If the inflammation is not acute, then it may not affect the general condition of the patient. Such patients often neglect the disease and try to cope with it themselves, as a result of which the acute process turns into a subacute one. A sign of chronification is a decrease in pain intensity.
- bursitis
- Causes of bursitis
- Classification of diseases associated with bursitis
- Symptoms of synovitis
- causes
- classification
- Treatment of ankle bursitis:
- COST OF TREATMENT
- How dangerous is self-medication
- Symptoms of bursitis (achillobursitis)
- complications
- Causes and development mechanisms
- classification
- Achillobursitis
- wrist ball
- Why SM Clinic?
- treatment of synovitis
- Types of knee bursitis
- Symptoms of popliteal bursitis
- Bunion Toe Symptoms
- causes
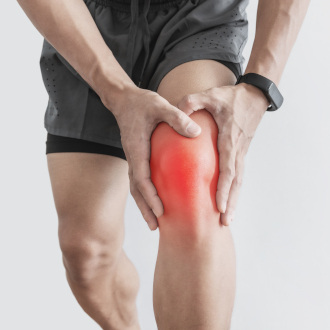
bursitis
Various diseases of the soft tissues surrounding the joint, e.g. B. bursitis, are a common reason for visiting a surgeon or trauma surgeon. In recent years, the frequency of this pathology has increased. It is often clearly work-related and leads to a loss of ability to work. At the Paramita Clinic in Moscow, this condition is effectively treated using a combination of traditional and unconventional methods.
Synovitis (bursitis) is inflammation of the joint capsule, which is part of the periarticular tissue complex. Inflammation can be acute, subacute, chronic and recurrent. The inflammatory process is accompanied by the secretion of inflammatory fluid, an exudate of various types: serous (inflammation without pus), purulent, hemorrhagic (with blood), purulent-hemorrhagic. It is accompanied by swelling, redness, pain and restricted joint mobility. Synovitis is more common in men and primarily affects the elbow, shoulder, and knee joints. The ICD10 codes for bursitis are M70.2 for elbow bursitis, M70.5 for knee bursitis and M70.7 for thigh bursitis.
The main functions of the bursa are cushioning and protection. The bursae are located in the soft tissues surrounding the joint and protect it from injury during movement. Most commonly, the bursae are located in areas where bony protrusions form as the joint moves. They are small, flat, elastic sacs filled with synovial fluid produced by the synovial membrane lining the interior of the bursa (the same membrane that lines the interior of the joint cavity). Bursae can be found in various soft tissue layers: under the skin, in fascia (connective tissue covering muscles, vessels and nerves), in muscles and tendons. Since the tendons are often attached to the inside of the joint, bursitis is related to the joint cavity.
Causes of bursitis
Inflammation can develop when a joint is exposed to a variety of factors. The most common causes include:
- Skin trauma and the penetration into the bursa of an opportunistic microflora (streptococci, staphylococci) living on the surface of the body; this pathology develops especially often in immunocompromised individuals;
- closed trauma can cause aseptic (infection-free) inflammation, but infection can enter the bursa from distant sites via the lymphatic and blood vessels (chronic tonsillitis, maxillitis, cholecystitis, etc.)
- possible development of the disease when a specific infection enters the bursa with the bloodstream, if the patient suffers from it – tuberculosis, brucellosis, gonococci, syphilis;
- Persistent micro-injuries of the joint in certain professional activities or sports; for this reason, some professionals consider synovitis an occupational disease;
- chronic joint diseases leading to salt deposits in the periarticular tissues - cystic fibrosis, rheumatoid arthritis, etc.
- Diabetes, AIDS, cancer after chemotherapy or radiation therapy - immunity is reduced and the risk of bursa after injury is increased;
- in chronic inflammatory joint diseases;
- whose profession involves constant micro-traumas on certain joints; miners - shoulder and elbow injuries, 'maid's knees' - knee bursitis from constant kneeling, etc;
- Athletes – footballers – knee injuries, tennis players – elbow and shoulder injuries.
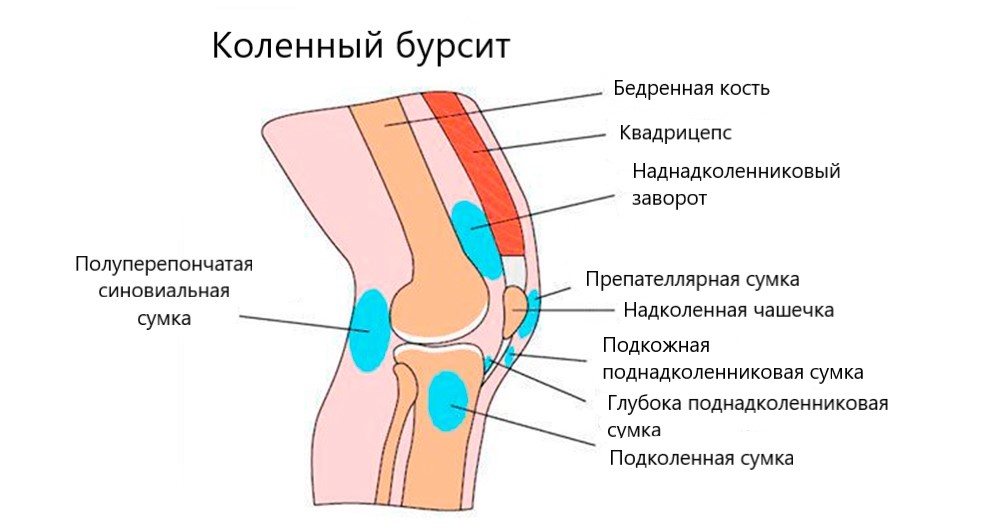
Classification of diseases associated with bursitis
- specific course (acute, subacute, chronic or recurrent);
- causative pathogen (specific or non-specific infection, inflammation without an infectious agent); and origin (primary or secondary synovitis)
- type of exudate (serous, purulent, hemorrhagic)
- Location .
Sudden and acute synovitis can be completely cured with early treatment. If the visit to the doctor is repeatedly delayed or if the doctor's recommendations are not followed, a transition to a chronic form is more likely. – In this case, the bunion persists for several months and then reappears, with irreversible consequences.
As a primary form, synovitis occurs when there is direct injury or local infection of the periarticular capsule. Secondary as a result of another chronic disease. The type of effusion can only be determined by taking a sample - this is the basis for treatment.
Symptoms of synovitis
Acute bursitis usually begins suddenly and is accompanied by:
- acute pain that increases with movement and can occur at any time of the day;
- soreness and tenderness of the skin over the joint;
- restriction of mobility;
- Hypersensitivity and swelling of the skin over the joint;
- local or general fever
- muscle weakness;
- Palpation of the joint may reveal a soft, fluid-filled nodule that feels like a water-filled balloon;
Most frequently. Symptoms of synovitis appear in the arms, Kneel, elbow and ankle jointsas well as Joints with heel tendon. Symptoms and treatment of synovitis depend on the severity of the inflammation. If left untreated, it can cause a rise in body temperature up to 40 °C due to the purulent process. At this stage, complications such as hardening of the subcutaneous fat are likely.
The symptoms of chronic synovitis are as follows
- The pains become weaker, tolerable or absent altogether;
- The swelling under the skin lasts for a long time;
- The movement is less stiff or there is no amplitude limitation at all.
The recurrent course is characterized by a combination of all symptoms of synovitis: the chronic course is interspersed with periodic exacerbations of symptoms.
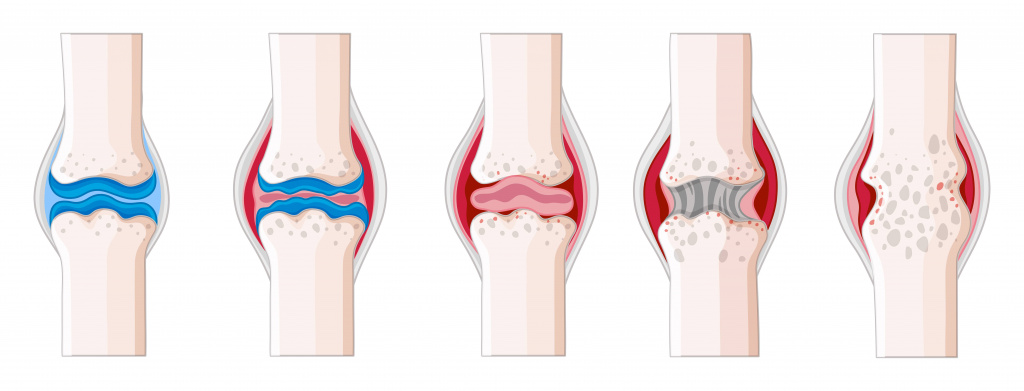
Fluid accumulation in the joint cavity is a common symptom of synovitis.
causes
In orthopedics and traumatology, a distinction is made between aseptic and infectious synovitis. Aseptic synovitis occurs without microorganisms and is a reaction of the synovial membrane to pathogenic stimuli. Infectious synovitis is caused by the invasion and multiplication of microorganisms in the joint cavity. Aseptic synovitis can be caused by trauma to the joint: bruise, dislocation, torn ligament, etc. Sometimes reactive aseptic synovitis is 'triggered' by an allergic reaction of the body.
In some cases, aseptic synovitis is caused by a constant irritating effect on the synovial membrane of a joint part, e.g. B. on the cartilage, which has lost its suppleness in osteoarthritis. Aseptic synovitis can be caused by endocrine disorders (eg, diabetes), neurogenic factors (neuritis, neuropathies), arthritis, hemophilia, static joint deformities, and congenital or acquired ligament weakness.
Infectious synovitis is caused by nonspecific or specific pathogens. Specific synovitis can be caused by tubercle bacilli, which is currently a very rare pathology. In the case of non-specific synovitis, the pathogens are usually staphylococci and streptococci, more rarely other bacteria. Infection enters the joint via contact, hematogenous (via blood vessels), or lymphatic.
Contact infections occur with abrasions, bruises, cuts or puncture wounds, closed hematomas, boils, abscesses or cellulitis in or on the joint. Hematogenous or lymphatic spread of infection can occur in some common infectious diseases and in the presence of distant foci of inflammation. Decreased immunity, exhaustion and weakness are predisposing factors.
classification
According to the features of the clinical course, acute and chronic synovitis are distinguished, taking into account the type of discharge (inflammatory fluid in the joint): serous, purulent, hemorrhagic and sticky (serous fibrin). In the case of serous inflammation, the discharge is liquid, clear and poor in cells; with hemorrhagic inflammation it is also liquid, but reddish or brownish; in a purulent inflammation it is cloudy, yellowish-greenish and foul-smelling. Adherent inflammation is characterized by a small amount of fibrin-rich fluid.
The patient suffering from acute aseptic synovitis experiences heaviness and (often persistent) pain in the joint area. With mild inflammation, the pain is minor and occurs mainly with movement. With severe synovitis, the patient feels pain and swelling even at rest. Mobility is restricted. Examination reveals a slight swelling of the soft tissues, smoothing of the contours and enlargement of the joint (the degree of enlargement depends on the amount of exudate). There may be slight redness and an increase in local temperature. There is hesitation on palpation.
The course of chronic aseptic synovitis is usually wavy, alternating phases of exacerbation with more or less long-lasting remissions. During remission, synovitis symptoms are absent or minimal, and the clinical picture depends on the underlying disease (e.g. arthrosis). With an exacerbation, the symptoms are similar to those of acute aseptic synovitis, although the details may vary depending on the type of inflammation.
Infectious synovitis is characterized by a sudden onset with moderate to severe pain and general signs of intoxication: fever, weakness, fatigue, headache, etc. The joint is swollen, enlarged, the skin over the joint is hyperemic, and the temperature is elevated. Movement is severely restricted by the pain and support is limited. Palpation of the joint is painful.
Treatment of ankle bursitis:
First, the foot should be given as much rest as possible. To this end, the foot is immobilized (fixed) with a cast splint for the duration of the exacerbation and independent movement is avoided. Non-steroidal anti-inflammatory drugs are always used to eliminate inflammation, swelling and pain. If a large amount of exudate has accumulated, it is removed by puncturing the bursa. Once the exudate is removed, steroids are injected into the joint cavity, which also have an anti-inflammatory effect. If the bursitis is purulent, a puncture and antibiotics are essential. As soon as the pain subsides, the pus is removed and the exudate dissolves, the treatment of synovitis of the foot can be supplemented with physiotherapeutic treatments (magnetic therapy, phonophoresis, UHF), as well as paraffin and medicinal mud. Surgery is indicated for chronic and severe Achilles tendonitis with a high risk of rupture.

COST OF TREATMENT
| General physiotherapy | 30 minutes | 4,000 rubles |
| Restoration of foot function and shape with Bauerfeind orthoses | Including examination with Stabilograph or Plantoscopy, advice on choosing the insoles, correction of the insoles | 8500 rubles |
| What is the difference between osteopathy and manual therapy? | Read the answer>>>> |
| Lorem ipsum dolor sit amet, consectetur adipisicing elit. Natus, provident harum non, voluptate place at quod! Nam aliquam maiores numquam, culpa asperiores at accusantium earum? Officia quas repellat, nam excepturi sapiente. Lorem ipsum dolor sit amet, consectetur adipisicing elit. Possimus omnis modi nobis dicta repudiandae, quo fugiat, aperiam, mollitia expedita animi nihil explicabo incidunt eius laborum tempore quae? Doloribus dolores, voluptate! | |
| How is the fluid circulation in the tissues optimized? | Read the answer>> |
| Lorem ipsum dolor sit amet, consectetur adipisicing elit. Natus, provident harum non, voluptate place at quod! Nam aliquam maiores numquam, culpa asperiores at accusantium earum? Officia quas repellat, nam excepturi sapiente. Lorem ipsum dolor sit amet, consectetur adipisicing elit. Possimus omnis modi nobis dicta repudiandae, quo fugiat, aperiam, mollitia expedita animi nihil explicabo incidunt eius laborum tempore quae? Doloribus dolores, voluptate! | |
How dangerous is self-medication
Self-medication is just as dangerous. Your doctor will be able to recognize the bunions by the smallest signs. To confirm the diagnosis, he will order an ultrasound scan, an X-ray or an MRI and will know exactly where the inflammatory process is located. The doctor will then prescribe treatment for the acute bursitis, which may include:
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) – Ibuprofen, Dexalgin, etc.; these drugs also have pain-relieving properties;
- In case of a purulent process, the doctor punctures the sac, removes the pus, flushes the cavity with antiseptics and prescribes antibiotics;
- With a pronounced inflammatory process, hormonal drugs are injected into the sac;
- prescribes physiotherapy treatments.
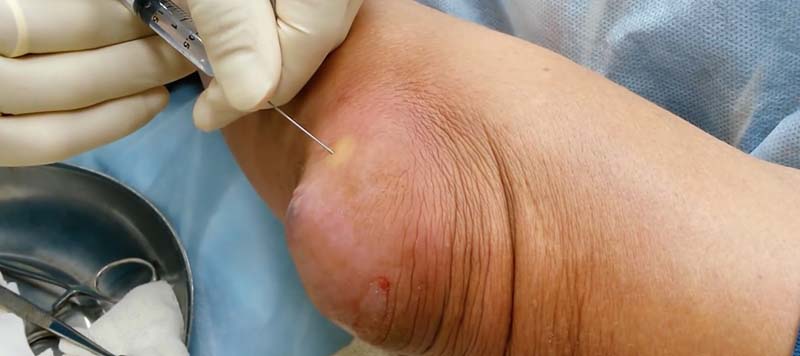
If all this is not done and treated with folk remedies at home, the risk of complications increases dramatically, the treatment of which is problematic even for a specialist doctor.
Acute bursitis rarely develops without chronic trauma to the joint. Pain in a joint requires immediate referral to an ambulance. If this is not done, the consequences can last a lifetime.
'You have thought about your own health and come to us - with this step. You have entrusted your life to us.. We appreciate your decision and I would like to assure you on behalf of the Paramita Clinic team that we will do everything to make it worthwhile.'
Symptoms of bursitis (achillobursitis)
Bursitis as a result of trauma or spreading infection develops acutely and affects one side. In the case of rheumatic diseases, the onset is insidious and bilateral involvement is possible. With strains, at first there is an acute attack, then the disease goes into a chronic course, sometimes the pathology is primarily chronic. Patients complain of wrist pain that increases with movement and shoe compression.
On examination, swelling and local hyperemia are noted. Initially, the swelling is small and limited. The swelling then increases and there is a thickening in the lower third of the tibia. Anterior Achilles bursitis is characterized by a fusiform swelling with thickenings on either side of the Achilles tendon. If the posterior capsule is affected, a soft, round, or oblong mass is visible over the tendon.
On palpation of the posterior capsule of the Achilles tendon, a stabbing pain is noted under the tendon, anteriorly in the superficial tissues. The affected area is soft and elastic, and the fluctuation sign is positive. With aseptic inflammation, the skin temperature in the affected area is slightly increased. When infected, there is significant local hyperthermia with an increase in overall body temperature, redness spreads to surrounding tissues, pain increases, and cramps appear, depriving nightly sleep.
complications
In a chronic course, the probability of an Achilles tendon rupture increases significantly. With infectious Achilles tendonitis, there is a risk that the purulent process will spread to the surrounding tissue and an abscess or mucus will form. Dangerous complications are inflammation of the heel bone and purulent inflammation of the ankle. In individual cases, generalization with septicemia is also possible.
The diagnosis is usually made by an orthopedic surgeon. Diagnosis is made by a rheumatologist when there is a previously diagnosed rheumatic disease and by a surgeon when there is evidence of purulent inflammation. The following procedures are used to determine the cause, type, and progression of achillobursitis:
- anamnese. The doctor inquires about the dynamics of the disease, the circumstances that preceded the onset of symptoms (trauma, overload), occupational characteristics, the presence of diseases of the joints and periarticular tissues.
- Investigation. Objective examination reveals pain, local thickening of the bursa area, congestion, overheating. Maximum sensitivity on palpation of the soft tissues and not the bony structures, limited edema in a typical form suggest achillobursitis.
- Ultrasound examination of the tendon. Examination of the tendon and surrounding tissue can reveal signs of inflammation. In chronic achillobursitis, there are areas of fibrous degeneration of the bursa wall, sometimes with calcifications, and the tendon is degenerative.
- MRI of the ankle. Layered imaging of the affected area allows for an accurate determination of the location of the inflammatory process, as well as the nature and extent of changes in the tendon and peroneal tendon capsule.
- X-rays of the ankle. In the case of soft tissue involvement, this technique is not very informative and is recommended to rule out traumatic or inflammatory ankle arthritis and to clarify the causes of achillobursitis.
- laboratory tests. If the process is purulent, then inflammatory markers - increased blood sedimentation, leukocytosis with a left shift - are examined. Examination of urea, C-reactive protein, rheumatoid factor, anticytokine antibodies and other indicators can confirm or refute the rheumatic etiology of achillobursitis.
Causes and development mechanisms
Synovitis of the foot and ankle joints develops as a result of the following causes:
- Acute injuries - impacts with soft tissue injuries, fractures, dislocations, sprains, etc.;
- Long-term micro-injuries in:
- Long-term micro-injuries during:
- Professional or sporting activity; Achilles bursitis is more common in runners, hamstring bursitis in jumpers and dancers;
- Various orthopedic pathologies – flatfoot, clubfoot, etc;
- overweight.
- aging, thinning of the ligaments and tendons that support the foot;
- inflammatory and degenerative joint diseases - arthritis and arthrosis;
- Spine diseases – osteochondrosis and postural defects;
- Metabolic disorders with salt deposits in the bursa (e.g. urate in gout);
- wearing uncomfortable, tight, high-heeled shoes.
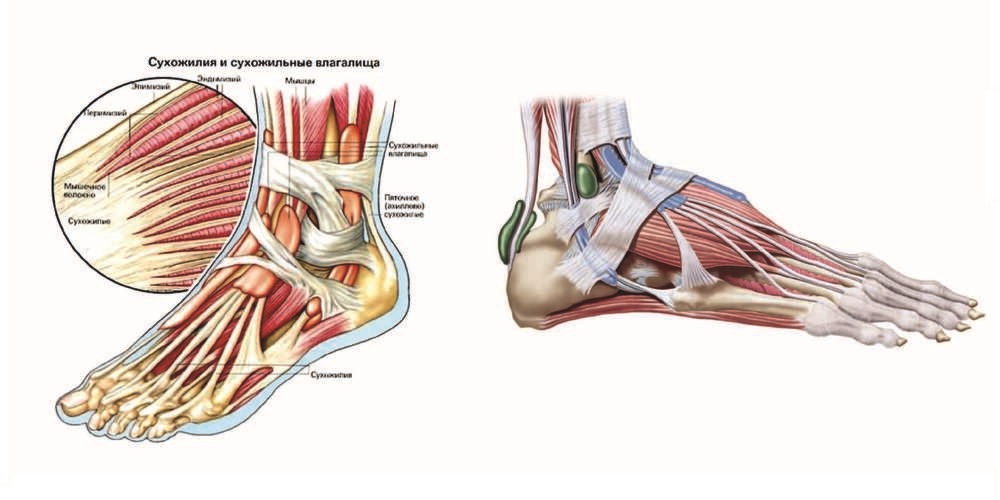
Various factors cause the bursa to become inflamed and the volume of inflammatory fluid to increase. The bursa enlarges and can be seen on examination as a protruding, elastic, painful mass. When there is compression of the surrounding tissue, including nerve endings, the pain can be significant, especially severe in upper arm bursitis. Initially, the inflammation is aseptic, but the foot is often traumatized, small wounds, blisters are formed, through which the infection can spread, the process becomes purulent, and the patient needs urgent surgery.
classification
All osteoarthritis of the ankle and foot are classified according to different parameters.
Even mild symptoms of ankle bursitis need to be treated appropriately to avoid complications. Consult your doctor and do not delay treatment!
The disease can be mild and unremarkable, but can also become recurrent or purulent. The course depends on the location of the affected bursa and the cause of the disease.
Achillobursitis
The inflammation originates in the subcutaneous bursa, which is located on the back of the heel bone at the insertion point of the Achilles tendon. The main cause is constant injury to the tendon and bursa while running. It also occurs in older and overweight people and can be asymptomatic for years before eventually manifesting as pain.
Symptoms: Pain in the area behind the heel that radiates up to the back of the shin. Walking is painful, but running is even more painful. On examination, there is a resilient, thick, round, painful bulge just above the heel. If the heel ball is treated when the first symptoms appear, complete healing is guaranteed. A chronic course requires long-term conservative treatment.
wrist ball
This type of condition originates in the bursa on the underside of the heel bone. Heel bunions do not develop spontaneously, but are usually associated with various orthopedic disorders (especially heel spurs) and long-term microtrauma while running, jumping, or walking. As a result, the wide plantar fascia is constantly traumatized and irritated, and an inflammation develops in it - the fasciitis. In some areas, the fibers of the plantar fascia are torn. There are many nerve endings in this area, so fasciitis is painful and the inflammation almost always spreads to the bursa.
Calf spurs can be not only a cause, but also a complication of fasciitis and heel bursitis. It is the result of constant irritation of the fibula bones, leading to an overgrowth of bone tissue, creating osteophytes - bony outgrowths or spurs.
Why SM Clinic?
Diagnosis begins with a conversation with the doctor and an objective examination, during which characteristic clinical signs are identified. If there is a suspicion of a specific process, a puncture is performed; the fluid obtained is sent for testing and the blood is tested for antibodies (serological reactions).
If there is a suspicion of deep capsular inflammation that cannot be felt during a routine examination, an x-ray or MRI of the joint is ordered.
The doctor will not only analyze the specific clinical picture, but will also ask about the medications that the patient is taking. Some blood-thinning medications, if taken in excess, can cause blood to leak into the joint (hemarthrosis), which resembles a bunion. A thorough differential diagnosis is required, which can only be performed by a specialist doctor.
treatment of synovitis
Treatment can be conservative or surgical.
The extent of treatment depends on the clinical picture.
In mild cases, local treatment—rest, a restrictive joint bandage, and anti-inflammatory compresses—is sufficient.
If there is a disease that leads to salt deposits in the joints, the treatment aims to improve the general condition. In addition, a number of nonsteroidal anti-inflammatory drugs are prescribed to relieve pain and reabsorb pathological fluid.
The treatment of specific bursitis - tuberculous or syphilitic - is carried out in a hospital with the appropriate profile.
Types of knee bursitis
Depending on the type of inflammatory process, there are three main types of bursitis in the knee:
- Acute disease characterized by the development of an active inflammatory response;
- Chronic course, in which phases of aggravation alternate with phases of remission (the inflammatory process can be activated by general and local hypothermia, concomitant pathologies, etc.).
- The subacute course, which lies between the two forms described above.
Depending on the type of inflammatory process, 4 forms of the disease are distinguished:
- serous - this is usually the initial stage when the inflammatory discharge consists of plasma and also contains a small part of the cellular component;
- purulent – develops when the pathological process progresses further and leads to the death of microorganisms and protective immune cells (the pus also contains dead cells of the affected organ);
- hemorrhagic - there is a particularly high proportion of red blood cells in the excreted plasma (the exudate may have a reddish-violet tint);
- fibrinous - characterized by a high fibrin content.
The fibrinous form is usually characterized by chronic inflammation in the area of the bursa.
Depending on the localization of the pathological process, the following types are distinguished:
- prepatellar bursitis;
- Infrapatellar bursitis with deep and superficial localization;
- suprapatellar bursitis;
- infrapatellar bursitis (anserin bursitis);
- Baker's cyst.
Symptoms of popliteal bursitis
The main objective symptom of popliteal bursitis is a round, tight, elastic swelling of the movable joint. This localized swelling is painful to the touch, and the skin over it may feel hot. The swelling is variable, that is, with pressure, receding surges of fluid are felt.
The main clinical sign of patellar inflammation is a pain syndrome. The pain can vary in intensity from mild to severe. The pain is present at rest and increases with movement.
Depending on the location of the swelling, the doctor can determine which knee joint capsule is affected by the inflammation:
- Swelling in the popliteal fossa is characteristic of an inflammatory lesion of the hemispherical capsule (this process is also called Baker's cyst; sometimes the inflammatory swelling can acquire very large proportions and pass from the knee to the lower leg);
- local swelling in the area of the kneecap indicates inflammation of the kneecap capsule;
- An inflammatory bilateral (lateral and medial) bulge around the patellar ligament is a sign of infrapatellar bursitis.
Inflammation of the tendons of the three muscles that attach to the tibia leads to infrapatellar bursitis (the infrapatellar bursa is formed by these three tendons). Limited swelling is rare with this inflammatory process. The main symptoms of this condition are pain on exertion and local pain when palpating the lower part of the knee.
In most cases, acute bursitis resolves within one and a half to two weeks. However, sometimes the inflammatory process passes into a purulent stage. This is due to the presence of a pus-like organism. If medical treatment is delayed, the pus quickly spreads to the surrounding tissues, partial or complete necrosis of the tissues of the inflamed capsule occurs, phlegmatic foci form under the skin and between the muscles. The clinical picture in this situation is particularly pronounced and severe. The following symptoms are present:
Bunion Toe Symptoms
Symptoms of a bunion toe can include
- pain in the area of \u200b\u200bthe inflamed capsule;
- redness and swelling of the skin over the inflamed capsule;
- Localized increase in skin temperature.
In the initial phase, the pain only occurs after walking for a long time or wearing non-ergonomic footwear for a long time. In the later phase, the pain can also occur at rest, including during night sleep, leading to insomnia. With ankle bursitis, the pain is particularly severe when the patient tries to stand on their toes.
The clinical presentation depends on the location of the inflamed capsule. During visual examination, not only the symptoms of bursitis are often detected, but also predisposing factors in the form of foot deformity. Bursitis of the first metatarsophalangeal joint, for example, bunions on the inside of the foot and corns, where the skin is exposed to excessive pressure, are found. In severe cases, the first toe drags over the second toe, indicating a severe deformity.
causes
Inflammation of one or more synovial capsules in the foot is most commonly caused by repetitive injury to the joint capsule. Predisposing factors increase the likelihood of developing the condition. This may include the following conditions:
- the presence of a foot deformity – most commonly a valgus big toe, heel spur, flatfoot or clubfoot;
- concomitant acquired diseases of the musculoskeletal system (plantar fasciitis);
- Repeated foot injuries, including those related to sports (long jump, athletics, etc.);
- Obesity, which increases the load on the joints and periarticular tissues;
- Biological aging, which provokes dystrophic processes in many tissues (bunions in women can often be associated with the onset of menopause);
- thinning of the subcutaneous fatty tissue where the joint capsules are located under the skin;
- Deforming arthrosis of the medium and small joints of the lower limbs;
- Wearing compression shoes that have a mechanically unfavorable effect on the musculoskeletal system of the foot;
- Pathology of the spine, which increases the load on the feet;
- Metabolic and autoimmune disorders in the body.
- Heel bone tendon sac in Latin.
- heel strike hurts.
- Ligament inflammation in the ankle.
- ligaments in the ankle.
- Structure of the heel.
- Ligament damage in the right ankle.
- ligaments in the ankle.
- heel joint.
