Liposarcoma is a malignant soft tissue tumor that develops from fatty tissue cells. Liposarcoma usually grows very slowly. The symptoms depend on the location: The tumor can e.g. B. lie on the thighs, back and stomach area.

- Skin cancer: symptoms
- Which skin growths should raise suspicion?
- A little about sacrum pain
- causes
- How a CT scan with contrast medium is performed
- Contraindications for contrast-enhanced CT examination
- disc prolapse
- Causes of lower back pain
- Liposarcoma – Diagnosis
- Liposarcoma – treatment
- How long does tramadol last?
- How long does the substance remain in the blood?
- How long it remains in the urine
- Effects of tramadol
- Tramadol in combination with alcohol
- Psychological effects of tramadol
- Hallucinations after tramadol
- symptoms
- Treatment
- contraindications
- Preparation
Skin cancer: symptoms
Head of the Department of Oncology at the Ichilov Clinic.
How to get remote skin cancer treatment in Israel during coronavirus outbreak?
Skin cancer, including melanoma, is very treatable in its early stages. The most important thing is to recognize the signs of pathology in a timely manner and start treatment. It is extremely important to properly identify a new growth on the skin that could potentially be cancerous. Early detection of skin cancer can significantly increase the chances of recovery.
Which skin growths should raise suspicion?
Most birthmarks, brown spots and skin growths are harmless - but not always. If you have a lot of moles and freckles, you need to be very careful when the pigmentation changes. When a birthmark starts to bleed or Liquid leaks.you should see a dermatologist.
New growths on the skin should also be observed. Many skin cancers are essentially colorless. They are often pink or pearly papules or scaly patches. These are signs of primary cancer and it is advisable to show them to the doctor. Bleeding and weeping skin growths are particularly worrisome.
A little about sacrum pain
Evolutionarily speaking, lower back pain, including sacrum pain, is the price of humans' ability to walk upright and have their arms free. In an adult human, the sacrum is a fairly large bone located almost at the bottom of the spine, in front of the tailbone. It is connected above to the last lumbar vertebra and below to the first vertebra of the coccyx. The sacral part of the spine is located between the two bones of the pelvis.
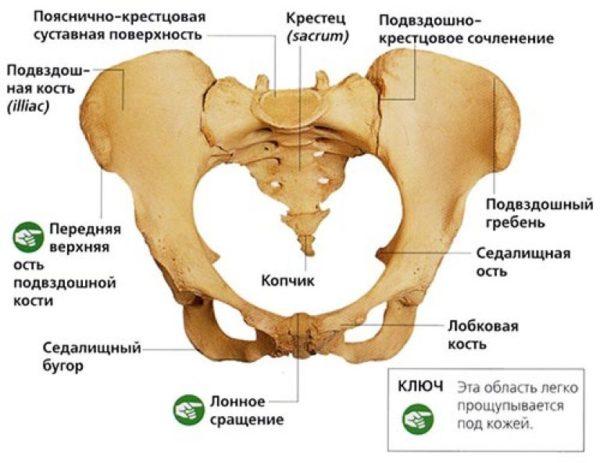
Danger!!! If the sacral region of the back hurts when sitting, the pathology that caused it may be actively developing and a visit to the doctor should not be postponed.
Any kind of pain whether he chronic or acuteIf they appear in the sacrum area, a person of any gender, especially women, should be alerted immediately. Pain in this part of the body is not always a sign of problems with the spine. Sacrodynia is a type of pain that occurs when a pathological process develops in the pelvic region. It is therefore a symptomatic pain that is not directly related to problems with the musculoskeletal system. In any case, the pain syndrome itself is not an independent condition, but always the consequence of a specific pathology.
Sacroiliac pain is not common. However, it is usually quite intense and increases when you lift weights, raise your body quickly, or bend forward. And this symptom is rarely specific to a spinal disease. Problems with other organs are usually the cause.
causes
There are many causes of sacral spine pain. In general, they can be divided into two main categories: pain related to spinal diseases and pain due to diseases of other organs.
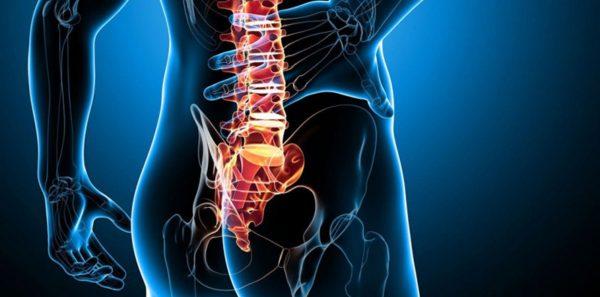
Tabel. Causes of sacroiliac pain in women.
| Diseases related to the spine | Diseases related to other organs |
|---|---|
| Spinal diseases, compressed spinal roots, displacement of vertebrae or intervertebral discs, trauma, age-related changes. | Kidney diseases, gynecological diseases, metabolic disorders, muscle sprains or strains. |
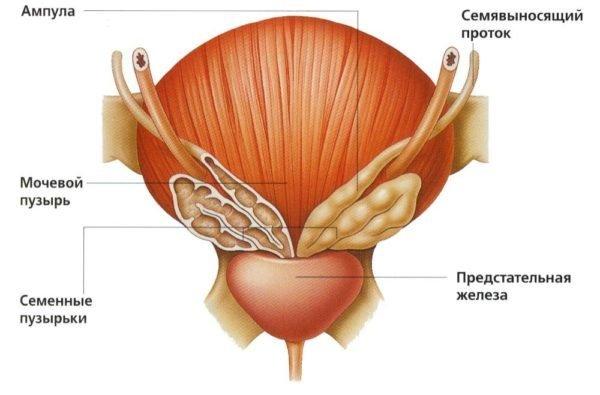
Sacral pain can occur in both sexes. However, in men it is often related to spine or prostate problems, while in women sacroiliac pain can occur due to a number of other problems.
How a CT scan with contrast medium is performed
Aside from inserting the catheter into the vein, the procedure is painless.
Modern clinics use bolus injection of the dye, in which the dye is injected into the vein automatically and at the appropriate speed using a pump injector. This method provides optimal contrast phases for various targets and tasks in the brain, kidneys, liver and other organs.
The dynamic bolus technique has several advantages:
- better representation of internal structures;
- lower risk of extravasation (rupture of the vein and penetration of the medication into the surrounding tissue);
- the possibility of quick scanning of the entire body.
Contrast-enhanced CT scanning is a standard procedure:
- the patient completes a questionnaire to identify contraindications and is admitted to the examination room;
- The X-ray technician places the patient on the extendable table and shows him the position of the panic button for communication with the nursing staff
- The nurse inserts the catheter into the vein and connects the autoinjector;
- At the operator's instruction, a native examination is performed;
- After evaluating the unamplified images, the doctor selects the scanning phases and the corresponding modes depending on the abnormalities detected;
- After the contrast medium has entered the vein, a certain period of time must be waited for the preparation to spread throughout the vascular bed;
- Another series of images is taken.
There is no pain during the CT scan with contrast medium. The nursing staff observes the person's condition from an adjoining room through the secure X-ray glass.
The time required varies: For example, a contrast-enhanced CT examination of the joints takes 25-30 minutes, a CT examination of the biliary tract or a urography takes around an hour.
Contraindications for contrast-enhanced CT examination
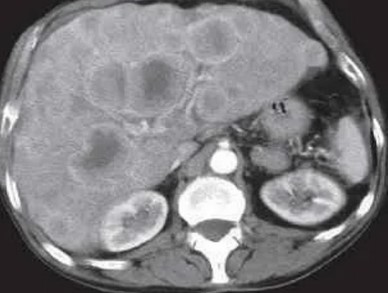
CT examination is the leading examination for liver metastases
- Thyroid diseases associated with excessive hormone production
- Renal failure at any stage, severe cardiovascular disorders, liver;
- Allergy to seafood, iodine.
People at risk with potentially expected effects - patients over 75 years old, patients with gout, severe bronchial asthma, multiple hypersensitivity reactions, a history of acute renal failure, patients taking nephrotoxic drugs - may require special preparation in the hospital.
Alcohol must not be consumed before the test: ethanol increases the nephrotoxic effect.
The use of an index drug in young children is acceptable in the hospital setting to assess vital signs. A contrast-enhanced CT scan in a child can be performed on an outpatient basis once the child turns 12 years old if referred by a doctor.
Patients taking metformin to normalize blood sugar levels must stop taking the drug 48 hours before the contrast-enhanced CT scan (in consultation with the endocrinologist).
During breastfeeding, the woman should give breast milk 3-4 times and perform decompression: the damage caused by the dye will be completely neutralized after 10-12 hours.
disc prolapse
A herniated disc is an equally common cause, the clinical sign of which is pain in the lumbosacral region of the back. The intervertebral disc (inner nucleus pulposus) loses its elasticity and flexibility with prolonged exposure and increasing age.
With prolonged stress (excess weight, trauma, progressive osteoporosis), the fibrous ring of the intervertebral disc becomes thinner and cavities form in it. These weak points in the fibrous ring allow the nucleus pulposus of the intervertebral disc to move and even bulge.
Causes of lower back pain
Back pain is such a non-specific symptom that it can be caused by many different causes. Depending on how intense and severe the pain in the lower back is, whether it occurs constantly or intermittently, primary or secondary, there may also be a cause:
- osteomyelitis;
- Ankylosing spondylitis;
- deformed spondylosis;
- Growth diseases – scoliosis;
- Infectious lesions of the intervertebral discs and vertebrae (epidural abscess, spinal tuberculosis, brucellosis);
- Metabolic bone diseases - osteomalacia, osteoporosis;
- Primary and metastatic tumors of the spinal cord, vertebrae and retroperitoneal space;
- Non-infectious inflammatory diseases - rheumatoid arthritis, Reiter's syndrome, ankylosing spondylitis;
- kidney tumors;
- Atherosclerosis of the abdominal aorta and its branches
- spondyloarthritis;
- hip joint abnormalities;
- Epidural inflammation of the spine;
- Lumbar disc protrusion;
- osteochondrosis of the spine;
- Acute disc prolapse;
- Intestinal obstruction, atypical course of acute appendicitis;
- urolithiasis;
- Acute dislocations, vertebral fractures;
- lumbago, sciatica;
- Acute circulatory disorders of the spine - stroke;
- Acute pyelonephritis.
Irritating pain in certain diseases of the internal organs:
- Diseases of the abdominal organs. In women – inflammatory processes of the uterine appendages, endometriosis, uterine cancer, ovarian cancer, sexually transmitted diseases (chlamydia, ureaplasmosis, gonorrhea, trichomoniasis, etc.) In men – prostatitis, prostate cancer;
- Diseases of the stomach, pancreas, duodenum, gallbladder;
- Intestinal diseases - diverticulitis, nonspecific ulcerative colitis, intestinal tumors;
- Kidney diseases - renal colic, kidney stones;
- Abdominal aortic aneurysm.
Liposarcoma – Diagnosis
Patients with various types of tumors under the skin often wonder how to diagnose liposarcoma. The examination alone is not enough to make the diagnosis because the tumor is very similar to a definite lipoma. Therefore, the dermatologist primarily prescribes an MRI scan to determine the quality of the tumor.
This examination is possible, among other things, if a liposarcoma is suspected, but the diagnosis must be clarified by a histopathological examination to detect tumor cells. Above all, histopathology makes it possible to accurately determine whether the lesion described during the examination is a liposarcoma or a lipoma. In addition, microscopic examination allows the diagnosis of a specific type of tumor, e.g. B. from liposarcomas and myxoids.
Knowing the type of lesion is important to determine the patient's prognosis for healing. The material for histopathological examination is obtained through a biopsy.
Liposarcoma – treatment
Surgery plays an important role in the treatment of liposarcoma. Patients who develop cancer in the hip, for example, often fear having to amputate the entire limb. Unfortunately, this risk exists, but amputations are usually only carried out if it is the last possible solution. If possible, conservative treatments will be considered first.
The main aim of treating these lesions is to remove them completely while preserving the reserves of healthy tissue.
In addition to surgery, radiation and chemotherapy are also used. These are particularly useful if the patient's existing cancer has invaded important structures such as large blood vessels, meaning that complete removal of the tumor is not possible. In this case, radiation therapy is effective. If the patient has formed multiple metastases, chemotherapy becomes the main treatment.
How long does tramadol last?
The half-life of the drug is 6-7 hours. The active ingredient is eliminated from the body after 3 days. Most of the substance (about 90 %) is excreted via the kidneys; 10 % are excreted via the gastrointestinal tract.
How long does the substance remain in the blood?
The toxic substance can be detected in the blood within 1-2 days.
How long it remains in the urine
The drug's metabolites can remain in the urine for up to three days. A comprehensive detoxification program is initiated to accelerate the elimination of the drug from the body.

Effects of tramadol
Tramadol has numerous side effects that pose a serious threat to human life and health. It is a powerful drug and its long-term use is strictly prohibited.
Tramadol in combination with alcohol
Taking tramadol and similar analgesic opioids with alcohol is strictly contraindicated. Otherwise, severe symptoms of poisoning will occur, leading to jaundice. Alcohol in combination with the active ingredient causes respiratory depression. This condition poses a serious threat to human life and health. Irregular and interrupted breathing can lead to the death of the patient.
Psychological effects of tramadol
Tramadol has serious psychological side effects. Long-term use of the narcotic painkiller leads to dependence, not only physically but also psychologically. The addicted person begins to view tramadol as the main sedative and the range of interests gradually narrows.
Addiction causes psychological reactions such as:
- Major depression;
- Schizophrenia;
- anxiety states;
- Sleep disorders;
- suicide attempts;
- Development of personality disorders.
Anyone who becomes addicted to drugs struggles with the urge to use drugs for the rest of their lives. Avoid irrational use of medicines: Fleeting weakness and hope for happiness lead to irreversible changes in physical and mental health.
Hallucinations after tramadol
According to former drug addicts, the systematic use of tramadol leads to the development of hallucinations. Often during seizures the person sees terrible things that trigger panic. Sometimes such attacks lead to irreversible consequences: the addict is able to make an unconscious attempt at suicide, he inflicts serious injuries on himself. As a result, the person may end up in a psychiatric hospital or intensive care unit in serious condition.
symptoms
Erythema annulare causes different symptoms depending on its clinical form. We describe some of these symptoms.
- Erythema multiforme – In response to an allergic substance (food, medicine). The spots are red, there is no desquamation and the course is quite mild (the lesions disappear within a few days). In contrast to simple erythema, persistent erythema is long-lasting.
- Scaly form – A resulting red spot will soon begin to peel. Some pigmentation is visible in the center of the redness, the color gradually fades. The spots reach a considerable size of up to 20 cm. The lesion remains largely unchanged in the center and grows in the periphery. This form can take several months to develop. After the rash clears up, the skin is pigmented. Recurrences are common, and strange patterns (hyperpigmented patches) form on the skin over the years. The cause of the psoriatic form is often helminth infections and tumors.
- Erythema darius centrifugalis – Erythema annulare – The etiology is unclear (viral, bacterial and fungal pathogens cannot, however, be excluded). It is characterized by the appearance of numerous small pink spots that rise slightly above the skin. The spots tend to enlarge and change shape. A characteristic feature of erythema darius is the circular shape of the lesions. They mainly occur on the trunk, less often on the face.
- Another form of centrifugal annular erythema is a rare form of lupus, an autoimmune disease. The redness appears to spread from the center of the face to the edges without causing any physical discomfort. It occurs as an independent disease (erythema Bietta of the rings) or as a symptom of another disease.
Main symptoms of erythema annulare
- Characterized by pink or red spots on the skin.
- The erythema in the center is almost normal in color or may be pale.
- Itching is not always present, which can sometimes be burning.
- Belly, flanks, arms and sometimes the face (cheeks).
- The spots can grow quite quickly, up to 20 cm in diameter. If several spots are in close proximity to one another, coalescence occurs.
- They then lift easily from the skin.
- Over time, a 'pattern' of old and new lesions forms on the body.
- In the garland type, the spots only appear for a short time, in the vesicular type (vesicles are small bubbles) they appear immediately and disappear just as quickly, in the exfoliative type the spots peel off towards the outside.
Treatment
Making a correct diagnosis is not an easy task. Therefore, the doctor prescribes a number of methods to clarify and confirm the form of the disease. Before the diagnosis is made, an examination of the affected area is carried out and the patient is interviewed.
- blood tests;
- serological methods – these indicate the presence and level of antibodies against the bacterial/viral source of the disease;
- Allergy testing – this can be used to determine whether an allergen is present;
- If the spots secrete fluid (exudate), this will be removed for examination;
- Differentiation from symptomatically similar diseases: toxoderma, mycosis fungoides, lupus, leprosy.
The success of treatment depends on the possibility of eliminating the cause of erythema annulare. For this purpose, the doctor prescribes the following systemic drugs:
- medications to treat the underlying disease (antimicrobial medications);
- Hyposensitizers – they are used in the treatment of skin diseases and reduce sensitivity to the allergy pathogen. This group includes preparations of calcium and sodium thiosulfate;
- Antiallergic drugs – relieve itching and peeling skin areas;
- Cytostatics – slow tumor growth and relieve symptoms of autoimmune diseases;
- Helminthiasis treatment – prescribed to people diagnosed with worms. Sometimes more than one treatment is needed to get rid of the worms;
- Glucocorticoids – broad-spectrum hormonal steroids that help to quickly eliminate the symptoms of the disease and have anti-inflammatory, anti-allergic and immunoregulatory effects.
The above groups of drugs are administered orally and are intended to treat both the underlying cause of the disease and the external symptoms on the skin. Treatment of erythema annulare also includes medications applied topically to the affected skin areas:
- Antihistamine ointments, gels and creams – relieve itching and redness and are very effective for allergic erythema annulare;
- zinc-containing ointments – help relieve itching, flaking and inflammation;
- Steroid ointments and creams – slow the growth of the spots, reduce their external appearance (itching) and improve the complexion.
contraindications
X-ray examination is an examination for which there are few contraindications. The biggest potential risk is the X-rays, which can have harmful effects on the body. But even in everyday life, radiation exposure cannot be completely avoided - we have to deal with radiation from devices in our environment, the earth's magnetic field and cosmic radiation from space. There are values that are considered partially safe for people. During an X-ray examination, the doctor knows what radiation dose the patient is receiving and ensures that it does not exceed a safe level. There is no reason to worry about the possible dangers of X-rays - several dozen X-rays can be taken in adults and three in children per year. However, old, analog devices are used. Modern medical centers are equipped with new digital cameras that emit less radiation. Therefore, the examination cannot cause any harm. Treatment without an accurate diagnosis and understanding of the problem can only worsen the condition.
Pregnant women and children under 14 in particular need to be careful. However, for bone fractures and other emergencies, x-rays are performed at the doctor's discretion. A protective apron is worn to protect the internal organs of the abdomen and chest.
Preparation
X-rays of the feet can be taken without any preparation. It is sufficient to take off your shoes and, if necessary, your jewelry at the examination site.
Foot x-rays are usually performed in two projections:
- Simple – this is carried out for various bone and joint diseases and injuries. The foot is placed directly on the camera's recording device. In such a picture, the heel and tarsal bones, the lower part of the shinbone and the ankle joint can be clearly seen.
- Laterally - in this photo, in addition to deformations, fractures and pathological changes, the longitudinal flatfoot can also be seen. The patient turns his leg sideways towards the camera.
X-ray of the foot in oblique projection - at an angle of 45 0 - is used less often. It is useful in diagnosing the forefoot, which may not be in the image area of the straight or lateral projection.
X-ray examinations of the foot in two projections are carried out while lying or sitting. The leg is held in place to prevent movement and blurry images.
Depending on the suspected diagnosis, the doctor may also recommend a stress x-ray. In this case, an X-ray of the foot is also taken in 2 projections, but with the foot standing and with the body weight pressed downwards. The X-ray under stress is the most informative for flat feet and makes it possible to assess the type and degree of deformity as well as the dynamics of its progression.
The images are evaluated by a radiologist who prepares a written report describing the anomalies detected and their characteristics (location, size, structure).
You can apply by selecting the department in your city
Read more:- Outer malleolus of the right tibia.
- Front lower leg area.
- foot pattern.
- Ankle strap at heel.
- Heel bone human anatomy photo and description.
- Photograph of a person's leg with a description.
- The structure of the human foot and diseases.
- foot of phot.
