After receiving the test results and the examination picture, the specialist prescribes drug or physiotherapeutic treatment.
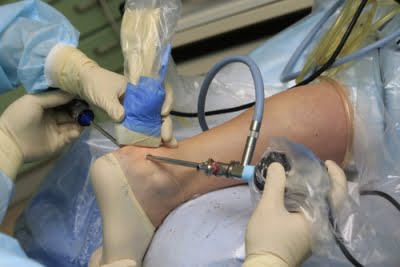
- Problems with the Achilles tendon
- Conservative treatment
- Immobilization of the ankle
- physical therapy
- Diagnosis of Achilles tendon bursitis
- Treatment of bursitis of the Achilles tendon
- Treatment of Achilles tendon enthesopathy
- Rehabilitation and prevention of Achilles tendonitis
- Classification of bursitis
- Popliteal bursitis
- Why does enthesopathy occur?
- Symptoms and diagnostic procedures
- signs
- shoulder
- Elbow
- Knee
- diagnosis
- symptoms
- diagnosis
- Clinical Significance
- inflammation
- degeneration
- Other animals
Problems with the Achilles tendon
Active people, especially those who play sports, often notice pain and swelling in the Achilles tendon area and the back of the foot. A pronounced 'lump', redness, persistent pain and swelling in the Achilles tendon area cause concern for patients.
Patients attribute this phenomenon to uncomfortable shoes, but this is only partially true. The cause is more complex and has to do with anatomical changes in the foot, such as: B. Flat feet or significant overload of the ankle or foot due to sporting activities.
The list of diseases affecting the Achilles tendon is quite extensive. These include Achilles tendonitis and tendinosis, synovitis and Haglund's disease, achillobursitis and many others.
Achilles tendon diseases are not as harmless as they may seem. Some of them can even lead to a rupture of the Achilles tendon over the long term.
In this article we will focus on the most common Achilles tendon disorders and explain what the Achilles tendon is and why it is needed, as well as what treatment options exist for patients with Achilles tendon and hindfoot problems based on the current state of medicine.
The human foot and ankle have a very complex structure. Together they form a unit and provide the human body with stable support when walking and running.
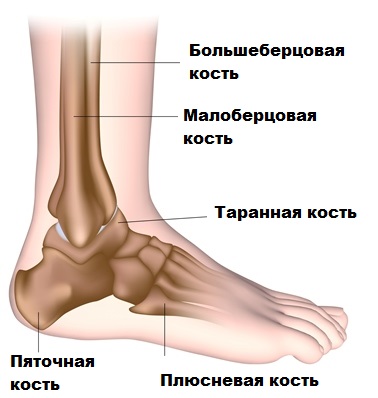
The ankle and foot are moved by many muscles and tendons, with the Achilles tendon playing an important role.
The Achilles tendon is the largest tendon in the human body. The tendon connects the calf muscle and the calf muscle to the heel bone.
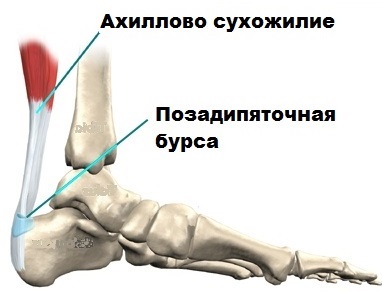
The Achilles tendon transfers the contraction force of these muscles to the heel bone, making it possible, for example, to stand on toes. Without the Achilles tendon, a person is unlikely to be able to jump, play sports, or move normally.
Conservative treatment
Nonsurgical or conservative treatment includes wearing heavily cushioned shoes, offloading the foot and ankle, physical therapy, and anti-inflammatory medications.
Corticosteroid injections are sometimes helpful, although this can be risky in terms of a future Achilles tendon rupture.
Custom-made insoles can be effective, especially when associated with flat feet.
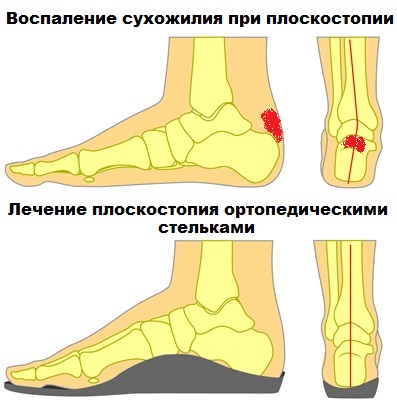
Unfortunately, the pain in the Achilles tendon area can be very persistent, making conservative treatment ineffective.
If conservative treatment is ineffective, surgical treatment is indicated.
Immobilization of the ankle
The injured foot should be rested as soon as possible. For mild sprains, this can be done with an elastic bandage or tape bandage. In more severe cases, the foot is immobilized with a special orthosis, a classic plaster cast or a modern plastic plaster cast. Proper immobilization keeps the foot in an optimal position with the toe extended so that the injured tendon ends are close together and can heal more easily. It is better to keep the foot in an elevated position to improve lymphatic drainage. Such immobilization should last at least 60-70 days.
The doctor recommends individual medication, taking into account the patient's age, concomitant diseases and, of course, the extent of the lesion.
- Painkiller. The orthopedist usually prescribes painkillers in the form of tablets or topical sprays to relieve the pain.
- Non-steroidal anti-inflammatory drugs. These are needed to relieve inflammation and swelling. NSAIDs are prescribed in short doses at the beginning of treatment, since degenerative processes take precedence in the subsequent pathogenesis.
- The doctor may inject a mixture of cortisone and a local anesthetic into the area around the inflamed area, which usually allows the medication to reach the lesion quickly and effectively. However, this penetration into the affected area must be done professionally. Overdose or injection into the tendon may increase the risk of rupture. Short intra-articular injections can be combined with medications in tablet form.
- Heparin injection. Until full loading is possible, thrombosis prophylaxis with low molecular weight heparin should be carried out.
- Once the bandage is removed, the doctor will prescribe venotonics to promote blood circulation and reduce swelling.
- In the long term, chondroprotectors can be administered to nourish the joints.
physical therapy
The first treatment for a sprain, bruise, or tear of the Achilles tendon is hypothermia. Cooling is indicated for the first three days. The foot can then be warmed (only if medically indicated!). More common physiotherapy shows excellent results once the pain subsides and regeneration of the damaged tissue is stimulated. Some of the most popular methods are.
Physiotherapy is particularly effective when combined with other techniques such as physical therapy (link to ort120619)
Diagnosis of Achilles tendon bursitis
Diagnosis of posterior and anterior Achilles tendon bursitis begins with an examination.
In the Posterior bursitis of the Achilles tendon The doctor looks for a red or flesh-colored swelling.
In the Anterior Achilles tendon bursitis The doctor presses on the space between the tendon and the heel bone, causing pain. Radiological examination Radiological examination A doctor can often diagnose a disease of the musculoskeletal system based on the history and physical examination. To make or confirm the diagnosis, an x-ray examination is sometimes necessary. More Information Bursitis cannot be diagnosed, but the doctor may do this exam to rule out other causes of heel pain, such as: B. a fracture of the heel bone or damage to the heel bone due to rheumatoid arthritis or other inflammatory arthritis.
Treatment of bursitis of the Achilles tendon
For both diseases - warm or cold compresses, non-steroidal anti-inflammatory drugs (NSAIDs) and injections of a mixture of corticosteroids and anesthetics
Both Anterior and posterior bursitis of the Achilles tendon Warm or cold compresses, NSAIDs Nonsteroidal anti-inflammatory drugs The most important medications for pain management are analgesics (pain relievers). The doctor selects a painkiller based on the type and duration of the pain, as well as the expected benefits and risks. Read more and injecting a mixture of corticosteroids and anesthetics into an inflamed pouch can temporarily relieve pain and inflammation. The doctor should be careful not to inject the mixture into the tendon. The patient should be able to rest after such treatment.
W Posterior bursitis of the Achilles tendon The aim of treatment is to reduce the severity of the inflammation and correct the position of the foot in the shoe to relieve pressure and shift the back heel. To raise the heel level and reduce pressure, pads made of porous rubber or felt are inserted into the shoe. It is advisable to use protective gel insoles placed on the painful joint capsule or to stretch the back of the shoe and place the insoles around the inflamed capsule. Until the inflammation has subsided, the shoe can be worn without the buttocks insert. Special shoes are sometimes used to control unnatural movements of the foot and heel that cause inflammation in the back of the heel. Other types of shoes contain insoles that reduce inflammation in the back of the heel and Achilles tendon.
If these treatments are ineffective, surgical removal of part of the heel bone may be necessary.
Copyright © 2023 Merck & Co, Inc, Rahway, NJ, USA and its subsidiaries. All rights reserved.
Treatment of Achilles tendon enthesopathy
Comprehensive conservative treatment. In the acute phase, when the pain syndrome is severe and the limb's support function is limited, it is recommended to limit the load and fix the ankle joint with an orthosis.
Drug treatment is aimed at eliminating pain symptoms, inflammation and swelling.
Physiotherapy: electrical stimulation, laser therapy, paraffin therapy, magnetic therapy, electrophoresis, percussion therapy - contributes to the restoration of metabolism, reduction of inflammation and restoration of blood circulation.
Extracorporeal shock wave therapy (EUVT) should be considered for poorly treated forms of Achilles tendon enthesopathy. With EUVT, low-frequency pulsed waves are administered in a targeted manner using a pocket applicator. Pulsed pressure wave is a safe, non-invasive method that stimulates metabolism and increases blood flow as well as repairs damaged tissue and accelerates healing. After just a few sessions, the pain can be quickly relieved and mobility of the ankle joint can be restored.
Kinesiology or biomechanical taping helps stabilize the joint, relieve pressure on the Achilles tendon, reduce swelling, and reflexively reduce pain.
Therapeutic exercises help to relieve tension in the calf muscles and restore mobility to the ankle joint.
In rare cases, hormone blockades or lidocaine blocks may be used due to possible side effects.
More recently, PRP injections have been widely used to treat epicondylitis and enthesopathy.
Rehabilitation and prevention of Achilles tendonitis
Rehabilitation of Achilles tendonitis begins at an early stage. Therapeutic exercises are aimed at stretching the calf muscles, strengthening the Achilles tendon, and restoring range of motion to the ankle joint.
Wearing shoe inserts or custom orthotics reduces pressure on the tendon and relieves pain. Even if only one of the heels is affected, insoles should be used for both heels to avoid biomechanical problems with walking and possible secondary pain in the hip, knee, and lower back.
For athletes, prevention consists in choosing the right footwear and a mandatory warm-up before training.
Do not self-medicate - the uncontrolled use of painkillers can cause the pathology to move from the acute to the chronic phase, involving the surrounding tissues and even the joint.
Classification of bursitis
Arthritic bursitis is divided into specific and nonspecific bursitis.
Specific means that it is caused by a specific pathology, a pathogen, e.g. B. Bursitis in tuberculosis, gonorrhea, syphilis, etc. Nonspecific means that there is no connection with a specific disease.
Depending on the contents accumulated in the synovial sac, the pathology is divided into: serous, purulent, hemorrhagic, fibrotic.
Serous refers to the fact that the exudate consists of plasma with a small amount of formulated blood components. Purulent means that the contents contain destroyed cells, microorganisms and dead white blood cells.
Hemorrhagic fluid contains large numbers of red blood cells.
Fibrinous synovitis refers to the presence of a large amount of fibrin in the fluid.
In addition, medicine distinguishes between aseptic bursitis and infected bursitis.
It is also divided into: knee bursitis, elbow bursitis, shoulder bursitis, hip bursitis and heel or foot bursitis. Each of these forms is explained in more detail below.
Popliteal bursitis
The knee is a large joint that is subjected to enormous stress every day, so it is not surprising that inflammation and injury can occur.
The former arise from constant trauma to the knee, gout or rheumatism.
Tendonitis is caused by inflammation of the muscles and tendons below the kneecap. It can be caused by a fall on the knee, a blow to the knee, or a tear of the meniscus.

Goosefoot is an inflammation of the inner or posterior joint wall. It hurts when you move, especially when climbing stairs. It occurs more often in overweight people.
Symptoms of knee bursitis: pain, swelling, tenderness on palpation.
Why does enthesopathy occur?
Enthesopathies often occur in the area of the joint where the same movements are carried out over and over again. This is the case with athletes and in certain professions. The most common forms of enthesopathy are:
- Achilles tendon enthesopathy. It occurs at the point where the tendon attaches to the heel bone. It occurs more often in athletes, athletes, people with a sedentary and overweight lifestyle.
- heel spur. A lowering of the portion of the tendon that attaches to the lower surface of the heel bone. This pathology is especially common among dancers.
- 'Tennis elbow (another common name is 'golfer's elbow'). This condition is also known as epicondylitis. The inflammation occurs at the tendon attachment point of the elbow as a result of frequent bending and stretching of the arm.
- The 'runner's knee – A condition that often occurs in people who walk or have to bend and straighten the knee frequently.
- Adhesive capsulitis in the shoulder – This is a thickening of the joint capsule of the shoulder joint, which causes pain and limited mobility.
Enthesopathy can occur as a manifestation of various pathologies, most of which are inflammatory in nature. The list of possible causes is quite long. Some of the possible causes are listed below:
- Infectious arthritis – Inflammation of the joint caused by an invasive pathogen.
- Ankylosing spondylitis (Bechterew's disease) – is a chronic joint disease that primarily affects the spine as well as the sacroiliac and pelvic joints.
- reactive arthritis – An inflammation of the joint that occurs in response to an infection, although the pathogens themselves do not penetrate the joint.
- Psoriatic arthritis (psoriasis) – Inflammation of the joints caused by psoriasis.
- Enteropathic arthritis – Joint inflammation caused by intestinal diseases (Crohn’s disease, non-specific ulcerative colitis).
Symptoms and diagnostic procedures
Pain in the affected joints, swelling and restricted movement. The manifestations depend on the cause of the enthesopathy and the place of origin.
After the examination, the rheumatologist prescribes an examination program, which may include the following tests and analyzes:
- General blood test, urine test. These provide information about changes that are characteristic of the inflammatory process in the body.
- If autoimmune diseases or systemic connective tissue diseases are suspected, immunological blood tests are ordered.
- X-rays, ultrasound, CT and MRI can reveal changes in the joint and surrounding tissue.
- If there is suspicion of an infectious disease or gout, the doctor recommends a puncture of the joint and a subsequent examination of the joint contents.
signs
- Pain, inflammation and swelling in the shoulder, elbow, hip or knee, which is particularly noticeable when the joint is stretched.
- Stiffness or limited mobility of the joint with or without pain.
- Muscle weakness due to pain. bursitis may cause pain and soreness in the area of the affected bone or tendon. The bursa may enlarge, causing difficulty in movement. Synovitis usually occurs in the shoulder, elbow, knee, and hip.
shoulder
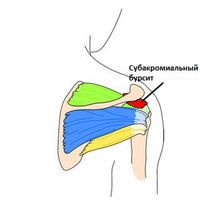
In the shoulder, the subacromial capsule (subdeltoid capsule) separates the tendon of the supraspinatus muscle from the underlying bone and deltoid muscle. Inflammation of this capsule is usually the result of injury to the surrounding structures, especially the rotator cuff. This condition limits shoulder mobility, causes impingement syndrome and is characterized by pain in the front and side of the shoulder. The discomfort occurs when you raise your arm above your head and put pressure on your shoulder.
Pain increases at night, shoulder mobility decreases, and pain appears in some areas.
Elbow
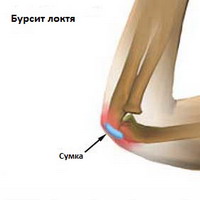
Bursitis at the tip of the elbow (olecranon) is the most common form of bursitis.
- Pain may worsen when bending the elbow as pressure on the capsule increases.
- This type of bursitis is most often post-traumatic and can be caused by both direct trauma and excessive rotation and flexion of the elbow (e.g. when painting).
- Infection is also quite common with this type of bursitis.
Knee
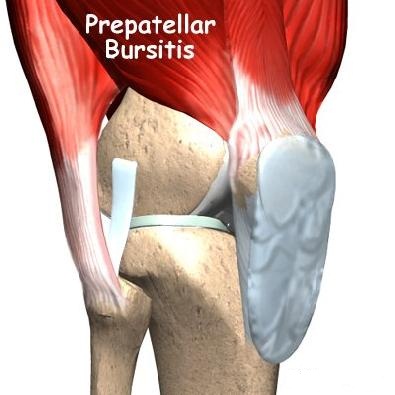
- Prepatellar bursitis Front part of the kneecap. The swelling in the front of the kneecap can be caused by chronic trauma (such as kneeling) or a blow to the knee. The swelling can occur within 7-10 days after a single impact to the area, usually after a fall. Prepatellar bursitis is also known as priest's knee or carpet cleaner's knee.
- Popliteal bursitis located in the area where the three main tendons of the inner knee are located. This type of bursitis is most common in patients with arthritis and is mostly seen in overweight, middle-aged women. Hamstring bursitis hurts when bending the knee and at night. At night, the pain forces the patient to sleep in certain positions, which reduces the pain. This bursitis is also characterized by increased pain when climbing stairs, which may radiate to the inside of the thigh. Bursitis is also not uncommon in athletes, especially long-distance runners.
diagnosis
The diagnosis of bunion relies on a combination of symptoms, clinical signs, history, and instrumental diagnostic methods. An anamnesis helps to determine the presence of underlying diseases.
To rule out other causes of pain, certain diagnostic procedures may be prescribed. These include the following diagnostic procedures:
- X-rays may reveal the presence of osteophytes or osteoarthritis.
- A sample obtained by puncturing an enlarged capsule (microscopy) can rule out gout and the presence of an infection. Synovitis in the knees and elbows is most susceptible to infection.
- Blood tests can rule out rheumatological diseases (e.g. rheumatoid arthritis) and metabolic diseases (diabetes).
- An MRI scan may be ordered if detailed morphologic imaging is required.
symptoms
The symptoms of the defect depend on the type and form of the defect.
Symptoms of achillobursitis include pain in the limb, swelling along the leg (especially near the connective tissue), redness, discomfort in the leg after sleeping, prolonged rest, pain when standing on tiptoes and jumping, as well as restricted movement and indecision .
The disease can occur in one or both limbs. If therapy is inadequate, the patient may stop walking.
Symptoms of TMJ disorder include pain and swelling in the heel area, redness of the skin, stiffness in movement, and discomfort with pressure. The progression of this type of disease to a chronic form is characterized by hardening in the heel area.
Symptoms of the posterior variant of the disease are characterized by swelling and inflammation of the posterior part of the ankle and limited mobility.
The acute phase is characterized by a grinding sound when moving, intermittent pain, the ligaments are significantly thickened and swollen and the affected person limps.
Symptoms of the chronic form include a 'blurry' clinic, a swollen appearance, a long-lasting pain syndrome and problems wearing shoes.
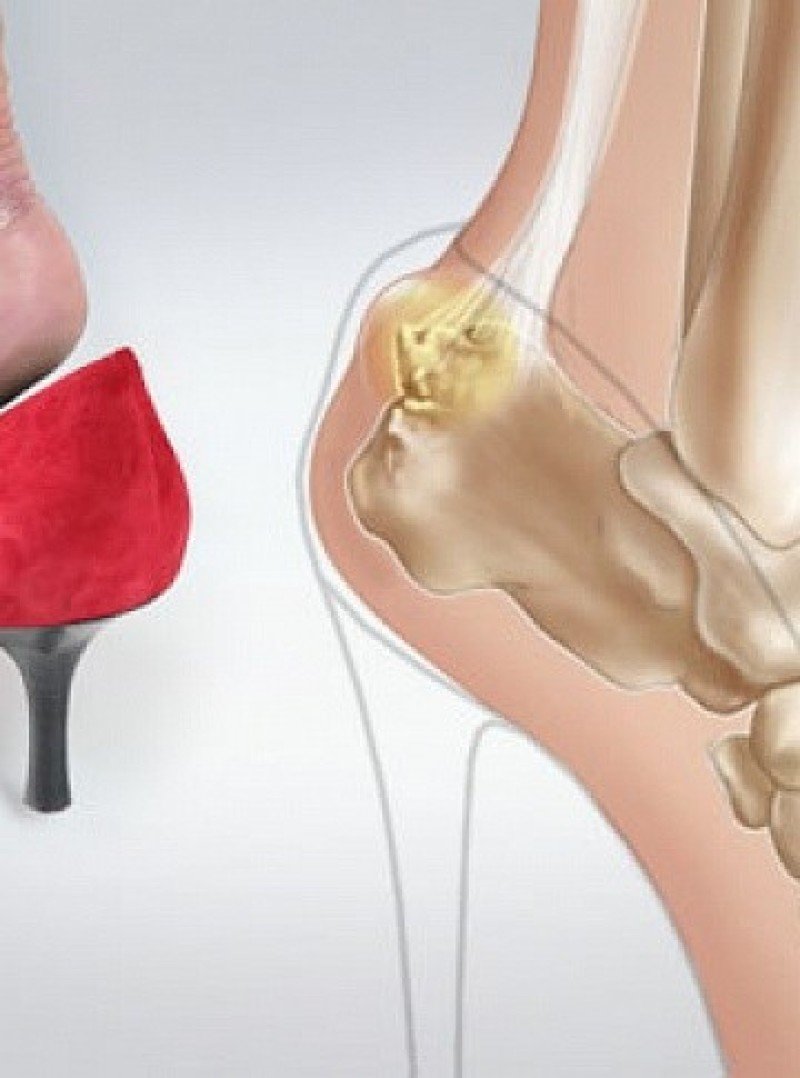
diagnosis
If you have swelling in the heel area or swelling of the lower limbs, you should make an appointment with an orthopedist or trauma surgeon. An examination by a physiotherapist is also required. The diagnosis is usually made on the basis of an initial examination. To confirm the diagnosis, blood tests (to rule out diabetes and gout), x-rays, ultrasound and MRI will be ordered.
Depending on the activity and severity of the occurrence, the doctor selects physiotherapy: anti-inflammatory creams and physical therapy are prescribed. Sometimes an examination by a surgeon is also necessary.
Various proven methods of folk medicine are used for effective treatment:
- Dry warming on a brick.
- Foot bath with pine needles.
- Alcohol tincture on lilac.
- Honey compress with vodka and aloe vera.
Clinical Significance
inflammation
Inflammation of the Achilles tendon is called Achilles tendonitis. Achilles tendonitis is pain or stiffness of the tendon that increases particularly with physical exertion and is usually due to overuse. [16] The most common symptoms are pain and swelling in the area of the affected tendon. [17] The pain usually increases at the beginning of the exercise and then subsides again. [18] Stiffness in the ankle joint may also occur. [19] The onset of the disease is usually gradual. [17]
It usually occurs as a result of overuse, e.g. B. when running. [19] [18] Other risk factors include injury, a sedentary lifestyle, high-heeled shoes, rheumatoid arthritis, and fluoroquinolone or steroid class medications. [17] Diagnosis is usually made based on symptoms and an examination. [18]
Although stretching and back-strengthening exercises are often recommended as prophylactic measures, the evidence for these measures is insufficient. [20][21][22] Treatment typically includes rest, ice, nonsteroidal anti-inflammatory drugs (NSAIDs), and physical therapy. [17] [19] A heel raiser or orthoses can also be helpful. [19] [18] If symptoms persist for more than six months despite other treatments, surgical intervention may be considered. [19] Achilles tendonitis is quite common. [19]
degeneration
Degeneration of the Achilles tendon (tendinosis) is usually examined using MRI or ultrasound. In both cases, the tendon is thickened and surrounding inflammation may be evident by the presence of paratenonitis, retrocalcaneal, or retroachillary bursitis. Increased blood flow, disorganization of the tendon fibers and small thickness tears can be detected in the tendon. Achilles tendonitis often affects the central part of the tendon, but can also affect the insertion, which is then referred to as enthesopathy. Although enthesopathy can be considered in the context of aging, it is also associated with arthritis such as gout and seronegative spondylitis. Achilles tendinosis is a known risk factor for calf muscle rupture. [23]
Other animals
With the exception of humans, the Achilles tendon is short or absent in great apes, while it is long in gibbons and people who live in trees. [36] It offers flexible energy storage when jumping, [37] walking and running. [36] Computer models suggest that this energy-storing Achilles tendon increases peak running speed by more than 80 % and reduces the cost of running by more than three-quarters. [36] It has been suggested that 'the lack of a well-developed Achilles tendon in non-human African monkeys prevents them from running effectively at both high speeds and over long distances.' [36]
The earliest known written mention of a tendon named after Achilles dates from 1693 by the Flemish-Dutch anatomist Philip Verheijen. In his widely published work Corporis Humani Anatomia He described the location of the tendon and stated that it was commonly referred to as the 'navel of Achilles'. [38] [39] The tendon was already described by Hippocrates, who called it the ' big tendon ' (Latin: big tendon ), and called the 'Hippocratic tendon' by later anatomists before Verheyen [39].
Verheyen was referring to the mythological tale of Achilles, who was held by his heel by his mother Thetis as she dipped him into the River Styx as an infant to make his body invulnerable. Since the heel by which she held him was untouched by the water, it was his only vulnerable spot (hence the term 'Achilles' heel'), and he was eventually killed by a poisoned arrow lodged in his heel. The name also refers to the particularly painful and disabling effects of an injury to this tendon. [39] The first closed crack was described by Ambroise Paré in the 16th century. [39]
The Achilles tendon is also called the 'heel tendon' (lat: Heel tendon (English). ). [39] Because eponyms (names that refer to people) are irrelevant to the topic, most anatomical eponyms also have scientific descriptive names. The term heel Bone comes from the Latin word calcaneum which means heel.
Read more:- cysts in the ankle.
- Heel bone human anatomy photo and description.
- Lamb Muscle Soreness.
- Pain in the heel bone of the foot.
- heel strike hurts.
- Latinized heel bone.
- dorsiflexion.
- Structure of the heel.
