is acted upon directly, which is done in various ways. One of them is the use of cotton swabs soaked in medication.
- Nonspecific inflammatory diseases of the vagina, colitis;
- specific vaginitis caused by certain sexually transmitted infections - mycoplasma, ureaplasma;
- bacterial vaginosis – vaginal dysbacteriosis with suppression of lactobacilli and replacement with opportunistic microflora (Gardnerella);
- vaginal candidiasis (thrush);
- endocervicitis (cervicitis);
- erosion of the cervix;
- vaginal fistulas.
Advantages of topical treatment: the drug acts directly on the focus of inflammation to produce an effect. Only a small part of the drug enters the bloodstream. Therefore, the risk of side effects is lower. However, we typically combine therapeutic tamponades with oral medication and injections to achieve optimal results.
We also use therapeutic tamponade as an additional treatment for other inflammatory diseases of the urogenital tract. This includes:
In these cases, the drug injected into the vagina diffuses and spreads to the uterus with adnexa, perianal tissue, bladder wall, and urethra.
How effective is vaginal tamponade?
We use this method as part of a comprehensive treatment plan when there is a pathological process in the vaginal vestibule and cervical canal. We achieve the greatest therapeutic effect with this safe and completely painless outpatient procedure, which is performed in the middle of the monthly bleeding cycle.
tamponade technique
The optimal time for a vaginal tamponade is in the middle of the menstrual cycle. Before the procedure, the bladder and bowel must be emptied and intimate hygiene carried out.
site tamponade The tamponade itself is performed on an outpatient basis in the treatment room of the gynecological center. The woman sits in a chair. After applying antiseptics, the vagina and the vaginal part of the cervix are exposed. For this purpose, the doctor uses a curved Simps mirror.
In the next step, mucus and pathological discharge are removed with a sterile swab inserted into the vagina on a cone. For the same purpose, antiseptic douching with sprays and vaginal baths are performed.
The doctor then uses tweezers to insert a sponge soaked in medication. Clean cotton wool is not used for cleaning and tamponing. When the cotton comes in contact with the mucous membranes, microscopic cotton fibers remain on the mucous membranes. Therefore, a piece of cotton wool is wrapped in gauze to form a ball of about 3 x 1.5 x 1.5 cm, the ends of which are a few centimeters long so that they can be easily removed.
All dressing material is sterile. Ordinary sanitary napkins are not suitable for this purpose, as they completely absorb the drug. We use ointments, creams and solutions as medication to impregnate the tampons. This includes:
- Vishnev's balsamic ointment;
- Levomecol ointment;
- Pimafucin antifungal cream;
- hydrocortisone ointment for inflammation;
- antiseptic solutions;
- Vegetable oils (olive oil, tea tree oil, rosehip oil, sea buckthorn oil).
All medicines are also sterile. The choice of medication is made individually depending on the clinical picture. The swab procedure only takes a few minutes. Thanks to the skillful approach of the doctor, the woman does not feel any pain during this period.
Read more:- Long legs, small body.
- Pronation and supination in anatomy.
- foot bone in Latin.
- How to amputate a leg.
- name of the fingers.
- lower leg prosthetics.
- The pubic ligament where it is located Photo.
- Why are the big toes crooked?.
