As a rule, significant swelling of the foot occurs shortly after such an injury. Patients with this type of foot injury are usually evaluated carefully because fractures of the elbow are often associated with breaks or dislocations in other parts of the foot.

- Why does heel pain occur?
- Where does heel pain occur?
- Clinically Relevant Anatomy
- mechanism of injury
- Conservative treatment
- surgical treatment
- diagnosis
- Treatment of foot cysts
- Causes of pain in the upper foot
- Pain in foot and swelling
- prevention
- General information
- classification
- Big toe: Other causes
- Prevention: Can bunions be prevented?
- What is a valgus deformity?
- Lateral thickening of the foot: causes of hallux valgus
- Treating a broken foot
- Rehabilitation after a foot fracture
Why does heel pain occur?
The most common cause of discomfort or pain is in the heel
- Trauma to the foot – sprain or tear of ligaments, damage to the fibrous capsule (joint capsule) and cartilage, and bone fracture. Sometimes the pain is quite bearable and the affected person can walk. However, over time, an inflammatory process develops, pain increases, the load on the limbs is redistributed, and the joints are constantly displaced. Ultimately, degenerative changes occur in the tissue of the foot.
- An inflammatory process that develops as a result of infection or autoimmune disease of the joint tissue. When the immune system is weakened, pathogens can easily enter the body. A similar problem occurs with skin injuries. Synovitis, septic arthritis, osteoarthritis and bursitis can be caused by tuberculosis or the invasion of pus pathogens. If a malignant tumor develops in the body or a nidus of chronic infection persists over a long period of time, the immune system fails. The result is an autoimmune disease. Influenza, infectious diseases of the digestive, urinary or genital tract can trigger reactive arthritis. Other causes of inflammation of the foot tissues include fever, hypothermia, poisoning and cathartic injury to the ENT organs.
- Metabolic problems can also cause heel pain. In gout, for example, uric acid levels rise and accumulate in the joints. This process eventually leads to arthritis. Diabetes primarily affects the nerves and arterioles – the small blood vessels. As a result of impaired blood circulation, the feet lose sensitivity and the risk of injury increases.
Where does heel pain occur?
Pain in the heel can occur if one of the following pathologies is present:

- Fracture of the heel bone (old or recent), undetected fracture, osteoarthritis, osteochondropathy (aseptic necrosis of bone cellulose), tuberculosis, malignant tumor. If the bones adjacent to the heel are damaged, the pain may radiate into the heel.
- Damage to the joints (osteoarthritis, arthritis), consequences of wearing uncomfortable shoes, excessive stress on the feet. In gout patients, the joints on the inside of the foot (next to the talus, scaphoid and heel bone) or on the outside of the foot (between the ulna and heel bone) are affected.
- Ligament injuries – tendonitis (dystrophy or tendinitis), sprains, strains. Spurs, epiphyses, spikes – all of these can put pressure on the soft tissues. Injuries can affect the ligaments of the ankle joint. If the Achilles tendon is injured, the pain can spread to the back and top of the heel. When the synovial sac surrounding the tendon becomes inflamed, synovitis occurs.
- Diabetes, which attacks the blood vessels and nerves. The walls of blood vessels (angioedema) or nerves (neuritis) can become inflamed after an injury. Vascular changes can also occur in immune diseases, tuberculosis and bone inflammation.
- Wounds, cracked heels, burns and fungal infections can also cause pain. When a person loses a lot of weight, the subcutaneous fat melts and the bones press on the skin, causing pain.
Clinically Relevant Anatomy
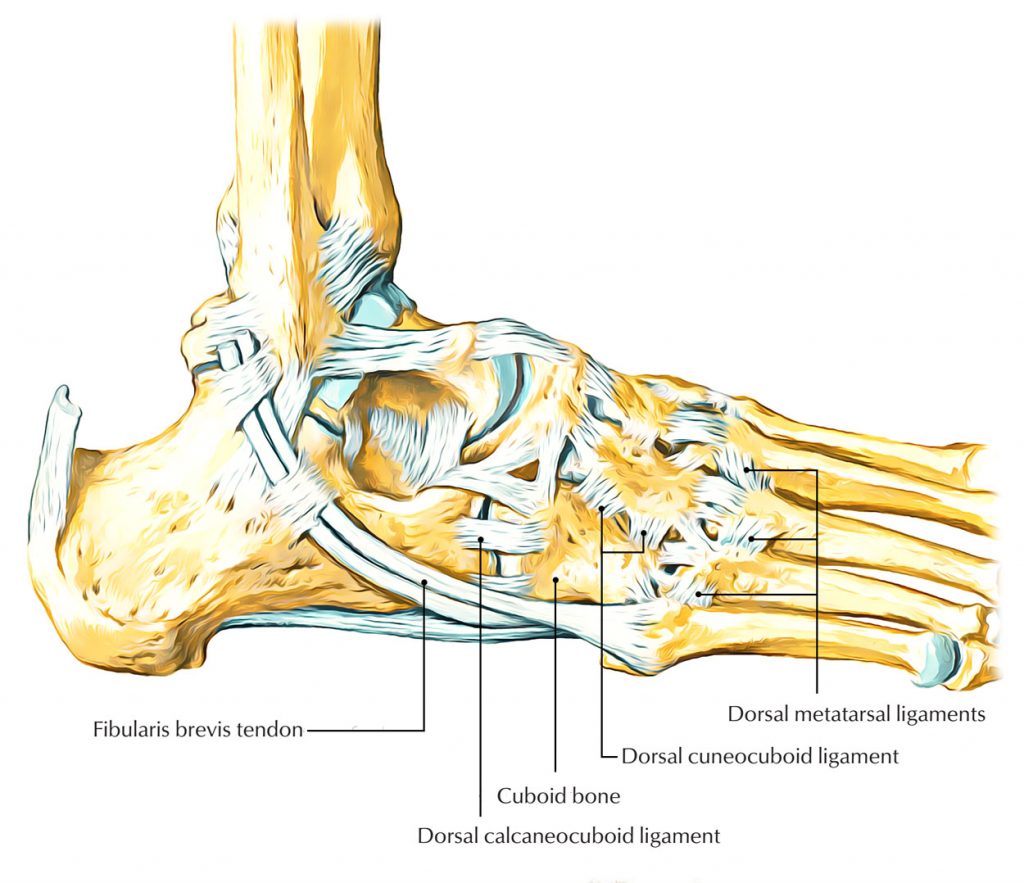
The elbow bone is a pyramid-shaped, short bone in the lateral side of the foot with six sides. It meets the 4th and 5th metatarsals anteriorly, the lateral talus and calcaneus medially, and the calcaneus posteriorly. The function of the pastern joint depends on the mechanics of the tarsal transverse joint, as the heel bone and the elbow bone move together when walking. The mechanics of the ankle are very diverse. The main movement in the ankle/foot joint is medial-lateral rotation about the anteroposterior axis, with the tuberosity of the calcaneus serving as the fulcrum. In inversion/reversion, the elbow bone rotates 25° about an axis running from the posterior to the anteroposterior side of the tarsal bone, with a movement of approximately 52° (43° to 72°) relative to the base. In addition to the inversion/inversion, this is evidence that the calcaneus-thigh joint is also stretched backwards and forwards when walking.
The ankle-foot joint is essentially unchangeable when its articular surfaces and tendon attachments are aligned. When standing, the ankle joint is radiologically largely congruent. The posterior and medial ligaments of the ankle and ankle as well as the wedge-shaped fibrocartilage tendon sheaths within the ankle and ankle contribute to stability and maintain balance. The long fibrocartilaginous tendon, which wraps around the elbow medially and laterally until it connects to the first metatarsal bone and the medial epicondyle, also contributes to the stabilization of the ankle joint. The elbow bone is the pulley for the tendon of the long fibula muscle; contraction of this muscle during the metatarsal gait cycle causes the elbow bone to straighten. Eversion of the elbow by the long fibular tendon can facilitate load transfer to the entire forefoot during a position change.
mechanism of injury
Two mechanisms of injury have been proposed:
- Injuries associated with flexion and inversion of the foot: With rapid flexion and inversion of the foot (a mechanism of dislocation of the transverse ligament of the ankle), a strong reflex contraction of the long calf muscle occurs. The ankle acts as a fulcrum, and the tendon transfers the load to the ankle, resulting in a downward-medial displacement, i.e. subluxation of the ankle.
- Overuse syndrome: This mechanism is poorly characterized and rarely observed, but there is evidence that ankle subluxation occurs as a result of repeated microtrauma (when returning to intense activity).
- instability of the joint of the tarsal bones to each other;
- excessive weight bearing;
- inadequate or poorly designed orthotics or shoes;
- movement (intensity, duration, frequency);
- movement on uneven surfaces;
- sprains of the foot or ankle;
- Ankle syndrome may predominate in patients with pronated foot due to increased strength of the long fibular arm.
Conservative treatment
Patients with isolated fractures of the elbow with little or no displacement should be immobilized with a short cast to allow weight bearing on the extremity.
In these cases we recommend immobilization for 6-8 weeks.
After immobilization is complete, the plaster splint is replaced with an orthopedic shoe and the foot can be put under some weight again.
Return to normal footwear will depend on the severity of pain and residual swelling, as well as the presence of radiographic signs of healing.
In most cases, patients begin wearing regular footwear 8-12 weeks after the injury.
surgical treatment
The treatment tactics for displaced fractures of the elbow are still controversial, as there is no consensus on how severe the displacement must be for the fracture to definitely require surgical treatment.
Most doctors agree that the elbow bone is an important stabilizer of the lateral column and that changes in the length of the lateral column inevitably lead to foot deformity, flat feet and pain.
The most common deformity caused by a compression fracture of the elbow is a shortening of the lateral column, so any surgical procedure should aim to restore this lateral column length.
Various surgical techniques are available. In our practice, we restore the length of the lateral column by internal fixation of the fracture with plates and screws and, if necessary, by bone grafting with supporting autographs from the iliac crest.
The results were good in all patients, so we use this treatment method for all fractures of the scaphoid bone that are associated with deformation of the articular surface.
In fractures with multiple fractures, bridging osteosynthesis with a plate may be the only option to restore the length of the lateral column of the foot. If the fracture is associated with severe soft tissue damage, external fixation may be the only treatment option. Regardless of the immobilization technique used, the main focus must be on maintaining the length of the lateral column of the foot, without which normal form and function of the foot cannot be restored.
Bone deficiency fractures or stress fractures of the elbow are usually characterized by the progressive development of pain on the outer edge of the foot that worsens with physical activity.
diagnosis
X-rays are the main method for diagnosing bone cysts. The photographs are taken in 2 projections, and the lesions discovered correspond to benign tumor-like masses. The cysts appear as round tumors less than 5-6 cm in size that are separated from healthy tissue. The cortex is removed and there is no periosteal reaction. Arteriovenous cysts usually have a 'soap bubble' appearance, while solitary cysts are always unilocular.
It is important to differentiate cysts from other tumors and foot bone diseases, as the effectiveness of treatment depends on this. Therefore, additional ultrasound, CT and MRI examinations may be recommended.
Treatment of foot cysts
Bone cysts can be treated conservatively or surgically. Conservative treatment focuses on puncture, that is, puncture of the cavity with aspiration of the contents and subsequent rinsing with medication. These are used for small tumors and are carried out under local anesthesia. However, large cysts on the foot do not respond well to such procedures and often require surgical removal.
In children, attempts are made to postpone surgery for calf cysts and talar cysts until the growth plates have closed. However, if there is a great deal of training, a clear risk of a pathological fracture, persistent pain and other complaints, it can be recommended for adolescents. In adults, if there are no complications, the operation is carried out as planned. Emergency surgery may be necessary only for amputated and open fractures, as well as for damage to nerve endings and blood vessels, which is accompanied by the development of compartment syndrome.
Conservative treatment can be used for uncomplicated fractures of the heel bone, especially in children. This consists of immobilizing the limb with a plaster cast, immobilizing the leg from the knee to the fingertips. It is also advisable to limit physical activity for a month. When walking, patients must always use walking aids (crutches, canes) to reduce axial pressure on the heel. A control x-ray is always taken after one month to assess the changes in the cyst cavity. If there are signs of a positive development, further x-rays will be taken at regular intervals. If the cavity closes gradually, surgery is not necessary.
If a metatarsal bone cyst is diagnosed, immediate surgery is usually indicated as conservative treatment is ineffective.
A heel bone cyst, like most similar tumors, is removed through a marginal resection. The resulting defect is then filled with a bone graft. Excision can also be done by scraping the defect with a blunt spoon and then bone grafting.
Causes of pain in the upper foot
Feeling unwell at the end of the day is normal for people who exercise a lot. Being overweight can also be a risk factor - the extra weight puts additional strain on the bones and joints. In addition, poor fitness leads to painful pain in the back of the foot because the body is simply not used to increased activity during the day. Doctors also identify other risk factors:
- Gout;
- osteoarthritis;
- Arthritis of varying severity caused by infections, e.g. b.
- flat feet;
- heel spur;
- Broken bones, dislocations, bruises;
- wearing tight shoes, including those with narrow toes and high heels.
In addition, pain in the upper part of the foot is common in women because the calcium content in the body decreases during menopause.
Pain in foot and swelling
Self-diagnosis of the cause of lower limb discomfort can now be carried out using online self-diagnosis. However, only the suspected cause of the symptoms is stated; Only the doctor should make the final diagnosis. For example, if you have pain and swelling in the upper part of your foot, your doctor may tell you during your initial exam that the discomfort is caused by medications, such as: b.
- hormonal oral contraceptives;
- drugs that lower blood pressure;
- adrenal medications;
- antidepressants.
Upper foot pain with swelling around the joints can also be caused by:
- infectious processes in the lower limbs;
- impaired drainage of lymph fluid;
- fatigue and insomnia;
- kidney disease;
- Obesity;
- insect and animal bites;
- allergic arthritis.
prevention
To prevent foot pain, doctors recommend:
- Swimming, jogging, cycling, skiing, walking more;
- warm up your foot before training;
- Wear sports shoes and change them every six months;
- Rest your feet if you feel pain and fatigue;
- walking barefoot on grass;
- Buy shoes in the afternoon when your feet are slightly swollen;
- Make sure your shoes are comfortable and don't pinch;
- Wear tight shoes or high-heeled sandals less often.
The 5 phases of treatment in the health workshop

A medical advisor will ask you about your symptoms, choose the right doctor, inform you about the cost of treatments and arrange an initial appointment.

Do you need an appointment with a neurologist, orthopedist or rheumatologist but can't come to the clinic? The doctors of the health studio are ready to conduct an online consultation.
A comprehensive examination by a neurologist or orthopedist, during which the doctor takes a medical history, reviews test results, or makes a diagnosis, will make an initial diagnosis. *For a free consultation, please contact the clinic's consultants or call +7 (812) 421-70-36.
To achieve a quick result and ensure maximum patient safety, we carry out the diagnosis and prescription of treatments comprehensively. The patient can undergo multiple treatments on the same day.
General information
The name is derived from the Latin equivalents 'osteon' and 'myelos', meaning 'bone' and 'bone marrow' respectively. The ending 'it' indicates inflammation.
Statistics show that osteitis is the third most common musculoskeletal system disease after trauma and surgery. It occurs in 6-7 % of patients.
The disease mainly affects the hip, shoulder, lower limbs, spine and jaw.
Pathology is more often diagnosed in young men, children and pensioners. Females are rarely affected.

classification
The international community has adopted the following classifications non-specific and specific To form.
The first is caused by pus bacteria (streptococci, Escherichia coli), sometimes fungi. The second form is characteristic of tertiary syphilis, tuberculosis.
The pathogens get into the bones in various ways - among other things endogenous (blood-forming) and exogenous. The pathogens come from the source of the infection (abscess, cellulitis, tonsillitis, dental caries) via the blood. External mechanisms include introduction following trauma (gunshot, fall from height), surgical intervention, and spread from surrounding tissues.
Exogenous and endogenous osteitis differ symptomatically in the initial phase. The clinical picture gradually flattens out.
The following types of external forms are distinguished:
- Post-traumatic (develops after open fractures);
- Contact (the inflammation spreads from the surrounding tissue to the bone)
- Postoperative (poor quality, non-compliance with aseptic and antiseptic principles, application of spikes);
- Gunshot wound (after firing a shot).
The course of the disease is initially acute. As a rule, the patient recovers completely, rarely the process becomes chronic and the affected person becomes disabled or dies from sepsis.
In the atypical course there are no obvious symptoms. The process initially becomes chronic.

Big toe: Other causes
If the big toe is swollen, the cause may be more than one valgus deformity. Other diagnoses are:
- Gout. It is caused by the accumulation of uric acid salts in the joints and manifests itself as severe, sudden pain. The attack can last up to 5 days and is one of the main symptoms to distinguish gout from hallux valgus.
- Rheumatoid arthritis. Affects all joints and parts of the legs. Symptoms include calluses on the soles of the feet, deformities of claws on the toes. The 'ball' typical of hallux valgus is rarely present.
- Osteoarthritis of the big toe joints, hallux rigidus. Symptoms include pain at the base of the phalanges, swelling of the big toe, subcutaneous protrusions, and tuberosity.
Despite the differences, it is difficult for patients to differentiate hallux rigidus from gout and osteoarthritis. A consultation with an experienced orthopedist can be helpful. The doctor will diagnose the problem, examine x-rays, make a diagnosis and suggest treatment.
Prevention: Can bunions be prevented?
Simple preventive measures can reduce the risk of bunions developing into thickened, deformed bunions. Patients are recommended to:
- to eat healthily – avoid obesity, vitamin and mineral deficiencies;
- Wear comfortable shoes and orthopedic insoles so that the joints are always in the correct position;
- Exercise – to strengthen the muscles and ligaments in the legs.
At the first signs or suspicion of pathology, it is important to immediately consult a doctor, undergo an examination and start treatment.
What is a valgus deformity?
A valgus deformity is described by patients as a thickening on the inside of the foot. However, medically, the pathology is defined as a progressive, complex condition associated with deviation of the first toe and loss of stability of the bony structures of the forefoot.
- The abnormal load on the foot leads to a weakening of the musculoskeletal system.
- The bases for walking and standing for long periods have changed.
- The forefoot bones fan out.
- An imbalance occurs in the strength of the muscles that are responsible for the correct position of the big toe.
- The first toe deviates outwards and the metatarsophalangeal joint deforms.
The patient describes these changes as if 'a lump had popped out and grown on the foot'. This is indeed the case. Without treatment and preventative measures, the bunion of the big toe will enlarge, causing pain, discomfort and further curvature of the ankles.
Lateral thickening of the foot: causes of hallux valgus

Thickening on the side of the inside of the foot can occur in both children and adults. However, it is more common in women over 30 years old. Typical causes for the formation of a toe bunion are:
- Heredity – genetically inherited weakness of the ligaments and tendons.
- Obesity – excessive stress on the feet, which leads to deformation of the joint and connective tissue.
- Hormonal disorders – changes in the body that affect the strength of the joints.
- Osteoarthritis – degenerative joint damage with halus valgus as an accompanying diagnosis.
- Poorly fitting footwear - high heels and narrow toes shift the contact points from the normal to the pathological area, which leads to joint deformation and curvature of the big toe.
- Diabetes mellitus – the pathology is caused by a disorder of carbohydrate metabolism and blood supply to the feet.
- Certain professions - long and often irregular loads on the feet occur in salespeople, hairdressers, teachers, athletes and dancers.
- Mechanical injuries – severe trauma often leads to pathological joint changes.
Hallux Valgus is always a violation of the integrity of the connective tissue. For this reason, the disease is often preceded by the following diseases:
- Metatarsal head bursitis – inflammation of the joint capsule of the toe.
- Rheumatoid arthritis – disease of the big toe joint.
- Podagra – a disorder of uric acid metabolism leads to salt accumulation in the joint and affects the base of the first toe.
If a lump appears on your foot, you should not hesitate to go to the doctor. Under unfavorable conditions, the pathology develops rapidly and requires surgical treatment.
Treating a broken foot

Treatment for a broken foot depends entirely on the location, extent and type of injury:
- If the heel bone is injured without a sprain, the doctor will apply a plaster cast. This starts at the toe and ends at the knee. Particular attention should be paid to the longitudinal arch of the foot. On average, a plaster cast needs to be worn for several months. If there is a dislocation, a one-stage reduction is carried out first, then a plaster cast is applied. Osteosynthesis is often performed and is recommended 14 days after the injury. If the fracture is a fragment, an Ilizarov brace is used.
- Both repositioning and osteosynthesis are used for injuries to the tarsal bone, but skeletal traction is rarely used. A plaster cast is applied for an average of 3 months.
- If the fracture involves the phalanges or metatarsals, a bandage is required. This is stretched along the length of the knee joint.
- For multiple fractures, treatment is complex and lengthy, and sometimes surgery may be required.
Rehabilitation after a foot fracture
Swelling and pain may be present long after the bandage is removed.
For a speedy recovery the patient needs:
- Stretching massage of the foot and lower leg.
- Increased physical activity with mandatory physiotherapy. The exercises should be performed daily without skipping classes.
- Physical therapy.
- Wearing supinators. This condition is mandatory. If all the above measures are completed after three months, the person will have to wear supinators for at least 12 months, sometimes even longer.
Another common recommendation from trauma surgeons is to wear special orthopedic shoes. After removing the cast, it is recommended to wear them for six months.
Read more:- Pain in the heel bone of the foot.
- Anatomy of the heel bone.
- Pain in the long extensor of the big toe.
- Pain in the inner arch of the foot.
- Metatarsal tarsal bones.
- metatarsal bones.
- bones of the foot.
- dislocation of the foot.
