Book a callback. We are there for you 24 hours a day, 7 days a week.

- Hereditary palmoplantar erythema and plantar erythema (Lane's disease)
- causes
- Which doctor should be consulted?
- Diabetic foot symptoms. Stages of the disease progression.
- What is gout on the feet of women?
- How to treat gout in Moscow?
- Warts (plantar warts)
- The appearance of plantar warts can be triggered by the following factors:
- Cracked feet
- Cracks occur due to:
- Swelling of the legs due to kidney disease
- Leg swelling in liver disease
- Photo of psoriasis on the legs, what psoriasis looks like
- The initial stage of psoriasis on the feet
- causes
- Symptoms of osteoarthritis of the foot
- What is gangrene?
- Causes of necrosis of the lower limbs in the elderly
- Treating swollen feet
- Prevention of leg swelling
Hereditary palmoplantar erythema and plantar erythema (Lane's disease)
Hand and sole erythema (Lane's disease, hereditary hand and sole erythema) is a genetically determined skin disease that combines a group of etiologically different processes with the common key symptom of irregular reddening of the skin.
The risk of erythema was not statistically significantly related to age or sex, but there was a clear familial pattern to the disease. As with most other hereditary diseases, the occurrence of palmar erythema and plantar erythema is relatively rare.
causes
As indicated in the nosological formulation, hereditary palmoplantar erythema and erythema oblongata are a genetic anomaly in which an abnormal network of venous-arterial anastomoses (connections) forms in the blood supply to the hands and feet. The result is impaired microcirculation and increased pressure in the arterioles and capillaries in the distal parts of the extremities, which is manifested by redness of the skin.
In some cases, Lane's erythrosis is not present at birth and manifests itself in adulthood or even in old age under the influence of specific triggers (most often poisoning or endocrine disorders resulting from gonadal dysfunction).
It should be noted that some sources also call immunoallergic mechanisms as triggers of hereditary erythema palmaris and erythema palmaris, while other authors exclude allergic erythritis from the concept of Lanae's disease.
Which doctor should be consulted?
An endocrinologist and a surgeon are the doctors to see at the first symptoms of a diabetic foot. The treatment often requires a comprehensive concept that may involve not only a vascular surgeon, neurologist and endocrinologist, but also an orthopedist, traumatologist, dermatologist and podiatrist. A series of measures should be taken and comprehensive treatment recommended to restore a comfortable life and pain-free mobility.
- Wearing tight, uncomfortable footwear that can cause blisters, corns, and other skin damage;
- Cuts, scratches, abrasions, insect bites and other mechanical injuries to the skin;
- minor cuts and wounds resulting from pedicures;
- ingrown toenails;
- cracked feet;
- Fungal diseases.
Diabetic foot symptoms. Stages of the disease progression.
People with diabetes need to be as careful and sensitive as possible about their own health. At the first changes in health and well-being, it is advisable to consult a specialist. The feet are a part of the body that also requires special attention.
It is advisable to see a doctor if the following symptoms occur:
- a feeling of running goosebumps on the feet
- Numbness and tingling in the lower extremities
- a burning feeling in the legs
- Cramps in the calves
- Hair loss on the lower legs
- Discoloration or discoloration (pale, red, or blue) of the legs
- Darkening of the nail plate (bruise under the nail)
- Cracking on the feet
- blistering eczema between the toes (small blisters with clear fluid inside)
- Injuries to the feet heal slowly or not at all
- itching
- swelling
- flaky, dry skin
Increased fatigue and pain in the legs at night and when walking can also be symptoms of gout.
What is gout on the feet of women?
In women, the natural processes of excretion and absorption of uric acid are disrupted, and urea levels in the blood rise significantly. This is due to insufficient production of estrogens, which occurs in women with menopause. Therefore, gout occurs more often in women over 50 years old, who have an acute deficiency of sex hormones and disorders in the endocrine system. The main symptoms are:
- tofu formation (accumulation of urate in the joint tissues);
- nephrolithiasis (accumulation of urate in the kidneys with subsequent formation of calculi);
- Gouty (uric) nephropathy.
How to treat gout in Moscow?
The rheumatologists at Yusupov Hospital know how to treat gout in the legs. When combating acute arthritis, doctors at Yusupov Hospital use several pharmacological groups at once:
- Nonsteroidal anti-inflammatory drugs (such as ibuprofen, indomethacin, diclofenac);
- Uric acid-lowering drugs – Anturan, Butadione, Cetazone;
- Corticosteroids (prednisolone, dexamethasone, triamcinolone).
Gout injections in the legs are used to relieve pain. The choice of medication depends on the patient's condition and his specific pain threshold, which is determined directly by the doctor.
As an additional treatment for gout, rheumatologists recommend applying an iodine mesh to the affected areas every night. This can reduce inflammation, speed up the remission process and reduce pain attacks. To enhance the effect, aspirin should be added to the iodine and the finished mixture should be regularly applied to the affected joints.
At Yusupov Hospital, physiotherapeutic treatments are actively used to effectively reduce inflammation, reduce seizures, prevent sodium urate stagnation, and repair affected joint tissues. For this purpose the hospital has:
- electrophoresis;
- phonophoresis;
- ultramonophoresis;
- heat treatments;
- magnet therapy;
- amplipulse;
- Ultrasonic.
Doctors at Yusupov Hospital draw up an individual diet program to exclude foods that trigger a gout attack. The hospital's rheumatologists prescribe therapeutic physical exercises to restore the previous mobility of the joints, normalize blood circulation and metabolic processes in the body, and strengthen the patient's muscular apparatus.
If you suffer from gout in your big toe and need treatment, contact the specialists at Yusupov Hospital. Doctors will carry out a comprehensive examination that will examine, among other things:
Warts (plantar warts)
The human papillomavirus (HPV) causes warts on the soles of the feet.
A plantar wart is essentially a benign growth in the form of a keratinized, yellowish or white patch of skin. At the beginning of growth formation, it can easily be confused with a black eye socket.
The nodule formation is easily confused with dry calluses or corns. The main difference from them is a sharp pain when the papilla is pressed. This can be explained by the presence of many deep roots in the optic disc leading to the nerve endings. This painful sensation can be compared to the prick of a thorn, hence the common name foam. A mature wart is characterized by the presence of many small black dots on its surface - these are the roots.
The appearance of plantar warts can be triggered by the following factors:
- uncomfortable, constricting shoes;
- excessive sweating of the feet;
- fungal infections;
- overweight;
- Flat feet, arthritis, arthrosis.
Unfortunately, it is not possible to remove plantar warts at home. Various wart removers can only remove the visible top layer of the wart. The roots remain and cause the same painful sensations. Therefore, in order to completely eliminate the warts, you have to resort to the laser method or cryoablation, which we have already written about above.
To prevent plantar warts, it is important to wear the right footwear and pay attention to foot hygiene.
Cracked feet
One of the most common foot problems in the older population is cracked heels. Cracked feet not only look unsightly, but they also cause a lot of discomfort and pain. And if the problem is not addressed in time, it leads to infection of the skin and triggers an inflammatory process.
Cracks occur due to:
- wearing uncomfortable, poor-quality shoes;
- Frequent contact with chlorinated water;
- lack of proper hygiene;
- Severe dryness of the skin;
- Deficiency of vitamins A, B and E;
- fungal infections on the feet;
- cardiovascular diseases;
- Diseases of the kidneys and digestive tract;
- Diabetes.
If the cracked heels are not caused by mechanical impact but by one of the causes mentioned above, you need to address the cause in order to effectively eliminate the problem. For example, if the cracks are the result of a fungal infection, the feet must first be treated with an anti-fungal agent and then the cracks themselves must be removed.
Treating cracked heels is complex. It includes hygienic treatments such as soothing foot baths, moisturizing creams and the use of special masks. In addition, vitamins A, B and E as well as magnesium and zinc should be included in the diet. Definitely avoid tight shoes and synthetic socks and avoid going to the swimming pool for a while. If you follow all the recommendations, you can get rid of the cracks after just a month of treatment.
Check out our readers' foot care tips. In her blog she describes her treatment method for cracked heels.
For easy walking without pain and discomfort, it is better to take preventive measures. And if you have at least one of the above-mentioned problems, you should not hesitate to address it and get it treated in a timely manner.
Swelling of the legs due to kidney disease
Swelling is caused by the development of kidney failure in acute or chronic kidney disease. Kidney disease can be latent for a long time, and even an examination cannot always detect it if it is not aimed at urinary tract pathology. In general, kidney failure is rarely detected in its early stages, but even if it is correctly diagnosed, treatment consists of lifestyle management with regular check-ups. Within a few years, the patient gets used to his diagnosis and has the grace to forget it. The course of renal failure is quite sporadic, and edematous syndrome, an important symptom, develops in just a few days.
Renal insufficiency can develop with any kidney disease or with 'kidney-related' complications of diabetes or systemic disease. It develops e.g. B. acute or chronic damage to the structural unit of the kidney - the glomeruli - which is referred to as nephritic edema. It is localized in areas of sagging subcutaneous tissue, starting with the face - this includes 'bags' under the eyes in the morning and thick, translucent eyelids, which patients simply declare, 'I drank my tea overnight', and therefore maintains it no need to burden the doctor with such a trifle.
As functional renal insufficiency worsens, the edema spreads rapidly and almost uniformly throughout the body, with the feet and lower legs appearing to swell, in contrast to the swelling of the heart, which subsides slightly in the evening but is present to an even greater extent the next day is. The swelling can go unnoticed for a long time because it is often accompanied by high blood pressure and decreased urine output. The whole person 'swells like a pillow'. – With anasarca, fluid appears in the cavities: abdomen, chest, heart. In this situation, hemodialysis and emergency treatment are required. The effectiveness of reducing edema depends on the results of treatment of renal insufficiency.
Leg swelling in liver disease
If liver function is impaired as a result of acute or chronic hepatitis of any etiology, the protein albumin is not produced in sufficient quantities and 'protein-free' edema occurs. In addition, any pathological process in the liver leads to the formation of scar tissue, which displaces the liver cells - hepatocytes. Scar tissue - fibrosis and liver cirrhosis - disrupts the normal outflow of blood through the venous system, and the abdominal and thoracic veins themselves are deformed by variceal nodules. There is an accumulation of fluid in the abdominal cavity - ascites - which further impairs blood and lymphatic circulation and leads to a persistent symmetrical and fairly dense swelling of the tissue, gradually increasing from the feet to the abdominal wall. Treatment of ascites syndrome is very difficult and ultimately rather ineffective unless a liver transplant is possible.
Involvement of vessels and lymph nodes is possible in some acute infections and malignancies, groin injuries and after surgical procedures or radiation from peripheral lymphatic collectors that 'suck' lymph fluid from a specific anatomical area. Lesions of the lymphatic system of the lower limbs are often referred to as 'elephantiasis' due to the similar shape of the leg. Lymphedema is characterized by high density and persistence as well as unilateral lesions. With the genetic defect of the lymphatic system, idiopathic lymphedema, the leg is affected on both sides, but always asymmetrically.
The swelling builds up gradually, starting with lymphedema, a soft enlargement of the hindfoot that eventually becomes padded and the toes become a completely normal size. The skin and fibers are gradually infiltrated by connective tissue and gradually replaced by scar tissue. The foot looks like a loosely sewn cotton trouser leg, with cracks and bars, rough folds, irregularly shaped pads and shallow depressions. A small skin wound takes weeks to heal and secretes clear lymph. An infection with Staphylococcus aureus can lead to purulent inflammation, which greatly aggravates the existing lymphostasis. The purulent inflammation often occurs in episodes, and with each exacerbation the soft tissue defects in the leg become larger.
Photo of psoriasis on the legs, what psoriasis looks like
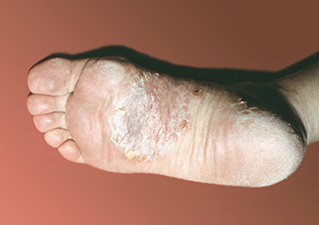
Photo 1.
Psoriasis on the feet.
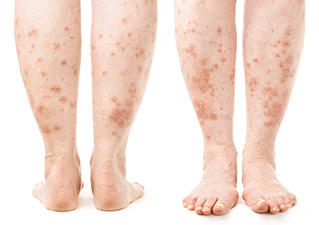
Photo 2.
Psoriasis on the legs.
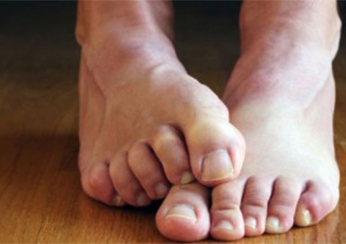
Photo 3.
Symptoms of psoriasis: Itching.
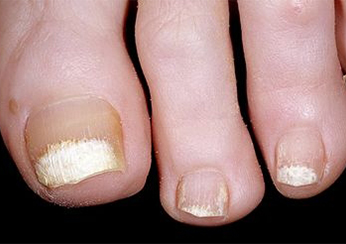
Photo 4.
Symptoms of psoriasis: Deterioration of nails.
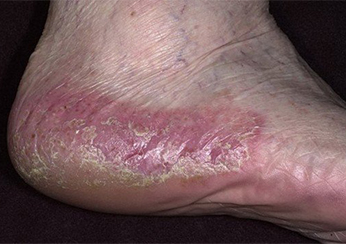
Image 5.
Psoriasis on the heels.
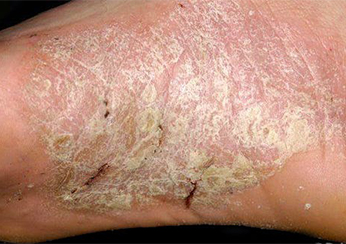
Image 6.
Cracked heels due to psoriasis.
To get an idea of what psoriasis on the feet looks like, you can view photos of the rash on medical websites. Detailed photos of psoriasis on the feet and allow you to examine the shape, appearance and peculiarities of the structure of psoriatic plaques.
The initial stage of psoriasis on the feet
The figure shows that the initial stage of psoriasis on the legs is similar to many dermatopathies, so it is sometimes confused with another disease and treated at home. The rash consists of pale pink papules with white scales on the surface. The subjective sensation in the form of itching is not characteristic of psoriasis, and pain may occur in the presence of cracks. In order to make a differential diagnosis between psoriasis and other dermatoses, specific symptoms are examined: In the progressive phase, the lesions intensify, become intensely pink, condense into plaques and are partially covered by white, shiny silvery scales. As the disease progresses, the area covered by the lesions increases and becomes completely covered by scales. Close contact with clothing causes itching and burning, as well as cracking due to dryness of the epidermis. In young children and when the rash is located in large folds of skin (intertriginous form of psoriasis), the syndrome is difficult to detect due to the rapid formation of scales.
The specificity of the clinical picture of psoriasis of the lower extremities depends on the localization and form of the disease. Vulgar or common psoriasis occurs more often in places that are in close contact with clothing and cause frequent rubbing: feet, backs of the knees and shins. The lesions are round or irregular in shape and tend to quickly merge into plaques. They are abundantly covered with white, silvery or gray scales, which flake off easily when rubbed or scratched. Local hypersensitivity, infiltration, itching and burning occur. Invasive psoriasis affects the volar skin surfaces and large folds: axillary, groin and intercostal folds, elbow and neck folds. A complex form of the disease that resembles various types of dermatitis and allergies. The rash is round, pale pink, possibly scarlet, and not covered with scales due to high humidity and active sweat glands. Moderate itching, burning and pain may occur. The exudative form can spread to the entire surface of the lower leg. The skin is covered with large, inflamed and moist plaques that are bright red in color. This form of psoriasis is characterized by dense, yellowish-gray scaly crusts on the surface of the lesions. Teardrop-shaped psoriasis is characterized by numerous small, reddish papules covered with silvery-white scales. In rare cases, this form of psoriasis causes the lesions to coalesce to form plaques. Erythrodermic psoriasis is the most severe form, with redness and infiltration of the entire skin. Pronounced peeling of the skin may occur. This form is characterized by an imbalance in the general condition of the patient, characterized by fever and general malaise.
causes
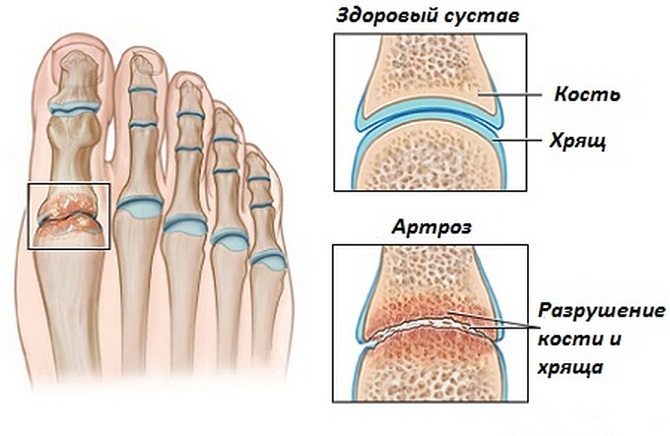
In most cases, arthritis of the foot arises from poor blood circulation in the joints, age-related mechanical wear and tear of cartilage and bone tissue, or trauma. There are the following possible causes of osteoarthritis:
- Specific foot structure: too wide feet, toe curvature, flat feet. Different leg lengths can also cause the problem.
- Excessive physical stress on the foot, especially in athletes or people who work hard.
- Injuries, bruises, fractures, bumps, torn ligaments, muscle damage.
- Frequent hypothermia of the feet.
- Excessive body weight, which increases stress on the feet.
- Mechanical breakdown of cartilage and bone tissue due to advanced age.
- Inherited predisposition.
- Wearing shoes that are too tight or too big, high-heeled shoes.

Other factors that can cause arthritis in the foot include:
- Endocrine abnormalities, disorders of the hormonal system;
- Insufficient intake of micro and macronutrients into the body;
- Chronic infectious lesions of the ankle joints;
- Allergic reactions, autoimmune diseases;
- Congenital dislocations or dysplasia of the hip joint.
Osteoarthritis cannot be completely cured, but the patient's condition can be significantly improved and complete deformation of the joints can be prevented. Therefore, treatment should begin as soon as the first symptoms appear.
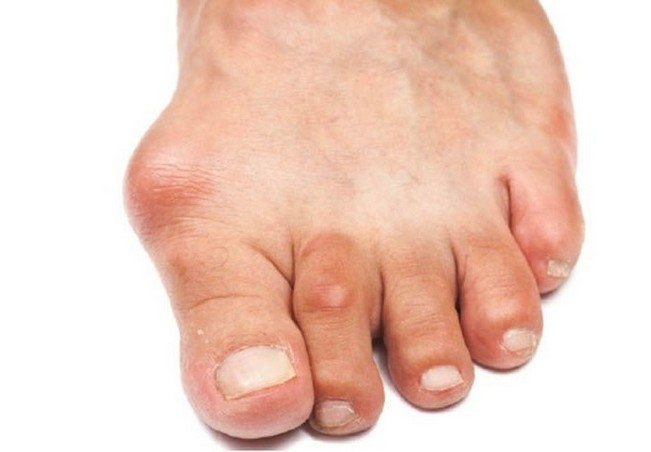
Symptoms of osteoarthritis of the foot
The pathology is manifested by the following symptoms:
- Pain in the foot after prolonged walking or standing and discomfort after physical exertion.
- Swelling and redness of the skin in the affected area. There may be an increase in local temperature.
- Painful reaction at the site of osteoarthritis to changes in the weather or contact with cold water.
- Crunching in the foot and ankle joints (occurs in the second stage of the disease).
- Excessively rapid fatigue of the feet.
- Limitation of limb mobility, muscle tension and stiffness, especially in the morning.
- Calluses on the soles of the feet.
- As the deformity increases, the patient may develop gait disorders over time.
Osteoarthritis of the feet also has the following symptoms:
- Pain in the joints of the feet that hurt, break or burn.
- Osteophytes (bony enlargements of the joints) can occur.
- The ankles get thicker.
Since osteoarthritis affects not only the bones and cartilage, but also the muscles, muscle cysts can be a sign of this disease.
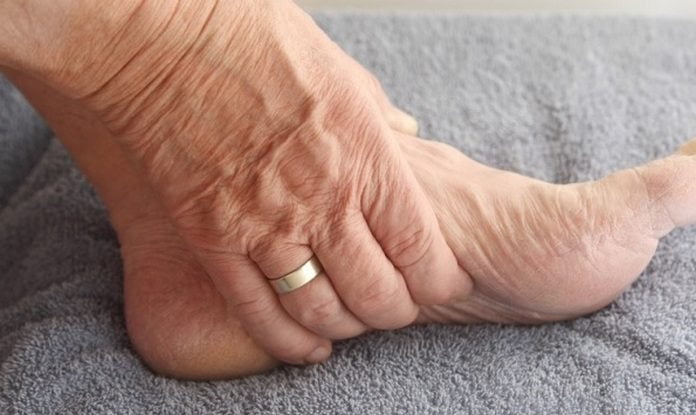
What is gangrene?
Gangrene is a necrotic tissue change (necrosis), a condition that develops as a result of impaired blood flow, its complete interruption in the damaged area and the development of a bacterial infection. The condition most commonly occurs in the lower limbs, affecting the toes, feet, or the entire leg. In some, particularly severe cases, damage to internal organs and muscle tissue occurs.
The onset of the disease can be recognized by the characteristic change in skin color - it begins to turn black and brown or blue spots appear. The skin becomes discolored due to the release of iron sulfide as a result of the destruction of hemoglobin. Depending on the symptoms and course of the dangerous disease, a distinction is made between dry and wet gangrene.
Causes of necrosis of the lower limbs in the elderly
- Mechanical damage to the outflow of blood (causing the dry type). The causative factors include a cast that is too tight, which compresses the soft tissues and hinders normal blood flow. Gangrenous lesions can be the result of pressure injuries caused by traffic accidents, stasis, exceeding the permissible time for applying a blood stasis seal.
- Diseases of the vascular system, heart – thrombosis, atherosclerosis and other pathologies.
- Bacterial origin of the disease. A non-sterile wound dressing, ingestion of streptococci, Enterobacteriaceae bacteria, etc. can provoke the appearance of pain.
- Thermal burns, chemical burns, frostbite can trigger an inflammatory process of an infectious nature, leading to disruption of blood transport.
- Mechanical injuries, the severity of which is aggravated by infections.
Necrosis in the elderly can be triggered by somatic diseases, reduced immunity, vitamin deficiency, alcohol addiction, smoking, sedentary lifestyle (immobility due to paralysis or amputation), hypothermia, poor health, age-related metabolic disorders and similar problems. The main risk is the loss of self-healing abilities due to a lack of nutrients in the body's tissues and insufficient oxygen supply. Even a small cut, wound or scratch can cause a non-healing ulcer that can become black and gangrenous.
Treating swollen feet

How to treat swollen feet? First of all, it is not necessary to treat only the swelling: without treating the cause, any treatment will only have a temporary effect and the swelling will return.
Only your doctor can tell you what to do if your feet are swollen. Only he can prescribe the most appropriate treatment based on all the analyzes and the patient's medical history. The process usually begins with conservative therapy, which can significantly improve the patient's quality of life.
If the examination reveals kidney or heart muscle abnormalities, the therapist will prescribe diuretic, antihypertensive and immunosuppressive medications.
Varicose veins, which cause permanent swelling in the legs, are treated with phleboprotectors and venotonics. These preparations can strengthen the vascular walls in the legs and normalize blood flow. Special ointments and compression stockings can relieve the discomfort caused by the parasite.
Joint disease also often leads to swelling of the soft tissues around the joints. If an X-ray shows abnormalities in the cartilage tissue, the patient is prescribed nonsteroidal drugs to relieve the inflammation. These can be ointments, tablets or injections. In some cases, the patient is also prescribed additional therapeutic treatments and massages.
For local infections, an antibacterial, antiviral, or antifungal agent is prescribed.
The benefits of lymphatic drainage massage should not be ignored. This treatment of the body contributes to the activation of metabolism and lymphatic drainage, which significantly reduces swelling.
In addition, the doctor may recommend a special diet. This is especially true for patients whose swelling is due to poor diet, being overweight or underweight. It is important to reduce the daily amount of fluids and limit excessive consumption of salty, spicy and fried foods. The patient needs to reconsider his daily diet and eat plenty of fresh fruits and vegetables. Dill, parsley and celery can be eaten for edema - a salad prepared with these herbs has an anti-edema effect.
Prevention of leg swelling

As with any condition, leg edema is easier to prevent than to treat its advanced forms. To do this, it is important to observe the following rules:
- Be responsible with your diet. The best solution is to eliminate all potassium-rich foods from your diet;
- Avoid uncomfortable, tight shoes;
- Pay attention to your feet when sitting: do not put too much pressure on your feet and make circles with them;
- It is important to massage your feet and legs regularly;
- Get into the habit of taking contrast showers;
- Don't forget to do physical activity: walk, swim and do aerobics to strengthen the muscles, blood vessels and ligaments in the legs;
- Sleep with a pillow under your legs so that they are at heart level. This way you can temporarily get rid of the swelling;
- It is important to leave all bad habits behind.
Leg health is something you only think about when uncomfortable and painful swelling has occurred. Well-planned doctor's visits, avoiding bad habits and eating right will ensure that your legs stay healthy for as long as possible!
Read more:- Treatment of a broken heel bone.
- Cracked ankle.
- Rubbing the heel.
- The sole in the heel area has sunk in, what can you do about it?.
- The outer arch of the foot hurts, why.
- Loss of a blister on the heel.
- Feet of teenagers.
- Heel abrasions from new shoes, how to treat them.
